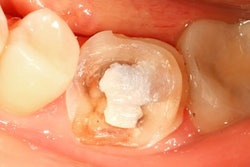
When a patient with advanced tooth wear needs extensive restoration at increased occlusal vertical dimension (OVD), how do you handle it clinically? Do you prepare all the teeth in a single day and place full-arch interim prostheses? Many practitioners do, but this can be tiring for both the patient and clinician, along with being difficult to schedule for all parties.
In a new case report in the Journal of Prosthodontics (February 6, 2015), Tarek El-Kerdani, DDS, and Arthur Nimmo, DDS, from the department of restorative dental sciences at the University of Florida College of Dentistry, proposed and demonstrated an alternative approach for these patients: preparing one arch and placing interim prostheses, while using composite resin in the opposing arch to maintain the newly established OVD.
Further, they recommended completing a diagnostic wax-up at the proposed OVD and then duplicating it in stone. Then, they load a vacuform matrix with composite resin that is applied to the unprepared etched teeth of the opposing arch. This restores form and occlusion until full contour interim prostheses can be placed when the patient returns.
This technique both restores OVD and provides occlusal stability with the opposing provisional crowns, according to the study authors.
Procedure
The decision to restore a patient at the existing or an improved OVD can be made after the present OVD has been clinically assessed, the authors noted. They suggested that a removable occlusal splint be fabricated to test the proposed OVD and also that a diagnostic wax-up be made at the tested OVD that will be the template for both the interim and definitive prostheses.
“This approach allows for tooth preparation in one arch at a time for patient and operator convenience.”
This technique under study will produce anatomic provisional composite restorations and will restore the lost OVD, along with withstanding occlusal forces until the interim prostheses are fabricated, they noted.
The case featured a 57-year-old woman who was categorized as a Prosthodontic Diagnostic Index (PDI) class IV dentate patient, due to the need for extensive reconstruction at an increased OVD. At the initial visit, the clinicians made two sets of maxillary and mandibular irreversible hydrocolloid impressions, along with a kinematic facebow record and centric relation (CR) record at the proposed OVD were made. Casts were poured and mounted in CR on a Whip Mix articulator model 3040.
Their first set of mounted casts was used for a full diagnostic wax-up, which was duplicated onto stone casts. At that point, maxillary and mandibular 0.75-mm vacuform matrices were fabricated. A mandibular processed acrylic resin bite splint was fabricated at the proposed OVD using the second set of mounted casts. The splint was delivered to the patient to use for three weeks, during which the patient reported only signs of normal wear and no signs of muscle fatigue.
The clinicians prepared maxillary and mandibular anterior teeth first to establish anterior guidance. They modified the bite splint in the incisal area of the mandibular anterior teeth to allow for the new anterior restoration. At the next visit, they prepared the maxillary posterior teeth and checked a vacuform matrix made from the duplicate diagnostic wax-up cast. The matrix was then loaded with acrylic resin and placed on the prepared teeth to create the maxillary posterior provisional crowns. The provisional crowns were finished and polished in the usual manner, then tried in the patient's mouth. The mandibular vacuform matrix also was tried in the patient's mouth and checked.
After light curing, the matrix was removed, and a finishing bur was used on the restorations. The practitioners verified the occlusion using an articulating medium, then the patient was instructed to floss between the splinted occlusal units using a floss threader.
At the next visit, the practitioners evaluated the composite resin restorations, which were found to be intact. The mandibular posterior teeth were prepared and interim prostheses were fabricated using a second mandibular vacuform matrix.
While the authors have reported success with this technique, they did note that one disadvantage is that the matrix produced occlusal composite surfaces that were connected, which means conventional flossing techniques for unsplinted teeth cannot be used. As noted above, the patient was instructed to use a threader or superfloss for flossing.
However, this "approach allows for tooth preparation in one arch at a time for patient and operator convenience," the authors concluded. The technique may also be used as an alternative for a removable splint for restoring OVD during the diagnostic phase, they noted.