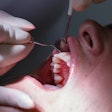
MIAMI - Infrared spectroscopy may help diagnose periodontitis, a researcher said Thursday at the International Association for Dental Research (IADR) meeting.
Dentists need more accurate ways of diagnosing the disease because current methods are so imprecise that many patients are overtreated or undertreated, said Kan-Zhi Liu, M.D., Ph.D., a research officer at the Institute for Biodiagnostics, National Research Council Canada and an associate professor of dentistry at the University of Manitoba. "Probing is the most widely used diagnostic method, but it doesn't tell you whether a site is active or inactive."
Other researchers have focused on biomarkers characteristic of the disease, but periodontitis is caused by so many different factors that the presence of just one or two of these markers doesn't tell you whether someone has the disease.
Dr. Liu and his colleagues used two different types of infrared spectroscopy: near-infrared spectra to measure inflammation in specific sites in the patient's mouth, and midinfrared spectra to identify the overall pattern of multiple biomarkers in gingival crevicular fluid (GCF).
To test the first approach, they invented a spectrometer with a small probe that could be inserted into a patient's mouth. "It's very portable and can be used in a crowded dental clinic," Dr. Liu said.
A source on the probe shines light on a site in the patient's mouth. A receptor on the same probe measures the wavelength of the light reflected from the tissue and sends information to a computer. "The procedure is quite simple," Dr. Liu said.
The researchers used a modified Beer-Lambert unmixing model that incorporated a nonparametric scattering loss function to determine the relative contribution of each inflammatory component to the overall spectrum.
Using different wavelengths reflected from the tissue, they analyzed the overall presence of hemoglobin to measure perfusion and the presence of oxygenated hemoglobin to measure oxygenation. They also used the presence of water to measure edema.
They found a statistically significant difference in these measures between healthy and inflamed tissue, according to Dr. Liu.
At the same time, the researchers took GCF samples and used a different spectrometer to identify an overall pattern created by the lipids, proteins, and DNA. With this method, they found that there were statistically significant differences between the patterns in healthy tissue and inflamed tissue in periodontitis. "The overall accuracy was 98%," Dr. Liu said.
Only a marginal difference was found between healthy tissue and gingivitis, he added.
Looking at the "big picture" of these patterns is more effective than focusing on one or two biomarkers, Dr. Liu said. "That's the beauty of our technology."
Panel co-moderator Panos Papapanou, D.D.S., Ph.D., a Columbia University professor of dentistry, questioned whether testing only a few specific sites could accurately produce a periodontitis diagnosis.
After Dr. Liu's presentation, Xiaoming Xiang, D.D.S., Ph.D., a periodontist working with Dr. Liu, argued that the method was still valid because individual sites within the patient would still need to be treated.
The researchers are currently looking for a commercial partner to bring the technology to market.
The research was funded by the Canadian Institutes for Health Research, the Natural Sciences and Engineering Research Council of Canada, and the U.S. National Institute of Dental and Craniofacial Research, among others. "I think everybody realizes the importance and novelty of this science," Dr. Liu said.
Copyright © 2009 DrBicuspid.com