Several studies published this summer showcase the potential for magnetic resonance imaging (MRI) as a hard- and soft-tissue diagnostic tool in dentistry, and research groups in Germany are leading the way.
Two presentations at the Computer Assisted Radiology and Surgery (CARS) meeting in Berlin in June focused on the use of MRI for assessing carious lesions and acute periodontitis. And a recent study in European Radiology (July 31, 2011) compared MRI's ability to visualize dental and periodontal structures with that of multidetector CT and cone-beam CT.
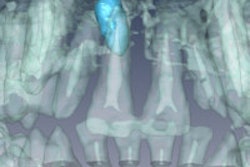
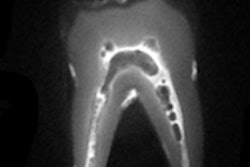
At the CARS meeting, researchers from University Hospital of Ulm and the University of Ulm presented results from a 40-patient feasibility study that investigated the applicability of MRI for the in vivo identification of carious lesions.
The patients underwent a conventional clinical dental exam (including an x-ray), followed by a dental MRI exam within 14 days. The patients were selected randomly and already had various dental restorative materials, including gold, ceramic, amalgam, composites, and crowns, in their mouths.
All MRI exams were performed on a 3-tesla whole-body MRI system (Achieva, Philips Healthcare), and data were acquired twice with a prototype two-element carotid artery coil (120 x 50 mm). The scan times were 5:32 and 7:49 minutes, respectively.
The MRI protocol was completed in 37 of the patients, and a total of 157 lesions were identified. Of these, 137 lesions (85%) were clearly identifiable in the x-rays. Some occult occlusal lesions and secondary lesions were visible only in the MR images.
When the MR and x-ray images were compared and the lesion parameters quantified, there was a significant (p < 0.5) underestimation of the lesion dimensions by the x-rays, the researchers noted.
"The application of ultrashort echo-time MRI appears feasible for identification of caries lesions with high sensitivity," they wrote. "In direct comparison to x-ray techniques, MRI may be able to identify the real extent of the lesions instead of showing the areas with substantial breakdown of the local mineral structures only."
Further clinical evaluation is needed to determine whether the limited spatial resolution and prolonged acquisition times will hinder the routine use of MRI for caries diagnostics, they added.
Assessing periodontal disease
In a related presentation, the same team studied the use of MRI for assessing acute periodontitis, including the 3D structure of related bone degeneration.
"While bone resorption can nicely be assessed by x-ray-based imaging methods such as conventional orthopantomography or volume tomography, acute and chronic inflammation can hardly be distinguished due to the limited soft-tissue contrast in x-rays," the researchers wrote.
“Dental diagnostic imaging should not be viewed as being only
x-ray.”
— Allan Farman, BDS, MBA, PhD, DSc
The study included 10 patients with clinically proven periodontitis and 10 patients with clinically proven apical periodontitis. All patients had multiple dental restorations, including amalgam, gold, ceramic, and composite fillings, and crowns and bridges.
Patients first underwent preparation scans, followed by a series of turbo spin-echo (TSE) scans and high-resolution multislice T2-weighted TSE scans. The scans were taken using the same whole-body MRI system used in the previous study, and the results were compared with a bitewing or 2D or 3D x-ray. Location and size of the lesion and/or bone resorption visible in the MR images were qualitatively compared with those in the x-rays.
Including planning, the entire patient exam was conducted in less than 45 minutes for all patients, the researchers noted. Acute inflammation and bone resorption could be clearly identified in the MR images. In patients with periodontitis, the MRI data allowed the researchers to visual the course of the cortical bone and distinguish between bone resorption that appears only on the lingual or buccal side of the mandible.
In patients with apical periodontitis, acute inflammation could be distinguished from chronic inflammation in the MRI data, and the respective bone resorption could be quantified.
The more accurate geometrical assessment of the 3D structure of the inflammation and bone resorption may improve diagnosis and treatment monitoring in periodontitis, the study authors concluded.
"These were nice, cutting-edge clinical trials showing a potential for the future when technology possibilities grow to meet ideas," commented Allan Farman, BDS, MBA, PhD, DSc, a professor of radiology and imaging science at the University of Louisville in Kentucky and president of the American Academy of Oral and Maxillofacial Radiology.
Comparisons with CT
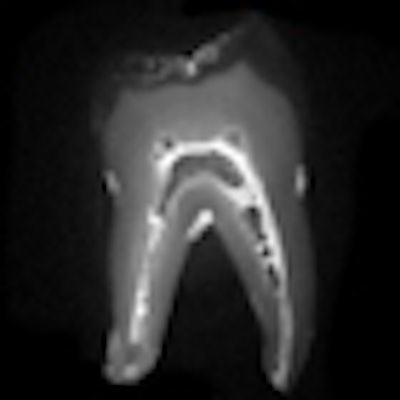
The European Radiology study further supports these findings. Researchers from University Hospital Heidelberg and University Campus Bio-Medico of Rome examined four porcine mandibles with MRI, microdetector CT, and cone-beam CT.
Two observers independently reviewed the images and assessed the image quality of different dental and periodontal structures. While all dental structures were imaged accurately with all imaging sources, periodontal space and cortical/trabecular bone were better visualized by MRI (p < 0.001), the researchers noted. In addition, MRI displayed the lamina dura "excellently," while this feature was not detectable with microdetector CT and was only inconsistently visible with cone-beam CT (p < 0.001).
"This experimental study shows the diagnostic feasibility of MRI in visualization of teeth and periodontal anatomy," the study authors wrote. "Detection of periodontal structures was significantly better with MRI than with MDCT or CBCT."
Further trials are needed to fully evaluate the potential benefit of MRI in a clinical setting, they added.
"Dental diagnostic imaging should not be viewed as being only x-ray," Dr. Farman said. "MRI and ultrasound are other technologies showing much promise, and without ionizing radiation."