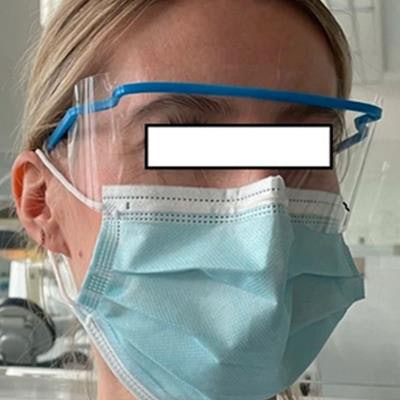
Blood and saliva droplets that are invisible to the naked eye can be found on protective eyewear worn by dental professionals after treating patients, according to a study published online February 14 in Clinical Oral Investigations.
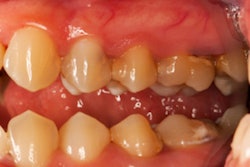
Tooth cleanings that were performed with air scalers resulted in the highest amount of blood splatter compared to other aerosol-generating procedures, the authors wrote.
"To prevent the conjunctiva from blood and saliva splashes, adequate protection of the eyes is necessary for the dental professionals," wrote the group, led by Dr. Nora Bergmann from Heinrich-Heine University in Düsseldorf, Germany.
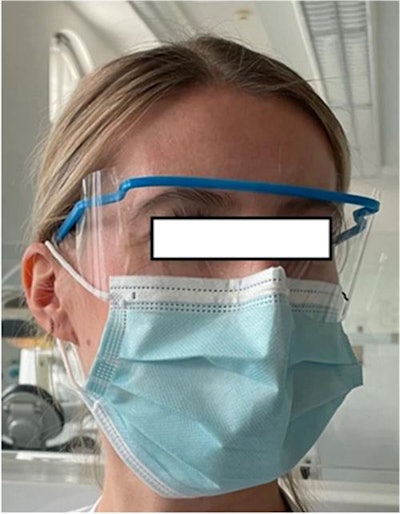 Protective eyewear worn by a participant prior to performing dental treatment. Image courtesy of Bergmann et al. Licensed under CC BY 4.0.
Protective eyewear worn by a participant prior to performing dental treatment. Image courtesy of Bergmann et al. Licensed under CC BY 4.0.Clinicians and their teams have always been at risk of exposure to blood and saliva aerosols while treating patients. Since the COVID-19 pandemic began, the issue has received much more attention, and dentistry has implemented new safety protocols, such as the use of additional personal protective equipment. What's more, the U.S. Centers for Disease Control and Prevention recommended that ultrasonic scalers not be used during the pandemic.
The researchers set out to explore the discernable contamination of protective eyewear worn by dental team members during aerosol-generating procedures and the effectiveness of subsequent disinfection. They used common forensic techniques to evaluate 53 eye shields worn by dentists, students, and dental assistants.
The shields were worn during procedures, including supragingival cleaning, carious cavity preparation, and subgingival periodontal instrumentation, and team members used evacuation systems during treatment. To detect blood, luminol was applied to the eyewear and analyzed.
Macroscopically detectable contamination from blood and saliva was found on about 60% of protective eyewear surfaces that dental team members wore while treating patients, the authors wrote.
Of the aerosol-generating procedures performed, the highest amount of blood (median, 1,087 pixels) was observed after dental professionals used air scalers to clean patients' teeth. This was followed by scaling and root planing, which had a median of 924 pixels. Endodontic and restorative therapy procedures had a very low pixel count, they found.
The authors noted a limitation of the study: Disposable shields were used and disinfected like reusable shields because this was a pilot study that was testing detection of contamination under standardized conditions. In the future, similar studies should be performed to test reusable safety glasses and magnification glasses, they wrote.
Because SARS-CoV-2 can be transmitted through indirect or direct eye contact, dental teams remain at high risk.
"It should be considered to recommend facial shields as standard personnel protective equipment for every aerosol-promoting dental treatment in post-pandemic time," Bergmann and colleagues concluded.