Antidepressants are associated with higher rates of dental implant failure, according to the findings of a new study presented at the recent American Association of Dental Research (AADR) meeting in Los Angeles.
The use of both antidepressants and dental implants in the U.S. has increased exponentially during the last decade, noted the researchers from the University at Buffalo (UB) School of Dental Medicine. Antidepressants have been shown to affect bone metabolism, and patients on antidepressants and antipsychotics are more likely to develop xerostomia, according to multiple studies (Journal of Dental Research, November 2014, Vol. 93:11, pp. 1054-1061; Anesthesia Progress, Fall 2008, Vol. 55:3, pp. 89-99).
"Antidepressants are the second most prescribed drug in this country, and there are millions of implants placed every year around the world, so this applies everywhere, not just the U.S.," researcher Sebastiano Andreana, DDS, an associate professor and the director of implant dentistry at the UB School of Dental Medicine), told DrBicuspid.com.
Antidepressants increase implant failure
The retrospective study analyzed 74 patients (41 women) who were 18 and older and received dental implants at the UB dental clinic between January 2014 and August 2014. The number of implants received per patient ranged between one and 11. The average implant failure rate is 5%, the researchers said.
| Number of implants per patient in study | ||||||
| Number of implants | 1 | 2 | 3 | 4 | 5 | 11 |
| Number of patients | 44 (57.9%) | 20 (26.3%) | 5 (6.6%) | 3 (1.3%) | 3 (1.3%) | 3 (1.3%) |
Sulochana Gurung, a student researcher at UB who presented the findings at the AADR meeting, said the study also evaluated other factors, including smoking status, alcohol use, and medical conditions, such as depression, diabetes, osteoporosis, HIV, and cardiovascular disease.
The frequency of antidepressant use was higher in patients who experienced implant failure (33.3%) compared with those who did not (11.3%), the researchers found.
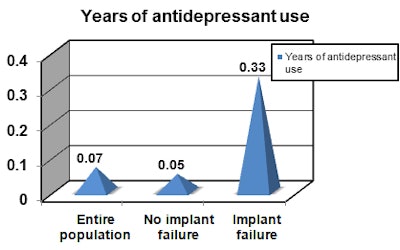 Above: Implant survival and failure in patients, years of antidepressant use. Below: Percentage of implant survival and failure in patients with antidepressant use. Charts courtesy of Sulochana Gurung and Drs. Latifa Bairam and Sebastiano Andreana.
Above: Implant survival and failure in patients, years of antidepressant use. Below: Percentage of implant survival and failure in patients with antidepressant use. Charts courtesy of Sulochana Gurung and Drs. Latifa Bairam and Sebastiano Andreana.The odds of implant failure among antidepressant drug users were about four times higher compared with controls (odds ratio [OR] = 3.93, 95% confidence interval [CI]: 0.61-25.51). Each year of antidepressant use was associated with a twofold increase in the odds of implant failure (OR=2.18, 95% CI: 0.68-7.02). The frequency of depression itself was not associated with implant failure.
Dr. Andreana said he wasn't surprised by the findings since three previous studies reported similar results regarding implant failure. The prior UB and Canadian studies led the researchers to focus on the patients who have had implants in UB's dental clinic.
"It became more and more obvious that there was a relationship," Dr. Andreana said.
Researcher Latifa Bairam, BDS, a clinical assistant professor in the UB Department of Restorative Dentistry, said many patients who were treated at the school's dental clinic were taking antidepressants.
"In clinical observations, we noticed a high percentage of dental patients are on antidepressants or selective serotonin reuptake inhibitors (SSRIs), so that encouraged us to look at this in detail," she said. "Many are on one or two different kinds of antidepressants or antipsychotics. But they all affect bone biology and bone density, and it can produce teeth clenching and dry mouth; all these things are related."
Clenching puts a lot of pressure on teeth and implants. Excessive force on implants isn't good for them, Dr. Bairam noted.
Another side effect of antidepressants is akathisia, the need to be in constant motion, which also causes teeth grinding, the study authors noted.
Patients' needs should be assessed
Dr. Bairam stressed that patients don't have to discontinue taking antidepressants before they get implants.
 From left to right: Latifa Bairam, BDS; Sulochana Gurung, student; Sebastiano Andreana, DDS. Image courtesy of the UB School of Dental Medicine.
From left to right: Latifa Bairam, BDS; Sulochana Gurung, student; Sebastiano Andreana, DDS. Image courtesy of the UB School of Dental Medicine."For patients who have been on antidepressants a long time, we're not telling them to quit their medication," she told DrBicuspid.com. "We just want them to be aware -- the dentist, patient, and physician. It's cooperation between all the parties to manage the procedure. That decision has to be made by the patient's physician to assess the patient's needs. You just have to be careful and watch; it's a risk factor."
When working with the dentist or oral surgeon, long-term monitoring should be done to note side effects, Dr. Bairam said. Also, patients should understand the need for follow-up and the necessity of lab tests to establish a baseline when the medication starts and over time at regular intervals to implement long-term prevention and treatment, she said.
"It would really be useful if patients provided the dentist with a current picture of lab tests, which would be helpful in treatment planning for the placement of the implant," Dr. Bairam said.
One of the most important is a bone density test to analyze signs of osteoporosis, among the biggest factors affecting the quality of bone at the implant recipient site, she said.
"The findings weren't really a big surprise, but it's one thing to read about it and it's another to see research findings for yourself," Dr. Andreana said. "So this was a confirmation of what others have reported."
The study's results need to be confirmed by larger prospective studies, Dr. Bairam said, and UB researchers are planning to analyze a target population of 1,200 patients who received implants between 2007 and 2014.
"We don't want to scare dentists or patients, but this study and others confirm that there is some association between antidepressants and implant failure," Dr. Andreana said. "This is a wakeup call."