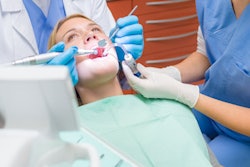
The Occupational Safety and Health Administration (OSHA) has released a proposed emergency temporary standard to protect health workers in hospital settings from COVID-19. Most dental practices will be exempt from the rules, but those providing services in hospital settings or treating patients with COVID-19 will be covered.
The standard runs more than 900 pages and aims to protect workers facing the greatest risk of exposure, such as those working in places where patients suspected or confirmed of having COVID-19 are being treated, according to OSHA. If the standard becomes a final rule, it will not apply to non-hospital-based ambulatory care settings where nonemployees are screened for COVID-19 prior to entry and will prohibit those diagnosed with or suspected of having COVID-19 from entering.
But there's more to know, according to Mary Govoni, RDH, CDA, a consultant and certified OSHA coach.
"The reality is that, according to OSHA's decision tree/flowchart for determining if a work setting is covered by the standard, many dental practices will be exempt from the standard," she said. "But in order for that to be true, the dental practice must be screening all nonemployees who enter the facility, and they cannot allow anyone with suspected or known COVID-19 to enter the facility. This would preclude practices from performing emergency treatment on patients with symptoms or who have tested positive for COVID-19."
That's not all. The standards that affect dental practices the most are the U.S. Centers for Disease Control and Prevention (CDC) Guidelines for Infection Control in Dental Health Care Settings, which was released in 2003, and the CDC Guidance for Dental Settings During COVID-19, Govoni pointed out.
"Although they technically are not rules, OSHA expects dental settings to follow CDC guidelines and use them for enforcement guidelines during inspections," she added.
The process
The new standard was recently submitted to the Office of the Federal Register for review and does not become effective until it is published in the Federal Register. The review process and timeline for the publication have not been disclosed. The standard may change during the review process, and only the version published in the Federal Register is the official final rule.
The administration can issue an emergency temporary standard when it determines that workers need to be protected from serious dangers, such as exposure to toxic substances, agents, or diseases. Once a standard is published in the register, employers must comply with most provisions within 14 days. Employers must comply with the remaining provisions within 30 days, according to an OSHA release.
Aerosol-generating procedures
Additionally, the standard defines "aerosol-generating procedures" as those that involve the use of air/water syringes, air polishing, air abrasion, ultrasonic scalers, and high-speed handpieces. In settings covered by the rule, employers would need to ensure employees have National Institute for Occupational Safety and Health (NIOSH)-approved respirators, gloves, an isolation gown or protective clothing, and eye protection when they are performing aerosol-generating procedures on suspected or confirmed COVID-19 patients.
Employers are encouraged to provide elastomeric respirators or powered air-purifying respirators instead of filtering facepiece respirators. The employees present during an aerosol-generating procedure also must be limited to those who are essential, and the procedure must be performed in an airborne-infection isolation room, if possible.
After a procedure is completed, the room's surfaces and equipment must be cleaned and disinfected, according to OSHA. Current guidance from the CDC, which was updated in December 2020, recommends that employees in all dental settings wear N95 respirators or a higher level of protection and take other precautions when they are doing procedures that cause aerosolization, Govoni said.
"OSHA expects dental practices to be following this recommendation," she added.
The standard also requires every dental office, regardless of practice setting, to have a COVID-19 plan and conduct a workplace-specific hazard assessment, according to a statement issued June 14 by the ADA. The organization has created a guide and checklist to walk dentists through the process.
"The strengthened infection control guidance and very low COVID-19 infection rate for dentists and dental hygienists prove that dental practices are safe workplaces," ADA President Dr. Daniel Klemmedson said in the statement.
Additional requirements
Furthermore, employers of oral health professionals who work at nonexempt settings will be required to take several other actions, including the following:
- Restrict and monitor entry areas where direct patient care is provided.
- Provide and ensure employees wear facemasks indoors and when traveling in vehicles with others for work-related business.
- Provide reasonable time and paid leave for employee vaccinations.
- Ensure employees receive training about COVID-19 transmission.
Dental team members who will not be affected by the standard are encouraged to use it to guide infection control practices at dental offices.
"This tailored standard allows OSHA to help the workers most in danger of contracting the virus, while the updated guidance will give other businesses across the country the information they need to help protect unvaccinated workers and continue mitigating spread in the workplace," said Jim Frederick, the acting assistant secretary of labor for OSHA, in a press release issued June 10 by the administration.
Employers can determine whether they are exempt from the standard on the OSHA website.