SAN FRANCISCO - Updates to periodontitis and peri-implant disease classifications can help dental professionals improve the care of their patients, according to a presentation at the 2019 ADA FDI World Dental Congress.
The new classifications, which aim to allow dental professionals to better diagnose, prevent, and treat periodontal and peri-implant diseases, were released in June 2018 following a thorough review from approximately 100 experts from around the globe.
"The new classification facilitates precision medicine in dentistry," said presenter Søren Jepsen, DDS, PhD, chairman of the periodontology, operative, and preventive dentistry department of the University of Bonn in Germany. "It is much simpler than you might think at first glance."
Periodontal disease
 Søren Jepsen, DDS, PhD.
Søren Jepsen, DDS, PhD.Under the new guidelines, periodontal disease is defined as the following:
- Periodontitis (formerly aggressive and chronic)
- Necrotizing periodontitis
- Periodontitis as a manifestation of systemic conditions
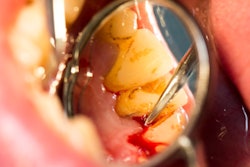
The key consensus was that bleeding on gentle probing is a sign of gingival inflammation, Dr. Jepsen noted. Bleeding of more than 10% is considered abnormal.
Dentists also must consider a patient's overall health status and some of the following risk factors before making a diagnosis:
- Smoking
- Nutritional factors, such as a vitamin C deficiency
- Hormone changes, such as puberty
- Diabetes
The classification of periodontitis includes new grading and staging categories based on severity, extent, complexity of management, and rate of progression.
Multiple variables determine the four categories of periodontitis. The three levels of periodontitis grading, which consider a patient's overall health status and risk factors, are listed below:
- Grade A: Low risk of progression
- Grade B: Moderate risk of progression
- Grade C: High risk of progression
"You do not have to populate every single cell of the grid before arriving at an assessment of stage and grade," Dr. Jepsen said.
Though staging cannot be revised, grading can be revised after assessing initial treatment responses, compliance, and risk-factor control, he added.
"A stage 4 patient can never be a stage 3 patient, but grading can improve," Jepsen said.
Peri-implant diseases
For the first time, experts also classified peri-implant diseases.
Peri-implant disease diagnosis requires the absence of erythema, bleeding on probing, and swelling and suppuration, Dr. Jepsen said.
Peri-implant mucositis requires bleeding or suppuration on gentle probing or the absence of bone loss.
Peri-implantitis requires bleeding on probing, increased probing depth compared with previous exams, and presence of bone loss that is beyond normal standards. Additionally, the diagnosis also requires probing depths of 6 mm or greater and bones levels 3 mm or more apical of the most coronal portion of the intraosseous part of the implant.
Jepsen emphasized the importance of probing and monitoring on a regular basis once diagnoses have been made.
"The classifications may seem complex, but for your patient, you can come to a very defined diagnosis in the end," he said.