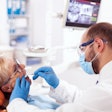
Dentists rarely adhered to ADA recommendations to defer treating patients who presented with elevated blood pressure levels, and the procedures were completed without causing measurable harm. The study was published on September 19 in the Journal of Dental Education.
This approach aligns with newer, less restrictive guidelines from the American Heart Association (AHA). Additionally, those patients who had treatment deferred were unlikely to return for dental care with improved blood pressure control or taking new blood pressure medicine, the authors wrote.
“Oral health providers must weigh the risks and benefits of care deferral and can consider an expanded role in hypertension management in dental settings when caring for patients with elevated blood pressure,” wrote the authors, led by Dr. Lisa Simon of the department of general internal medicine and primary care at Brigham and Women's Hospital in Boston.
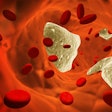
In the dental setting, blood pressure measurement can be a valuable tool for prompt referral for further diagnosis and treatment. Currently, the ADA recommends that dentists take blood pressure readings at dental visits, and several published resources have recommended dentists postpone treatment for patients with blood pressure levels as low as 160/100 mmHg for elective oral healthcare and 180/110 mmHg for urgent dental treatment.
In addition to previous research showing no evidence supporting deferring dental treatment for incidentally detected high blood pressure, the AHA Guideline on Preoperative Cardiovascular Evaluation and Management of Patients Undergoing Noncardiac Surgery also takes a slightly different stance. Patients with medically optimized heart disease who remain asymptomatic don’t need additional evaluation for low-risk surgeries, including tooth extractions. Also, the AHA recommends deferring surgery at a much higher threshold than the ADA at 180/110 mmHg, according to the study.
To explore the rates of hypertension and treatment deferral at a dental school clinic, a retrospective study was conducted. Data was extracted from a chart review of 26,821 patients who sought treatment at a clinic. Differences in dental procedures, the time between visits, and the number of antihypertensive medications were calculated between patients with and without a blood pressure reading that exceeded the ADA’s guidelines for elective treatment, according to the study.
Of the patients, 1,265 (4%) had blood pressure readings that were above the ADA’s guidelines for proceeding with dental treatment. These were patients with a blood pressure reading over 160/100 mmHg. Only 4% of these patients had a procedure deferred, the authors wrote.
For those that did have treatment postponed, the average number of days until the next visit was 88 days (95% confidence interval, 77 to 98 days), they wrote. The study had limitations, including that it was a single-site study, limiting generalizability, they wrote.
In the future, researchers should build on these findings to better understand the frequency of treatment deferral for elevated blood pressure in various dental settings, as well as the possible risks and benefits of postponing care, Simon et al wrote.
“Dental providers are encouraged to obtain a comprehensive history and physical examination and understand a patient’s functional status to best ascertain a patient’s risk when presenting for dental work,” they wrote.