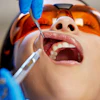
One reason patients cite for avoiding dental treatment is fear of pain during and after a procedure. Researchers from the U.K. conducted a comprehensive review to see if one injectable anesthetic worked better than others in different clinical situations.
All of the injectable anesthetics in the included studies appeared effective and safe, but one stood out for surgical procedures, the researchers found. However, they noted that available evidence ranged from moderate to very low in quality. The review was published on July 10 in the Cochrane Database of Systematic Reviews.
"The review suggests that of the 14 types of local anesthetic tested, evidence to support the use of one over another is limited to the outcome of success (absence of pain), from three comparisons of local anesthetic," wrote the authors, led by Geoffrey St. George, BDS, of the endodontics unit at the Eastman Dental Hospital in London.
What constitutes success?
Several different local, injectable anesthetics are available to dentists. The researchers investigated whether injection of one local anesthetic solution was more effective than another for preventing pain either during dental treatment or an experimental study.
The researchers took a comprehensive look at three aspects of anesthetic pain management to see if they could make a recommendation:
- The success of pain management with anesthesia
- The speed of onset and duration
- Systemic and local adverse effects among different local anesthetic formulations
They winnowed more than 120 studies down to 68 studies with over 6,600 participants for analysis:
- There were 23 comparisons of local anesthetic.
- There were 57 outcomes with 14 different anesthetic formulations.
- There were only 10 outcomes from eight comparisons involving clinical testing.
While the studies tested 14 different local anesthetics, evidence to support the use of one over another was limited to the outcome of absence of pain from three comparisons of local anesthetic.
One study found that 4% articaine, 1:100,000 epinephrine was superior to 2% lidocaine, 1:100,000 epinephrine in posterior teeth with irreversible pulpitis requiring root canal treatment. In this study, no difference between these solutions was seen when pain on injection was assessed. Lidocaine resulted in less postinjection pain, but the difference was minimal.
Two randomized controlled studies, both using a parallel design, showed that 2% lidocaine, 1:100,000 epinephrine was superior to 3% prilocaine, 0.03 international units (IU) of felypressin for teeth and dental tissues requiring surgical procedures and superior to 4% prilocaine plain for surgical procedures along with periodontal treatment.
However, for studies concerning the success of other anesthesia for teeth requiring surgery and those requiring extraction, the review authors noted that results were uncertain no matter which anesthetic was used.
No clinical studies met the authors' outcome definitions for comparisons assessing onset and duration.
For adverse effects, the researchers found that differences in postinjection pain between 4% articaine, 1:100,000 epinephrine and 2% lidocaine, 1:100,000 epinephrine were small, with lidocaine probably resulting in slightly less pain than articaine. However, meta-analyses for other anesthetic comparisons of local and systemic adverse effects were not possible, they noted. Other adverse effects were rare and minor, they wrote.
Bias risks
The authors noted that most of the studies had a low risk of bias, but at least 15 of the 68 studies had a high risk of bias.
In addition, some studies fell short in terms of quality, owing to small numbers of participants, unclear reporting of study methods, and reporting of data in a format that was not easy to combine with other data.
Further studies are needed to increase the strength of the evidence, the authors concluded.
"These studies should be clearly reported, have low risk of bias with adequate sample size, and provide data in a format that will allow meta-analysis," they wrote.