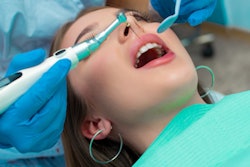
Controlling dental plaque after a patient has a stroke may be lifesaving, but the best way to do so is still unclear. A new study compared the results of oral hygiene instruction combined with different plaque control methods in stroke patients, among whom functional impairment is common.
The researchers found little difference in plaque reduction between individuals who used a power toothbrush with chlorhexidine gel and those who used a conventional manual toothbrush with a standard commercial toothpaste. Both methods were effective at initially reducing plaque, while other factors were linked to plaque levels at six months.
"This clinical trial demonstrated oral health promotion interventions are effective at reducing dental plaque among patients hospitalized following stroke," wrote the authors, adding that "these preliminary findings highlighted the importance of oral hygiene care among stroke survivors" (Journal of Oral Rehabilitation, November 23, 2017).
The lead study author was Normaliza Ab Malik, BDS, of the department of periodontology and dental public health at the University of Hong Kong Faculty of Dentistry.
Different ways to brush
More than 40% of stroke survivors have difficulty swallowing at presentation, and more than 20% still experience this difficulty a month after their stroke. This is important because oral pathogens in dental plaque can be drawn into a patient's lungs, which can lead to aspiration pneumonia. This makes controlling plaque after stroke important for reducing the risk of pneumonia, the study authors wrote.
Despite this risk, limited evidence exists about the effectiveness of oral health promotion interventions in stroke survivors. Therefore, the researchers conducted the current study, which randomly assigned stroke survivors to one of two groups:
- Control group: Daily manual toothbrushing with an Oral-B toothbrush with super thin and extra soft bristles (Procter & Gamble) with Colgate Maximum Cavity Protection toothpaste (Colgate-Palmolive)
- Test group: Daily powered toothbrushing with Oral B Pro-Health DB4010 (Procter & Gamble) with Hexigel 1% chlorhexidine gluconate gel (ICPA)
The study participants, who were stroke patients at five public hospitals in Malaysia, each received an oral hygiene kit containing their assigned toothbrush and toothpaste from a dental assistant who provided oral hygiene instruction. The patients underwent oral health assessments at baseline, three months, and six months.
The study included 86 patients at baseline, with 54 (62.7%) patients assessed at all three time points. Among them, 68 patients (79.1%) did not have a removable dental prosthesis, and 75 (87.2%) had experienced their first stroke, which was ischemic for 77 patients (89.5%). Sixty-one (70.9%) had a Modified Barthel Index (MBI; a modified measure of activities of daily living) score of less than 50, indicating severe to total dependency, and 33 (38.4%) had severe cognitive impairment, as measured with the Mini-Mental State Examination.
Dental plaque index scores, which were measured at six sites per tooth, were high at baseline but significantly dropped over time between all time points. However, the researchers found no statistically significant differences in scores between the treatment groups at any point.
| Dental plaque scores by plaque reduction method | ||
| Manual toothbrush (n = 29) |
Power toothbrush + gel (n = 25) |
|
| Baseline | 1.78 | 1.76 |
| 3 months | 1.31 | 1.27 |
| 6 months | 1.07 | 0.92 |
| p-value | < 0.001 | < 0.001 |
Baseline plaque levels and functional dependency levels were key predictors of plaque levels at six months, with those with higher functional dependency at baseline having higher plaque levels at six months.
This study used chlorhexidine gel in part because the use of chlorhexidine mouthwash may be difficult for patients with dysphagia. Chlorhexidine gel was found to be effective and can be used as an alternative approach in these patients, the authors noted.
Keeping it basic
The effect of prestroke oral health status on dental plaque scores measured in the study remains unclear, the authors wrote.
However, the results suggest that future studies might examine the use of more intensive oral hygiene approaches with frequent use or higher concentrations of chemical agents among those with higher levels of functional dependency. Additionally, the authors suggested that future studies look at the effects of focusing oral hygiene care interventions on stroke caregivers.
Nevertheless, since the current study found no differences in plaque levels between the treatment groups, this suggested the wisdom of keeping routines basic and less expensive, although further research on this would be useful, the authors noted.
"The conventional oral hygiene regime of manual toothbrushing with commercially viable toothpaste twice daily is supported given that it is a relative simple and inexpensive means to control dental plaque during stroke rehabilitation," they concluded.