Do you know the best practices for managing recurrent endodontic issues? Researchers of a new study found that individual practitioners often changed their minds regarding treatment of specific cases, and they discovered significant differences in decision-making among types of dentists.
The researchers sent a survey on treatment decisions for nonhealing periapical lesions to general practitioners, endodontists, and other specialists who had completed the same survey seven years earlier. They found that significant differences among the groups in their treatment recommendations held steady over time.
"The results of this study suggest that great inconsistencies still exist between different practitioner groups and with regard to practitioner reliability," the authors wrote (Journal of Endodontics, December 16, 2017).
The lead study author was Lorel Burns, DDS, then an endodontic resident at the University of Pennsylvania School of Dental Medicine in Philadelphia and now an endodontics instructor at the New York University College of Dentistry and an endodontist at Apex Endodontics in the Nashville, TN, area.
More education needed
The researchers conducted the study to gain a better understanding of interdisciplinary variations in clinical decision-making for nonhealing endodontic cases. Secondarily, they sought to determine any potential changes in treatment planning by assessing intraspecialty and intrapractitioner treatment decision reliability over time.
“Great inconsistencies still exist between different practitioner groups and with regard to practitioner reliability.”
The study's first part involved a web-based survey that was sent in 2009 to 2,419 members of the Pennsylvania Dental Association about treatment decisions for 14 deidentified endodontically treated cases with various coronal restorations and nonhealing apical periodontitis. In 2016, the researchers emailed a link to the same online survey to the previous respondents.
They selected the cases of three anteriors, five premolars, and six molars from the Endodontic Residency Program at the University of Pennsylvania. They represented four different restoration types depending on the presence or absence of a post and whether there was permanent full coronal coverage: no crown-no post, no crown-post, crown-no post, and crown-post.
For each case, study participants were told to choose, without regard to economic considerations, one of the following treatment options:
- Wait and observe
- Nonsurgical retreatment
- Surgical retreatment
- Extraction and fixed partial denture
- Extraction and implant.
In 2009, 262 dentists responded and were included in the study. In 2016, 104 (39.7%) of those respondents completed the survey again: 69 were general practitioners, 15 were endodontists, and 20 were specialists (periodontists, prosthodontists, or oral surgeons).
The researchers found significant differences in the treatment types chosen among the general practitioner, endodontist, and specialist groups in 2009. However, they discovered no statistically significant changes in treatment planning choices between 2009 and 2016 for those practitioners who responded both times, as well as for the smaller subsets of the general practitioners, endodontists, and specialists who also did so.
| Treatment decisions by practitioner group | ||||||
| General practitioner | Specialist | Endodontist | ||||
| Treatment decision | 2009 | 2016 | 2009 | 2016 | 2009 | 2016 |
| Wait and observe | 6.7% | 6.7% | 8.9% | 5.7% | 3.9% | 4.8% |
| Nonsurgical retreatment | 34.2% | 34.2% | 18.9% | 16.1% | 41.1% | 42.3% |
| Surgical retreatment | 27.2% | 29.9% | 31.8% | 29.8% | 44.3% | 42.3% |
| Extraction and fixed partial denture | 4.9% | 4.2% | 3.2% | 2.1% | 1.4% | 1.0% |
| Extraction and implant | 27.0% | 24.9% | 40.4% | 43.2% | 9.3% | 9.7% |
On an individual level, 760 treatment decisions remained the same and 696 changed, with an almost 48% chance of a change in the original decision. The chances of changing treatment planning decisions between 2009 and 2016 among the three practitioner groups were significantly different (p < 0.05), with general practitioners changing 50.3% of the time, endodontists 37.6%, and specialists 46.8%.
Among the 14 cases, the chances of changing the treatment planning decision ranged from 37.5% for a case with a post and no crown to 62.5% for a case with both a post and crown. Tooth-saving versus replacement treatment decisions remained similar between 2009 and 2016, with nonsurgical or surgical treatment representing 63.8% of decisions in 2016.
The team found significant differences among the practitioner groups by tooth type. For anteriors, endodontists and general practitioners chose nonsurgical treatment more frequently than the other options, while specialists more frequently chose extraction and implant.
For premolars, endodontists and general practitioners chose nonsurgical or surgical treatment more frequently, and while endodontists made the same choices for molars, general practitioners and specialists preferred extraction and implant.
The results for general practitioners could indicate a lack of awareness of the successful outcomes of modern endodontic surgery, even in molar areas, the authors noted. While no significant technical changes have occurred in clinical endodontic practice or implant therapy between 2009 and 2016, published studies during that period have provided more information on outcomes, they wrote. This has resulted in suggestions that extraction and replacement strategies be reconsidered in favor of keeping natural teeth.
"It appears that despite new evidence becoming available, no changes in the overall treatment planning trend for nonhealing endodontic cases occurred in this group of practitioners," the authors wrote.
New graduates, technology excluded
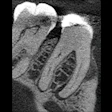
The researchers noted that their results had some limitations. The study included only clinicians who were practicing in both 2009 and 2016, which excluded recent graduates, who might be more likely to be exposed to newer information. Additionally, cone-beam CT images, which have become widely accepted but were not in 2009, were not included in the survey and might have facilitated decision-making.
Nevertheless, the authors emphasized the need for practitioners to expand their knowledge of best practices for the treatment of endodontic problems.
"These findings demonstrate that updated treatment planning guidelines and further education regarding the treatment planning [for] endodontic cases with recurrent or persistent disease [are] needed for practicing clinicians," they concluded.