Low-level lasers reduced pain following extraction and implant surgeries in a pair of blinded randomized controlled trials published on September 5 in the Journal of Oral and Maxillofacial Surgery and the Journal of Photochemistry and Photobiology.
The split-mouth studies each enrolled about a dozen participants and evaluated the effect of low-intensity laser therapy, also known as photobiomodulation (PBM) therapy, on pain. Patients reported their pain levels using a visual analog scale (VAS) -- a 10-cm line, where one end represents no pain and the other end equates to unbearable pain.
Participants in both trials reported significantly less pain on the VAS on the side of their mouth treated with the laser. Both groups attributed the finding to the laser's anti-inflammatory effects.
"Laser light has biological effects that can modulate inflammatory processes," wrote the authors of the J Oral Maxillofac Surg paper, led by Dr. Henrique Hadad. Additionally, in the J Photochem Photobiol paper, lead author Birang Reza and colleagues noted that "photobiomodulation has been used as a therapeutic method for the healing of wounds and controlling pain and inflammation."
Laser for third-molar extractions
In their study, Hadad, a doctoral student at the Sao Paulo State University School of Dentistry in Brazil, and colleagues investigated the use of a red low-intensity laser on patients scheduled for third-molar extractions. The group recruited 13 patients for the split-mouth trial. The patients were all young and healthy, with lower molars in need of extraction.
The patients underwent mandibular left and right third-molar extraction 21 days apart. They were randomly assigned to receive PBM laser treatment on one side of their mouth and a placebo red-light treatment on the other.
The authors performed the PBM therapy with a diode laser at a wavelength of 810 nm. The treatment lasted for six seconds.

Patients reported significantly less pain with the low-level light therapy than the simulated red-light treatment. PBM therapy also better controlled swelling and was associated with a slightly wider mouth opening. As a result, lasers can be considered as an adjuvant therapy for third-molar extraction, the authors wrote.
"The results obtained through the VAS for pain in this study demonstrated good control of postoperative pain when the laser was applied," they wrote.
Lasers for implants
In the other study, Reza, a periodontics professor at the Isfahan University of Medical Sciences School of Dentistry in Iran, and colleagues investigated the effectiveness of lasers with different intensities on patients scheduled for implant placement. The researchers recruited 21 patients in need of 42 implants. The patients were generally healthy and had a median age of 47.
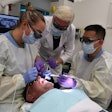
 (A) Implant insertion, (B) flap suturing, and (C) laser therapy on lingual side. Image courtesy of Reza et al and J Photochem Photobiol. Licensed under CC BY-NC-ND 4.0.
(A) Implant insertion, (B) flap suturing, and (C) laser therapy on lingual side. Image courtesy of Reza et al and J Photochem Photobiol. Licensed under CC BY-NC-ND 4.0.An experienced implantologist performed mandibular implant placement on the patients' mandibular left and right side in a single session. The patients were assigned to randomly receive laser therapy on one side and a placebo red-light laser treatment on the other.
The PBM therapy involved the use of a diode laser on the buccal, occlusal, and lingual sides of the implant regions. The implantologist first used a lower-intensity, 60-nm beam for 200 seconds to target surface tissues before switching to a higher-intensity beam of 810 nm for 20 seconds to reach deeper tissues. The PBM therapy was performed twice: once on the day of surgery and again two days after surgery.
The laser resulted in "significant improvement" in VAS pain scores 12, 24, and 72 hours after surgery. It also resulted in significantly better wound healing scores at three and 14 days after surgery.
"Therefore, PBMT [PBM therapy] might enhance wound healing and relieve pain after dental implant surgery," the authors wrote.