Oral cancer has a five-year survival rate of only 50%. A patient's best chance of surviving is early detection. While a number of methods and new technologies are now available to enhance early detection, the panel is still out on whether there is any one best approach for detecting oral cancer.
As we report this week, questions have been raised about the ADA's heavily promoted oral cancer campaign, which prominently features the BrushTest made by OralCDx Laboratories. Mark Lingen, D.D.S., Ph.D., a University of Chicago associate professor of pathology, has been among the most prominent critics of the campaign. So when he outlined his approach to detecting oral cancer at a recent meeting of the California Dental Association, an avid crowd showed up to listen.
"About 10% of all patients have some sort of oral mucosal abnormality," Dr. Lingen noted. Because it is extremely difficult to tell premalignant lesions apart from the harmless ones, the deadly disease often goes unnoticed until it is advanced and thus much harder to treat.
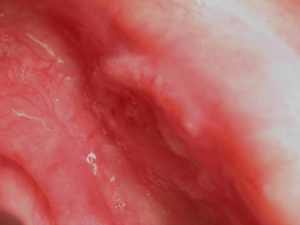
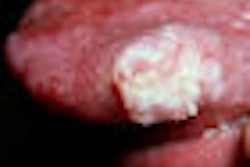
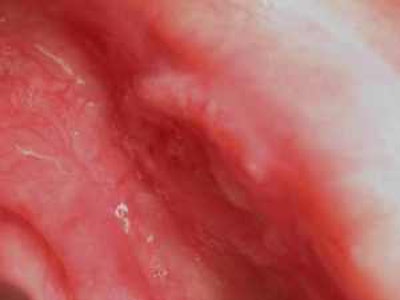
Oral cancer is indicated through two kinds of tumors: leukoplakia (white lesions) and erythroplakia (red lesions). Five percent to 25% of leukoplakias and 90% of erythroplakias have histological evidence of premalignancy when dentists see them.
It is important to keep in mind that not all white and red lesions are premalignant, Dr. Lingen explained. And the size of the lesion won't give you a significant clue.
His take-home message: If your patient has a white or red patch and you cannot figure out why it's there, it could be precancerous or cancerous. After seeing this lesion in a patient's mouth, a dentist usually has a 10 to 14-day window to check if it has subsided. If it hasn't subsided in that time, he said, do a scalpel biopsy.
Some common areas to look for lesions are:
- Floor of mouth
- Ventral surface of tongue
- Retromolar trigone region
- Soft palate
Less common areas include:
- Gingiva
- Buccal mucosa
- Hard palate
"I don't care how you get there -- tongue depressors, mirrors. The floor of the mouth is a very common place to get oral cancer. Examine it thoroughly," Dr. Lingen said.
Another area to check is the ventral surface of the tongue. Dr. Lingen showed a picture of a clinician using a piece of wet gauze to extend the patient's tongue.
"The most common location for oral cancer of the tongue is the posterior aspect of the anterior tongue," he said. "To get a good look at this region, you have to pull the patient's tongue out."
Another compelling reason to conduct a thorough exam is that dental-related malpractice suits associated with oral cancer are on the rise. Here are a few scenarios in which the cases are deemed indefensible:
- Failure to biopsy.
- Failure to re-examine a lesion. If you have a patient with a lesion, you need the patient to come back in 10 to 14 days to make sure the lesion is healing. If he or she comes back and the lesion is still there or has become worse, you need to biopsy.
- Failure to follow up on diagnostic report.
Diagnostic devices
A number of devices now on the market are designed to enhance early detection of oral cancer, including:
- The BrushTest (OralCDx)
- Toluidine blue staining
- ViziLite Plus (Zila)
- Microlux (AdDent)
- VELscope (LED Dental)
Here are the key advantages and disadvantages of each, according to Dr. Lingen:
The BrushTest
Dentists can use the BrushTest to collect cells from white or red lesions and send them to a lab for diagnosis. If the cells are abnormal, a biopsy will determine if the spot is potentially cancerous. You can get back three possible results: positive, negative, and atypical. If the result is atypical or positive, a scalpel biopsy is mandatory.
If the results are negative (and nothing else causes concern), then simple follow-up is probably sufficient.
Advantages:
- FDA-approved.
- Useful in cases in which a patient has multiple lesions throughout the oral cavity because it's painful to have multiple scalpel biopsies.
- Useful for a noncompliant patient. If you see suspicious lesions and want to refer a patient for a scalpel biopsy, but are quite certain he or she won't comply, do the brush biopsy to check for positive or atypical results.
Disadvantages:
- Often used inappropriately by the dentist. For example, some use it on papillomas.
- Cells are seen out of context, which can result in misinterpretation. For example, if the BrushTest is used to collect cells from a patient who has lichen planus and the cells are spread out on a slide, they will be out of context and will be read as atypical.
"Don't brush biopsy everything that looks atypical," Dr. Lingen said. "You do that, and you will get back a lot of atypical results which you will then be obligated to scalpel biopsy."
Toluidine blue staining
This technology is not yet approved for use in the U.S. and is more common in Canada and the U.K. It is a liquid dye composed of tolonium chloride. Practitioners swab the blue dye onto suspicious oral lesions and look for ones that retain the blue dye, as they can be cancerous.
Advantages:
- May help to better define gross extent of areas of lesions. These fields can be as large as 6 cm in diameter. If you have a patient with a field that large, but only a centimeter is clinically evident, and you excise it, you will still be left with 5.5 cm of molecularly altered tissue that has the potential to become cancerous.
Disadvantages:
- Not FDA-approved.
- High rates of false positives and false negatives.
- Works well on erythroplakias but not on leukoplakias, which is where clinicians need more help.
- May be better than visual acuity but does not identify the true margins of the field.
ViziLite Plus and Microlux
These competing technologies are similar. For the ViziLite Plus test, the patient rinses for 30 to 60 seconds with a solution that contains 1% acetic acid, and then the dentist uses a disposable light device to examine the oral mucosa. Any abnormalities will appear acetowhite. They can then be marked using the TBlue marking system.
Microlux is the same technology, except that the light device used in this system is not disposable.
Advantages:
- FDA-approved.
- May be better to define areas with increased amounts of DNA.
- High degree of sensitivity.
Disadvantages:
- Low degree of specificity. It will light up things that are not premalignant.
- May be better than visual acuity but does not identify the true margins of the field.
VELscope
The VELscope is a handheld device that shines a light into the oral cavity, which excites the tissue and causes it to fluoresce. The clinician can view the different fluorescence responses to help differentiate between normal and abnormal tissue. Healthy tissue fluoresces green, while abnormal tissue does not fluoresce and may appear dark.
Advantages:
- May help to better define surgical margins.
- FDA-approved.
Disadvantages:
- Low specificity as described for ViziLite Plus and Microlux.
- May be better than visual acuity but does not identify the true margins of the field.