In the future, the timing of dental implant placement may shift from a fixed approach to one that is more flexible and tailored to each patient. The study was recently published in the Journal of Periodontal Research.
Furthermore, clinicians may be inclined to follow an evidence-based approach that prioritizes placing implants as early as safely possible, the authors wrote.
“Implant placement timing will evolve from a rigid, schedule-based paradigm to a dynamic, biologically informed, patient-centered process,” wrote the authors, led by Dr. Daniel S. Thoma of the University of Zurich Center of Dental Medicine in Switzerland (J Periodontal Res, February 11, 2026).
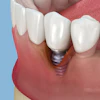
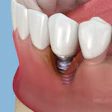
The researchers developed a clinically focused perspective article examining how implant timing concepts have evolved, reviewing current evidence-based practices, and assessing trends that could reshape future approaches. Historically, protocols favored delayed placement, with implants inserted three to six months after extraction to allow complete bone healing and reduce infection risk, they wrote.
This approach became the gold standard because clinicians prioritized infection control, full socket healing for optimal bone density and stability, and the limitations of early smooth-surfaced implant designs. The International Team for Implantology classification system outlines four timing categories from immediate to late placement, but real-world clinical decisions often extend beyond these structured definitions due to patient-specific and aesthetic considerations.
Future implantology is expected to move away from set timing categories to a more personalized, biologically guided approach. Instead of following set timelines, clinicians will increasingly base implant placement on individual anatomical, biological, and aesthetic factors, supported by digital diagnostics and advanced biomaterials, they wrote.
Additionally, regenerative technologies such as growth factors, bioactive scaffolds, and soft-tissue enhancement techniques are improving bone and tissue healing, particularly in postextraction sites. As innovations advance, healing time may become a controllable variable, with implant timing guided more by real-time tissue conditions and patient risk profiles than by predetermined intervals.
“The art lies in knowing when to accelerate treatment to meet patient requests and when to slow down to respect biological healing achieving the delicate balance between efficiency and predictability,” Thoma and colleagues concluded.