The authors of new review published in the Journal of Dental Research (April 3, 2014) hope to increase the understanding of dental, oral, and craniofacial manifestations of rare bone diseases and improve the ability to diagnose and treat these conditions. They identify four physiologic processes that cause these diseases and detail their dental manifestations.
While hereditary diseases affecting the skeleton are individually rare, the total number of people affected is great, according to the National Organization for Rare Disorders and the Rare Bone Disease Patient Network.
Researchers from various institutes of the National Institutes of Health; the Children's National Medical Center in Washington, DC; the department of the pediatric dentistry at the University of North Carolina at Chapel Hill School of Dentistry; and the department of oral medicine at the University of Pennsylvania School of Dental Medicine came together to review four key physiologic processes in bone and tooth formation, focusing on the dental, oral, and craniofacial manifestations of rare bone diseases when these processes go "awry."
Noting that the "rarity and lack of in-depth reporting" of these conditions limit their understanding and the ability to diagnose and treat patients, the authors stated that their goal is to "improve the identification of genetic, molecular, and/or biologic causes; diagnoses; and treatment of these and other rare bone conditions that may share underlying mechanisms of disease."
In their report, the researchers discussed mechanisms of how bone and tooth functions are negatively affected. If such dysfunction can be labeled, perhaps this labeling can be used to improve the identification of various causes of additional diseases because of similar skeletal and dental etiopathologies.
Breaking down the 4 processes
The authors reviewed the four processes of stem/progenitor cell differentiation, matrix function, mineralization disorders, and bone resorption.
“Only through this careful approach can we ... provide answers and appropriate care to individuals suffering from conditions that have eluded diagnosis.”
Defective stem/progenitor cell differentiation can cause fibrous dysplasia (FD) of bone. The dental disorders associated with FD include enamel hypoplasia and hypomineralization, dentin dysplasia, odontoma, taurodontic pulp, and high caries index. Taurodontism seen in FD may be the combined effect of FD and endocrine dysfunction, according to the authors. There can be extensive expansion of the skull, maxilla, and mandible, tooth displacement, severe malocclusion, and facial disfigurement in FD, they noted.
The authors then looked at defective matrix production and osteogenesis imperfecta (OI), which is a group of hereditary disorders characterized by variable bone fragility. Affected individuals have decreased bone mineral density, an increased fracture risk, deformations, short stature, kyphoscoliosis, craniofacial deformities, and a tooth phenotype resembling dentinogenesis imperfecta (DI).
"Teeth tend to be smaller than normal, and feature constriction at the cementum-enamel junction, diminished roots, blue-gray to yellow-brown discoloration, and pulp chambers that are progressively diminished and appear obliterated on radiographs," they wrote.
When DI is present, management of the dentition depends on the condition's severity and also whether enamel fracturing is present, resulting in excessive tooth breakdown, the authors wrote. Crowning of the teeth is the preferred treatment, they stated, as intracoronal restorations are not retained in DI teeth with enamel loss and excessive dentin loss.
Mineralization disorders and bone resorption
Mineralization disorders can cause familial tumoral calcinosis/hyperostosis-hyperphosphatemia syndrome (FTC/HHS), hypophosphatemic rickets, and hypophosphatasia. The authors noted that dental findings of FTC/HHS include short bulbous teeth, shortened roots, root dilacerations, thistle-shaped dental pulps, pulp chamber and root canal obliteration, and pulp stones. Radiographs of younger individuals suggest that abnormal calcification of the pulp occurs before root formation, they wrote, adding that, histologically, the root phenotype resembles dentin dysplasia II, but the timing of calcification is different.
Finally, the authors discussed the rare bone disease involving bone resorption, Gorham-Stout disease. "Histopathologically, the disease is a benign vascular proliferation of endothelial channels within bone, leading to extreme thinning of bony trabeculae, osteoclast-mediated resorption, and replacement of bone with fibrous tissue," they stated. Dentoalveolar findings include mobile teeth, malocclusion, mandibular deviation, bony deformity, and pathologic fractures.
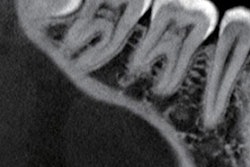
Panoramic radiographs and CT scans are preferred for monitoring disease progression in the maxillofacial region, according to the authors. Tooth loss may result from reduced alveolar bone, but tooth resorption has not been reported.
Conclusion
The formation and function of the skeleton and dentition are compromised when defects arise in from any of the four processes, the authors concluded. They note that practitioners should be aware of these conditions and that these patients should be referred to a craniofacial/dental team for clinical evaluation, the collection of clinical materials for translational studies, the monitoring of development over time, and treatment.
The authors emphasized that "only through this careful approach can we accomplish three issues of paramount importance": provide answers and appropriate care to patients with conditions that have eluded diagnosis, advance medical knowledge about rare skeletal and dental diseases, and develop and improve treatments.