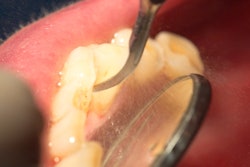
The best strategies for carious tissue removal have changed, but are you up-to-date on the latest clinical recommendations? Dentists should focus on improved treatment outcomes tailored to the tooth type and lesion depth, according to the author of a new review article.
Contemporary approaches for carious tissue removal and management are based on a changed understanding of caries from an infectious disease to an ecological imbalance within the dental biofilm, noted Falk Schwendicke, PhD, DMD, DDS, MDPH, from the operative and preventive dentistry department at Charité - Medical University of Berlin in Germany. This switch in perspective has called into question traditional therapies for caries and carious lesions.
"The only strong reason for removing carious dentin is to allow subsequent placement of a long-lasting restoration," he wrote (Journal of Esthetic and Restorative Dentistry, September 19, 2017). "Thus, carious tissue removal should be guided by how to improve treatment outcomes, not by the perceived degree of 'completeness.' "
His article was based on discussion by the International Caries Consensus Collaboration and resulting consensus statements. The collaboration consisted of 21 international clinical experts in cariology, operative dentistry, biomaterials science, clinical trials, systematic reviews, and guideline development from 12 countries. They met in Belgium in February 2015 to develop consensus recommendations for dental caries-related terminology, as well as for dealing with carious tissue removal and managing cavitated carious lesions.
Not taking it all
When caries was believed to be an infectious disease, treatment called for the eradication of causative micro-organisms and carious tissues, mainly bacterially contaminated and demineralized dentin, Dr. Schwendicke wrote. However, the newer understanding of the disease no longer requires removal of all carious dentin from a cavity.
“The only strong reason for removing carious dentin is to allow subsequent placement of a long-lasting restoration.”
Likewise, studies have found that removal of all bacteria from a cavity is not possible, and, if it were, it would not necessarily help to control lesion activity.
The more recent "ecologic plaque hypothesis" explains the development of caries as being caused by the dominance of acid-producing bacteria over acid-withstanding bacteria in the biofilm. Newer caries management strategies focus on reducing -- although not always eliminating -- invasive treatments, gaining control over biofilm and lesion activity, and rebalancing the equilibrium of dental hard-tissue mineral loss and gain.
For noncavitated lesions, this can include the patient limiting carbohydrate intake to rebalance biofilm, the use of mechanical or chemical oral hygiene control to remove or inactivate biofilm, and remineralization treatments using fluoride. Additionally, microinvasive treatment can be performed by removing a few micrometers of tissue and using resin to seal or infiltrate mainly enamel dental tissue, which can prevent acid diffusion into dental tissues and halt the disease process of treated lesions.
"For existing carious lesions, the priority should be to control its activity non- or microinvasively instead of removing and replacing them restoratively, thereby preventing further hard-tissue loss and postponing or avoiding the restorative cycle," Dr. Schwendicke wrote.
However, cavitated lesions still often require invasive and restorative strategies but no longer necessitate removing all bacteria before placement of restorations, since they create a seal that deprives remaining bacteria of carbohydrates, he noted. Likewise, demineralized dentin does not require removal since it can be remineralized.
"There is a consensus that the only strong reason for carious tissue removal before placing a restoration is to create a) a sufficiently large surface for bonding and b) a support for the restoration against masticatory forces," Dr. Schwendicke wrote.
4 goals for tissue removal
The experts at the consensus meeting decided that dentists should adopt the following goals when performing carious tissue removal:
- Retain sound remineralizable dentin or enamel.
- Hermetically seal residual carious dentin beneath the restoration by forming a peripheral zone to which a restoration can be bonded.
- Maintain pulp vitality by preventing pulp exposure and retaining the maximum amount of residual dentin possible.
- Lengthen the life of a restoration by creating surfaces for bonding and support.
Avoiding pulp exposure is most important in teeth with asymptomatic vital pulp with deep carious lesions, and it may allow them to be retained long term and help patients avoid painful, expensive, and invasive endodontic treatment, Dr. Schwendicke wrote.
The consensus group also agreed on the definitions of five types of carious tissue removal:
- Nonselective removal to hard dentin is now considered overtreatment and is no longer recommended.
- Selective removal to firm dentin in which firm dentin is left centrally and hard dentin peripherally is recommended for shallow or moderately deep lesions, allowing for placement of a long-lasting restoration and avoiding removal of remineralizable tissue.
- Selective removal to soft dentin, in which soft carious tissue is left over the pulp to avoid pulp exposure and allow a tight seal and placement of a durable restoration, is recommended for deep lesions.
- Stepwise removal can be used for deep lesions and combines various strategies, but there is debate about whether this should still be performed.
Another strategy Dr. Schwendicke discussed was not removing any carious tissue, as studies have confirmed the importance of preserving pulpal integrity and the reduction in pulpal exposure risk with less removal. This can include sealing shallow, noncavitated carious lesions using resins or nonrestorative cavity control, which involves opening up the lesion and regularly cleaning it and is not supported by sufficient evidence.
"Less invasive excavation retains teeth significantly longer and avoids endodontic treatment, thereby reducing treatment costs dramatically (up to 50%)," Dr. Schwendicke wrote.