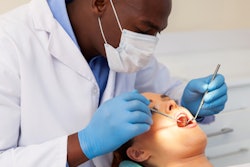
The number of U.S. children receiving dental care significantly increased from 2000 to 2014, according to a new study in Pediatrics. Even more positively, the researchers found a steep narrowing of coverage disparities in race/ethnicity and income. However, they are concerned about the future of treatment coverage under the new U.S. administration.
The authors knew from previous studies that insurance coverage had improved as pediatric enrollment in public health insurance through Medicaid and the Children's Health Insurance Program (CHIP) increased. However, they didn't know whether that translated to increased utilization and what the difference was among children of different races and ethnicities, as well as between poor and better off children.
"The expansion of Medicaid and CHIP financing for children from lower socioeconomic groups has made it easier for them to access these services," said study co-author Andrew Racine, MD, PhD, in an interview with DrBicuspid.com.
Dr. Racine is the system senior vice president and chief medical officer at Montefiore Medical Center and a professor of clinical pediatrics at Albert Einstein College of Medicine in New York.
Measuring changes in access
The health insurance coverage gains for U.S. children seen in recent years are expected to have improved access to healthcare services, particularly for vulnerable populations. Nonetheless, few studies have analyzed children's healthcare access trends, including by race/ethnicity and income, and whether the magnitude of disparities has diminished.
For future healthcare policy decisions, it is important to assess insurance coverage rates and also access to healthcare and disparities in access, the authors wrote (Pediatrics, November 15, 2016). Millions of children may become ineligible for public or subsidized coverage by 2019 if funding for separate state CHIP programs expires or states are allowed to roll back Medicaid and CHIP eligibility thresholds to statutory minimums.
Therefore, the researchers examined data from 173,038 children up to age 17 from the 2000 to 2014 National Health Interview Survey (NHIS), a nationally representative, cross-sectional survey of U.S. households. Within each household, a sample child was chosen. An in-person interview was conducted with a parent or adult knowledgeable about the child's health and healthcare.
They were asked about whether the child had health insurance and the type. They were also asked whether the child had visits with any type of dental professional (including dentists, oral surgeons, orthodontists, or hygienists), well-child visits, and doctor's office visits and also about usual sources of care and unmet health needs, which included dental care, within the previous year. The dental care question was asked only for children ages 1 to 17, with the sample size therefore smaller for that question.
Children were classified into three income categories:
- Poor (less than 100% of the federal poverty level)
- Near poor (between 100% and 199%)
- Not poor (200% and above)
The lack of a dental visit within the previous year dropped by half from 2000 to 2014 in Hispanic children and by 37% in black children, nearly eliminating disparities with white children, as shown in the table below.
| No dental visit within the previous year, 2000-2014 |
||
| 2000 | 2014 | |
| Hispanic children | 43.2% | 21.8% |
| Black children | 32.8% | 20.7% |
| White children | 25.1% | 19.5% |
For unmet healthcare needs, the higher rates seen in children in poor (12.8% in 2000 to 8.5% in 2014) and near-poor families (13.0% to 7.2%) narrowed compared with those from all other families (4.8% to 4.2%).
The rate of uninsured children dropped significantly from 12.1% in 2000 to 5.3% in 2014, representing an additional 4.9 million children receiving coverage. At the same time, public coverage among the children in the study increased from 18.9% to 38.9%, and private coverage decreased from 69.0% to 55.8%. Increases in public coverage and decreases in private coverage were found across all racial/ethnic and income groups.
The uninsured rate narrowed for Hispanic children compared with white children and was eliminated for black children compared with white children, as shown in the table below.
| Uninsured rates in children, 2000-2014 | ||
| 2000 | 2014 | |
| Hispanic children | 26.1% | 9.3% |
| Black children | 11.7% | 3.3% |
| White children | 8.2% | 4.0% |
Steeper declines in uninsured rates were seen for children in poor (22.2% to 5.9%) and near-poor (21.2% to 8.8%) families compared with others (6.0% to 3.5%).
"We have managed to satisfy a pent-up demand," Dr. Racine said regarding the increases seen in accessing dental care, in conjunction with increased rates of insurance. "We may not have reached the limits of what health insurance expansion can produce. Even if we did nothing and kept things the way they are, we might expect to see continued improvement."
Future public insurance coverage unknown
Gains in health insurance coverage appeared to explain some but not all of the increases in access to care, the authors wrote. Some states have quality monitoring programs with performance improvement programs targeting goals, including increasing dental visit rates, while some have worked to improve dental provider availability by increasing dental service reimbursement rates. And states are now required to provide dental services to all children enrolled in Medicaid and CHIP.
The Patient Protection and Affordable Care Act (ACA) had the effect of bringing more children who had previously been eligible for public insurance coverage into the system, Dr. Racine said.
In a separate commentary in the same Pediatrics issue, Stephen Berman, MD, a professor of pediatrics at the University of Colorado School of Medicine and School of Public Health, wrote that the study's findings have important implications for future child healthcare policy decisions.
"First, all children should have coverage, and strong efforts must be made to reach the 5.3% who remain uninsured," he wrote. "These efforts should target the near-poor and Hispanic families because the gap is greatest for these populations. Second, the reauthorization and continued funding of the Children's Health Insurance Plan, due to terminate in 2019, is essential and should be addressed sooner rather than later."
He also recommended that ACA exchange plans become more affordable to near-poor and middle-class families.
The study's strengths were its use of nationally representative NHIS data with consistent measurement over time and the ability to link health insurance and healthcare access data, according to the study authors. A limitation, though, was its reliance on parents reporting the use of health services not validated against medical records.
Dr. Racine noted that the availability of public health insurance, the willingness of dental practitioners to provide care to those with this coverage, and the willingness of our society to ensure that rates paid to practitioners are in line with the cost of providing them will determine if the rates of children receiving dental care increase in the coming years.
"Depending upon the policy responses of the new administration to these programs, we could see a complete reversal of these funds," Dr. Racine said regarding the incoming Trump administration's position on funding for children's health insurance through Medicaid and CHIP.