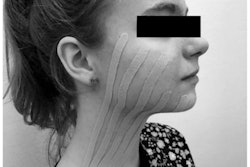
An 11-year-old boy’s painful chronic lockjaw may have been triggered by conversion disorder, a mental health condition that causes physical symptoms, according to a case report published on April 7 in Special Care in Dentistry.
Nonarticular hysterical trismus caused the child’s jaw to completely lock, causing moderate to severe pain and affecting his ability to eat, for three months. After consulting with specialists, including a psychologist, and undergoing myofascial therapy, the boy was able to open his mouth and return to normal eating habits, the authors wrote.
“This report highlights the importance of complete history taking and a thorough clinical examination to make a correct diagnosis in a patient with trismus,” wrote the authors, led by Dr. Donald Goodman of the University of California, Los Angeles (UCLA) Orofacial Pain Department.
An 11-year-old boy with a locked jaw
The patient, a boy, and his mother went to the UCLA Orofacial Pain and Dental Sleep Medicine Clinic because his jaw had been locked and was causing moderate to severe pain for three months. The pain was sharp, aching, and shooting and never occurred in the past.
About two weeks before his jaw locked, the boy experienced some temporomandibular joint (TMJ) noise and dysfunction, including locking, stiffness, and pain on both sides. He admitted that he had a habit of clenching his teeth, the authors wrote.
The boy explained to UCLA clinicians that he was sitting in class when he turned his head to the right and felt his jaw “slip.” Since that occurrence, he reported that he couldn’t open his jaw wide enough to insert his little finger.
Since he could not open his mouth, he couldn’t eat solid food. The boy had lost about 20 pounds and only was drinking fluids, protein shakes, and smoothies.
His mother said that she had seen his mouth open about one-half inch when he had a cold and his nose was stuffed up or when he was in deep sleep. Other than experiencing blunt trauma to his head and neck following a ground-level fall about six months prior, the child was healthy. The fall did not cause a jaw fracture or loss of consciousness, the case report's authors wrote.
Prior to visiting the clinic, the boy was seen by two TMJ-focused dentists. He underwent a computed tomography (CT) scan and was given a soft oral appliance, which had to be placed between his teeth when he could open his mouth.
Though the scan was of poor quality, the dentist considered the findings grossly abnormal. The dentist believed the fall led to vertebral disc slippage, which affected the boy’s ability to open his mouth. Therefore, the clinician sent him to a chiropractor and a physical therapist. The child visited a chiropractor and allowed the chiropractor to readjust his neck, according to the report.
Subsequently, a maxillofacial surgeon placed the boy under sedation and opened his mouth up to 36 mm. The surgeon observed that the boy's mouth opened without any difficulty. During the procedure, a device was placed in the boy’s mouth and increased the opening to 38 mm. After the device was removed, though, the boy's mouth opening was reduced to 24 mm and closed without any difficulty.
When he awoke from this procedure, the boy was crying about the pain he felt. The surgeon referred him to a psychologist because he suspected the boy may have had a psychological disorder.
About a week after the procedure with the maxillofacial surgeon, the patient started physical therapy, which included massage and ice and heat therapy. That continued for six weeks, but the boy experienced no improvement.
From there, the boy saw a pediatric psychologist; a neurologist; and an ear, nose, and throat specialist. Magnetic resonance imaging (MRI) of his brain showed nothing abnormal. He was prescribed an antispasmodic drug, which he took for two months but stopped taking after it didn’t change his symptoms.
An orofacial pain specialist sent the boy to have a TMJ MRI, which showed bilateral anterior disc displacement. This finding prompted the clinician to give him several lidocaine trigger point injections to the superficial and deep masseter muscles.
Additionally, the boy was prescribed cyclobenzaprine (5 mg) and amoxicillin (400 mg/5 mL), which was to be taken twice per day in conjunction with the injections. The orofacial pain specialist also prescribed 5 mg of prednisolone twice daily, but the boy discontinued the corticosteroid after experiencing severe side effects, including major crying spells and sadness, according to the report.
Since none of the treatments worked, the child was referred to a pain psychologist, and it was recommended that he have TMJ surgery with lavage. However, his mother refused the procedure.
To relieve the pain, the boy was taking 300 mg of ibuprofen three times per day as needed. Also, the pain psychologist provided biofeedback, hypnosis, and counseling to the boy. Ultimately, the psychologist diagnosed the boy with hysterical trismus and myalgia and referred him to the UCLA clinic for consultation, they wrote.
At the UCLA clinic, his consultation confirmed the diagnosis of a conversion disorder but no other significant psychiatric conditions. After three sessions of biofeedback, hypnosis, breathing, relaxation, cognitive-behavioral therapy, and psychodynamic therapy, which included decreasing the attachment between the mother and son and counseling the mother to not reinforce the possibility of secondary gain (a perceived advantage that occurs secondary to the stated or real illness), the patient’s mouth opening improved. He was able to put three fingers, which measures about 33 mm, between his incisors. His eating also returned to normal, the authors wrote.
Furthermore, his counseling included employing strategies for handling anxiety and stress. The boy was counseled on how his emotions (anxiety, anger, fear, worry, and embarrassment) could contribute to and cause his physical symptoms. Also, the patient learned to stretch his chewing muscle by holding a cork between his teeth. He was instructed to stay on a soft diet and correct his body posture, they wrote.
During his last visit, which was about two months after seeing a psychologist and starting myofascial therapy, his active mouth opening improved to 35 mm, and his passive mouth opening improved to 39 mm. The boy reported being mostly free of pain. Occasionally, he had mild pain when opening his mouth. Also, his mood had improved, and he was engaging in activities, including dancing and playing the piano, that he enjoyed, according to the report.
What to know
Conversion disorder, also referred to as functional neurological symptom disorder, occurs when symptoms start suddenly following a stressful event. Individuals with this disorder have altered voluntary motor, cognitive, and sensory function symptoms that aren’t compatible with any neurological condition.
A conversion disorder diagnosis relies on the presence of unusual neurological-type symptoms that don’t conform to anatomical and physiological characteristics that support neurological diagnoses. A type of conversion type reaction is hysterical trismus, according to the report.
Long-term, trismus may result in the atrophy of associated structures, leading to fibrous or bony adhesions or ankylosis. Also, trismus can lead to constraints, including social injunctions that cause anxiety and danger, for patients, they wrote.
Nevertheless, this case highlights how conversion disorders may lead to dramatic physical symptoms. To properly diagnose trismus, dentists must consider all possibilities, the authors wrote.
“Obtaining a complete history, including psychosocial, medical, drug and dental history, performing a thorough clinical and neurological exam, and taking appropriate imaging are important to rule out other causes of trismus,” Goodman et al wrote.