A 54-year-old healthy woman was diagnosed with a rare case of infective endocarditis after developing an acute ischemic stroke five weeks after having a tooth extracted. The case report was published on January 24 in the Journal of the American Dental Association.
The woman, who recovered after a weeklong stay at the hospital plus six weeks of IV antibiotics, had not been prescribed prophylactic antibiotics for the tooth extraction procedure because she was considered at low risk for developing infective endocarditis. Due to her infective endocarditis infection, she will be considered high risk, requiring antibiotic prophylaxis for invasive dental procedures in the future, the authors wrote.
“Despite her initial low-risk assessment, our patient ultimately developed infective endocarditis as a result of the dental procedure,” wrote the authors, led by Dr. Zachary Wilseck, a clinical assistant professor at the department of radiology at the University of Michigan Medical School in Ann Arbor.
A woman with a cracked tooth
The woman, with no underlying health conditions, cracked tooth #30 while chewing a popcorn kernel. Her dentist extracted the tooth. The woman experienced persistent pain at the site for two weeks but did not inform her dentist. Also, the dentist did not conduct any follow-up calls with her. Once the pain subsided, the woman began experiencing progressive fatigue, according to the report.
About five weeks after her tooth was pulled, the woman was taken to the emergency department after she was having trouble speaking and the right side of her face was drooping.
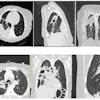
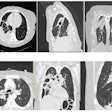
She underwent a computed tomographic angiography that showed a left segment middle cerebral artery occlusion “with reconstitution of the distal middle cerebral branches through arterial collaterals.” The blood clot was successfully removed, and her language and neurological deficits improved. Additional imaging revealed deep hemorrhages in the brain, they wrote.
Her blood tested positive for the common oral cavity bacteria Streptococcus mitis, resulting in her being diagnosed with infective endocarditis believed to have been caused by the dental procedure. The patient was started on antibiotics.
Though she remained asymptomatic for endocarditis, an echocardiogram revealed aortic insufficiency and mitral valve vegetation and regurgitation, the authors wrote.
The woman continued to take antibiotics, and she was released on day seven of her hospital stay. She was told to continue patient daily ceftriaxone infusions for six weeks.
Things to consider
Dental procedures like tooth extractions have been linked with transient bacteria that allow oral germs into a patient’s bloodstream. Most patients successfully clear the bacteria, but those who are immunocompromised, have heart conditions, including valvular abnormalities, are an increased risk of developing endocarditis, according to the report.
Based on American Heart Association guidelines, the woman in this case would have been considered low risk for developing endocarditis. This was based on her not having past cardiac issues, joint replacements, advanced gum disease, or diabetes. Also, she didn’t smoke, drank minimal amounts of alcohol, and had no chronic diseases.
“The temporal relationship between the tooth extraction and the subsequent development of infective endocarditis and stroke in our patient raises important considerations regarding the role of oral health and invasive dental interventions in the pathogenesis of systemic infections and cerebrovascular events,” Wilseck and colleagues wrote.