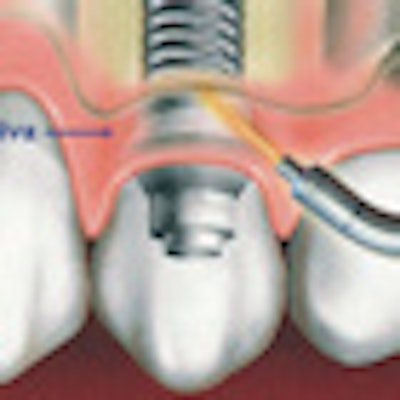
A team of Canadian researchers is developing a diagnostic tool they say can enhance the early detection and monitoring of peri-implant inflammation and thereby reduce the number of implant failures (Journal of Periodontal Research, March 11, 2011).
Several diagnostic techniques are currently used to assess the viability of newly placed implants, including implant mobility, sulcular probing, probing depth, and radiography.
— Kan-Zhi Liu, MD, PhD
However, "these tools are not sensitive enough to accurately detect early lesions, progressive lesions, and sometimes even late lesions, which are important in avoiding further loss of soft and hard peri-implant tissues and eventually implant failure," noted lead author Kan-Zhi Liu, MD, PhD, a senior research officer at the National Research Council of Canada’s Institute for Biodiagnostics and an associate professor in the department of dental diagnostic and surgical sciences, University of Manitoba.
These limitations prompted Dr. Liu and his colleagues to experiment with a more sensitive technique: optical spectroscopy.
"Nowadays more and more people are using implants," he told DrBicuspid.com. "There is a 7% to 20% chance that an implant will develop inflammation, and this is a destructive, infectious disease that affects hard and soft tissue around the implant. But existing diagnostic methods cannot predict disease activity or progression, and there is much interest in finding alternative methods that can do this promptly and thoroughly."
Multiple indicators
In an earlier study, Dr. Liu and colleagues from the University of Manitoba and the University of Louisville School of Dentistry established that optical spectroscopy can simultaneously determine multiple inflammatory indices directly in periodontal tissues in vivo (J Periodont Res, February 2009, Vol. 44:1, pp. 117-124).
"Visible, near-infrared (NIR) spectroscopy has the potential to be developed into a simple, reagent-free, user-friendly, chairside, site-specific, diagnostic, and prognostic test for periodontitis," they concluded.
In this follow-up research, they focused specifically on the ability of optical spectroscopy to measure regional tissue hemodynamics in periodontal tissue. Their goal was to further evaluate the diagnostic potential of optical spectroscopy in peri-implant inflammation in vivo by simultaneously assessing multiple inflammatory parameters:
- Tissue oxygenation
- Total tissue hemoglobin
- Deoxyhemoglobin
- Oxygenated hemoglobin
- Tissue edema
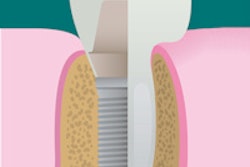
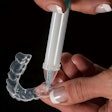
Dr. Liu and his team connected a near-infrared spectrometer (5-W halogen lamp was the light source) to a customized fiber-optic probe designed specifically for use in the oral cavity. The intraoral probe comprises a 180-mm-long stainless steel shaft, 5 mm in diameter, that houses 29 fiber-optic bundles. A central fiber area delivers light to the oral cavity, while an outer ring of fibers collect the spectra of light that is subsequently backscattered from the tissue.
For this study, 64 systemically healthy subjects were recruited from the Oral Implantology Clinic of Guarulhos University in Brazil in June and July 2009. The patients all had dental implants with various stages of inflammation. Medical and dental histories were obtained, and full-mouth periodontal and peri-implant exams were performed, including periodontal probing and periapical intraoral radiographs.
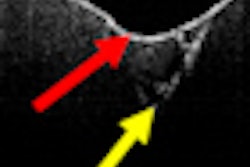
Using the spectrometer, visible-NIR spectra were then obtained, processed, and evaluated from healthy (n = 151), mucositis (n = 70), and peri-implantitis (n = 75) sites. The spectra were then analyzed to determine the relative contribution of each inflammatory component to the overall spectrum.
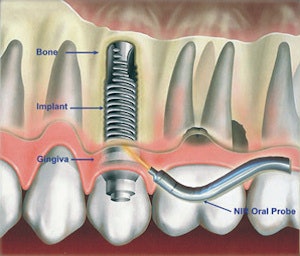 A proposed near-infrared oral probe can noninvasively assess peri-implantitis earlier and more accurately than conventional methods. Image courtesy of Kan-Zhi Liu, MD, PhD.
A proposed near-infrared oral probe can noninvasively assess peri-implantitis earlier and more accurately than conventional methods. Image courtesy of Kan-Zhi Liu, MD, PhD.The researchers found that tissue oxygenation at the peri-implantitis sites was significantly decreased (p < 0.05) when compared with that at health sites, which they attributed to an increase in deoxyhemoglobin and a decrease in oxyhemoglobin at the peri-implantitis sites compared with the mucositis and healthy sites. They also found that the tissue hydration index derived from the optical spectra in mucositis was significantly higher than that in other groups (p < 0.05).
"In general, the results demonstrated that hemodynamic changes can be clearly detected around diseased peri-implant sites by this convenient, noninvasive technique, especially in relation to tissue oxygenation and tissue hydration," the authors concluded. "The data provide new insights into the diagnosis of peri-implant diseases."
But Dr. Liu believes this is just the beginning, noting that the institute has already been in discussion with potential partners to commercialize this technology.
"These were proof-of-feasibility studies," he said. "Now we are doing some translational clinical studies to demonstrate that this tool can be used for clinical applications. Our hope is that general dentists would use this simple, operator-friendly, portable device to shine light on periodontal tissue and provide information about gingivitis and normal tissue."
It could be a complementary tool for assessing periodontitis as well, he added.
"This a very small unit that would be perfect for use at chairside," Dr. Liu concluded.