Obstructive sleep apnea (OSA) is a common medical disorder characterized by repetitive episodes of upper airway collapse during sleep. Recent prevalence estimates have suggested that 26% of U.S. adults between the ages of 30 and 70 have the disorder. Obstructive sleep apnea has been determined to be a causative factor in the development of numerous other medical diseases including, hypertension, heart disease, stroke, type 2 diabetes, depression, headaches, and acid reflux.
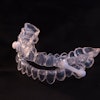
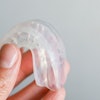
The pathophysiology of OSA is depicted in the images below.
 Above: Drawing of unobstructed airflow in a patient. Below: Drawing of an obstructed airflow in a patient. Images courtesy of Dr. Joseph Krainin.
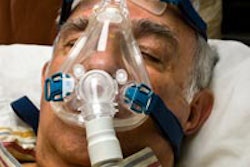
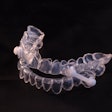
Above: Drawing of unobstructed airflow in a patient. Below: Drawing of an obstructed airflow in a patient. Images courtesy of Dr. Joseph Krainin.Dentists increasingly are finding themselves on the front line of OSA detection and treatment. Continuous positive airway pressure (CPAP) is considered the gold standard treatment for OSA, but low compliance rates have created an enormous market for alternative sleep apnea treatments. As public awareness of oral appliances for sleep apnea therapy has increased, patients are presenting to dental practices seeking an appliance.
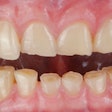
Additionally, dentists frequently identify risk factors for sleep apnea during routine examinations. These include physical findings such as a small airway, high arched palate, overjet, crossbite, and retrognathia. A patient may also have pathological dental findings related to OSA, such as bruxism-related wear and enamel erosion from acid reflux.
As dentists' involvement in this field expands, understanding key sleep medicine practice guidelines is important to remain in compliance with these recommendations.
Guidelines
The most important guideline for dentists to be familiar with is the American Academy of Sleep Medicine's "Practice Parameters for the Treatment of Obstructive Sleep Apnea and Snoring with Oral Appliance Therapy: An Update for 2005" (available here). The salient points are listed below:
 Joseph Krainin, MD, founder of Singular Sleep.
Joseph Krainin, MD, founder of Singular Sleep.- The presence of OSA and its severity must be established with a sleep apnea test before initiation of oral appliance therapy.
- Treatment goals include resolution of symptoms and also normalization of the Apnea-Hypopnea Index (AHI) value (AHI < 5) and oxyhemoglobin saturation as shown on a follow-up sleep study.
- Patients with severe OSA (AHI > 30) require an initial CPAP trial prior to consideration for an oral appliance.
- OSA patients treated with an oral appliance should have periodic follow-up with a sleep physician to assess for signs and symptoms of worsening apnea.
From the guidelines, it is clear that it is essential for dentists to develop a collaborative relationship with a sleep physician.
"Close communication [between the sleep physician and] the dentist is most conducive for good patient care," the academy wrote.
Best practices are for dentists to obtain two sleep studies in the course of the treatment plan: the initial diagnostic sleep study and a repeat one with the oral appliance after optimal mandibular protrusion has been achieved.
Involvement of a sleep physician will be necessary in managing severe OSA patients and also more complex patients requiring "hybrid therapy," that is, oral appliance therapy plus positive airway pressure (PAP), or oral appliance therapy plus positional therapy. Optimal patient outcomes are achieved when the dentist has easy access to a sleep medicine clinic to facilitate seamless patient care.
Sleep telemedicine
Telemedicine can be broadly defined as the practice of medicine in which the provider and patient are separated by place. Studies indicate that Americans are open to seeing their providers online; a 2015 Harris Poll showed that 64% of adults were willing to have a telemedicine visit.
Telemedicine is of particularly high utility in sleep medicine, given that specific physical examination findings are not part of the diagnostic criteria for any sleep disorder. Data can now be transferred from a patient's CPAP machine to a provider over a wireless network. The ascendancy of home sleep testing is synergistic with sleep telemedicine consultations, and it facilitates the comprehensive management of sleep disorders, such as sleep apnea, without the patient ever being required to set foot in a sleep clinic or spend a night in a sleep lab.
Patients can participate in sleep telemedicine consultations at a referring provider's clinic or at the location of their choosing. All that is required for a patient to have a sleep telemedicine consultation is a tablet, smartphone, computer with a webcam, and an internet connection. On the provider's end, the interaction must take place through a secure, HIPAA-compliant software platform.
Potential benefits for dentists
When managed effectively, the logistical simplicity of a sleep telemedicine practice enables the rapid diagnosis of sleep apnea, which will facilitate dentists' practice. In many areas of the country, wait times in excess of several weeks to months for both in-lab sleep studies and sleep doctor clinic appointments are not uncommon. In our sleep telemedicine practice, average time to book a new consultation is two to three days and sleep study results are usually available to the referring provider in seven to eight days.
“The potential synergy between dentists and sleep telemedicine clinics could enhance patient outcomes in both practices.”
Prolonged wait times aren't the only barrier to care that a sleep telemedicine practice may help overcome. Local sleep labs generally attempt to schedule patients for in-lab sleep studies. However, our experience is that patients who enter dental practices to obtain an oral appliance who are unaware that they need a sleep study are often resistant to in-lab studies. Such patients are usually more amenable to a home sleep test because of the comfort and convenience of home-based testing.
Additionally, for some patients, cost may be a roadblock to getting the help that they need. Because of reduced overhead, sleep telemedicine clinics may be able to pass on the savings to patients, and they offer sleep apnea testing and physician consultations at more affordable rates than traditional brick-and-mortar sleep centers. Telemedicine consultations can be an affordable way to provide the "face-to-face" encounter that many insurers require to pay for the oral appliance.
A good referring relationship between a dentist and sleep telemedicine clinic has the potential to be bidirectional. Not only do dentists need easy access to affordable and expedited sleep apnea diagnostics and the ability to offload more complex sleep apnea patients, but the sleep medicine physician needs experienced dentists to refer patients with mild-moderate obstructive sleep apnea who prefer an oral appliance, as well as patients with severe sleep apnea who have failed, or decline, CPAP. The potential synergy between dentists and sleep telemedicine clinics could enhance patient outcomes in both practices.
Joseph Krainin, MD, is a board-certified sleep medicine physician, fellow of the American Academy of Sleep Medicine, and founder of Singular Sleep, a comprehensive sleep telemedicine center.
The comments and observations expressed herein do not necessarily reflect the opinions of DrBicuspid.com, nor should they be construed as an endorsement or admonishment of any particular idea, vendor, or organization.