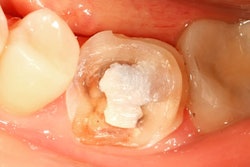
When a composite resin restoration fails, the most common approach is to replace it. Now, a new study has compared the outcomes over a 10-year period of replacing a composite restoration versus repairing it. Could repair be a more conservative and equally viable option?
New data suggest that this is so, according to a triple-blind clinical trial by researchers from the departments of restorative dentistry at the University of Chile Faculty of Dentistry and the Major University Faculty of Dentistry, both in Santiago, as well as the University Estadual Paulista School of Dentistry in Araraquara, Brazil (Journal of Dentistry, June 4, 2014).
"The repair of composite resins should be elected when clinically indicated, because it is a minimally invasive treatment that can consistently increase the longevity of restorations," the researchers wrote. Also, it costs less for the patient.
The replacement option has several drawbacks, such as a greater time commitment, the risk of a larger restoration resulting from the procedure, and the risk of injury to the dentin-pulp complex. The researchers sought to ascertain the possible benefits of the replace option by looking at the life span of repairs made to localized clinical defects in composite resin restorations where a replacement had been planned.
"The hypothesis was that repairing a restoration would recover its clinical condition, increase its longevity after the initial 10 years, and would be similar to replacing the restoration," they wrote.
“Repairing ... should be the treatment of choice.”
For the study, the researchers whittled 66 patients with 356 restorations to 28 included patients with a total of 50 composite restorations in their mouths. Patients at high risk of caries, those with marginal defects greater than 3 mm in their restoration, or those with xerostomia were excluded, as well as those with restorations where "clinical judgment" determined that repair was not indicated.
The included restorations had secondary caries and/or localized, marginal, anatomical deficiencies. These less-than-ideal restorations had a Bravo or Charlie rating applied to it based on the U.S. Public Health Service Criteria, while restorations in good shape were given an Alpha rating.
The researchers randomly assigned restorations with secondary caries (Charlie), marginal defects (Bravo), and/or undercontoured anatomical form defects to the repair (n = 25: class I = 12 and class II = 13) or replacement (n = 25: class I = 13 and class II = 12) groups, they explained. The latter served as a control group.
Two blinded examiners independently assessed the restorations immediately after treatment for a baseline reading and 10 years afterward. These assessments were done with a direct visual examination and an indirect radiographic examination via bitewing with four parameters in mind: marginal adaptation, secondary caries, anatomic form, and color. Differences in opinion between the examiners were settled with a third.
The repairs began with the removal of defective tooth tissue and part of the restorative removal with carbide burs (Komet, Brasseler) for additional diagnosis and evaluation. Preparation and priming of the cavity with Adper Prompt L-Pop (3M ESPE), a self-priming resin bonding system, and restoration with Filtek Supreme (3M ESPE) followed. "In this study, the most frequent reason for repairing the resin was a problem of the anatomical form or marginal adaptation," the researchers noted.
In the replacement group, the defective restorations were complete removed and replaced, using Vitrebond (3M ESPE), a glass-ionomer liner for deep dentin and the same primer and resin composite as the repair group. Secondary caries were the leading cause of replacement in this group.
During the study period, two patients from each group dropped out of the study. And in that time, the proportion of marginal adaption Bravos similarly increased for both groups, while a 5:1 ratio of failures given a Charlie rating in the repair group compared with the replacement group arose. After 10 years, the researchers observed the following distribution:
| Group | Repair | Replace |
| Alphas | 36% | 35% |
| Bravos | 60% | 65% |
| Charlies | 4% | 0% |
The researchers found the secondary caries were predominantly classified as Alpha over the term of the study for both groups. By the end of it, 93% of both were classified as Alphas, and two from each group had lost restorations as a result of decay, they noted. The differences between the groups with respect to secondary caries were not statistically significant (p > 0.05).
The researchers also rated how well the restoration followed the anatomic form of the tooth in both groups after 10 years and noted two restoration failures in the repair group:
| Group | Repair | Replace |
| Alphas | 40% | 57% |
| Bravos | 56% | 43% |
| Charlies | 4% | 0% |
The anatomy may have deteriorated to Bravo values, the researchers explained, but the restorations were still clinically acceptable. They also noted a statistically significant differences between the years that it took place within each group (p > 0.05). At five years, most of the replacement group had been rated Bravo, a percentage that held to the 10-year mark.
When color was considered, the researchers noted a higher proportion of Alphas in the replacement group than the repair one, with 75% (and 17% Bravos) versus 92%, respectively. Both groups had 8% Charlie ratings, and no statistically significant differences were found, since both Alpha and Bravo ratings are clinically acceptable.
"This study suggests that it is possible to double the half-life of the original restoration with minimal intervention and consequently increase the life of the tooth," the researchers wrote. "Repairing defective composite resin with secondary caries, poor anatomy, or marginal adaptation problems should be the treatment of choice to prevent further damage to the dental pulp and to save the healthy tissue."