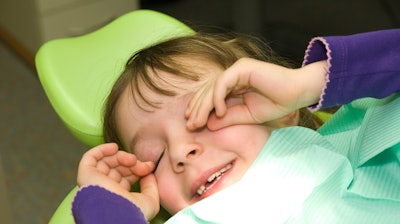
More than a half dozen behaviors, including tensed eyelids and no vocalizations, indicate that pediatric dental patients are experiencing delirium as they awaken from anesthesia, according to a study published on April 25 in Pediatric Anesthesia.
Identifying which behaviors are indicative of true emergence delirium (ED) will prevent misclassification. Currently, the diagnostic criteria for emergence delirium are sensitive but not specific, the authors wrote.
“These discriminators may be used to develop a scale that will lead to better diagnosis and treatment of emergence delirium,” wrote the report's authors, led by Dr. Jennifer O’Brien of the department of anesthesiology at the University of Saskatchewan in Canada.
When patients awaken from general anesthesia, an acute condition known as emergence delirium may occur. This condition has been characterized by restlessness with nonpurposeful movements, including thrashing, and can result in injuries to patients and caregivers. Typically, emergence delirium lasts fewer than 45 minutes, but four cases lasting two days have been reported in the literature.
The observational study comprised 154 patients between the ages of 20 months and 9 years old. The children were recorded upon waking from general anesthesia, resulting in 153 close-up and 151 full-body recordings. To identify the patients’ behaviors, 10 anesthesiologists, 12 anesthesiology residents, three pediatric dentists, and four recovery room nurses rated each 10-second video segment, according to the study.
After viewing the recordings, the experts agreed that 33 patients presented true emergence delirium. Then, three research assistants independently completed behavior checklists for the 33 patients and matched controls, they wrote.
The following eight behaviors were characterized as true emergence delirium:
- Tensed eyelids
- Restrained arms
- Inwardly furrowed eyebrows
- No vocalizations
- Kicking
- Squirming, shifting back and forth, tense
- Uneasy, restless, tense legs
- Mouth open and squared
The study had several limitations. While the study accounted for duration, the duration of any behavior needed for a diagnosis of emergence delirium was not considered, the authors wrote. In the future, the discriminators identified may be used to develop a scale that may be more specific for emergence delirium, they wrote.
“By determining which behaviors are most prevalent, we might begin to develop a scale to discriminate true ED from non-true ED that will lead to better diagnosis of this phenomenon, and eventually better treatment,” O’Brien et al wrote.