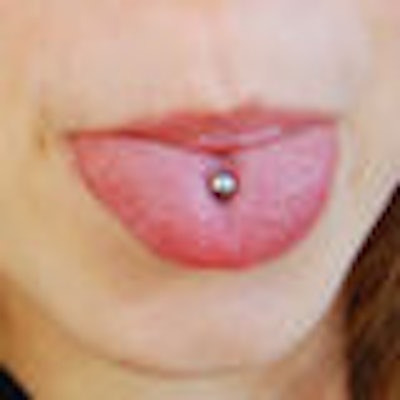
Being a teen's dentist is not easy. You are already battling problem trends such as crystal meth, smoking, questionable eating habits, and even diabetes.
Now a new study has pushed an old enemy to the forefront: oral piercings.
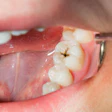
Researchers at the recent International Association for Dental Research (IADR) session in Toronto reported that the most common complications related to oral piercings are chipped, fractured, or cracked teeth and gingival recession. Less common but life-threatening complications include Ludwig's angina, Lemierre's syndrome, and hemorrhage.
“Health professionals should be aware and knowledgeable of these risks in order to provide their patients appropriate advice.”
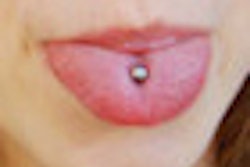
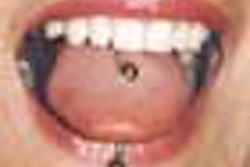
The researchers noted that oral piercings are most popular among younger patients between the ages of 18 and 30, and the tongue and lip are the most common piercing sites. They conducted a systemic review of research on the adverse effects of oral piercings over the last 12 years.
"Piercers are usually unlicensed and untrained," the authors noted. "Health professionals should be aware and knowledgeable of these risks in order to provide their patients appropriate advice."
A previous study looked at research published between 1992 and 2007 and found that 10% of all New York teenagers have some kind of oral piercings, compared to about 20% in Israel and 3.4% in Finland (American Journal of Dentistry, December 2007, Vol. 20, pp. 340-344).
The authors reviewed articles on complications from oral piercings. From the reviewed literature, the lowest recorded rate of swelling and infection after a piercing by a study was 24%, while the highest rate noted was 98%. Pain or tenderness ranged between 14% and 71%, while speech interference came in at 14% to 51%. Numbness, eating difficulties, and bleeding were common short-term postoperation side effects as well.
Jewelry-induced complications included tooth fracture (13% to 41%), gingival recession (19% to 68%), and ingestion of jewelry (7% to 34%). Other side effects included taste interference and halitosis.
"There are short-term complications to piercings in low percentages of teens, and in rare cases a piercing to the oral cavity can cause death," stated Liran Levin, D.M.D., a clinical instructor at the Maurice and Gabriela Goldschleger School of Dental Medicine at Tel-Aviv University and an author of the 2007 study, in a recent press release. "Swelling and inflammation of the area can cause edema, which disturbs the respiratory tract."
"There is a repeated trauma to the area of the gum," he added. "You can see these young men and women playing with the piercing on their tongue or lip. This act prolongs the trauma to the mouth and in many cases is a precursor to anterior tooth loss."
Dan Peterson, D.D.S., who practices in Gering, NE, has had several teen patients come in with swelling and infection because of an oral piercing, and had to talk them into taking the piercing out and letting the area heal.
"I tell my patients that, even if they do not have any immediate infection, there will be some piercing-related complications in the future, so overall it's just a bad idea," Dr. Peterson said. "There are too many things that can go wrong."
With lip piercings, the jewelry constantly rubs against the gum tissue, which causes erosion over the long run, he said. In addition, biting down hard on a tongue piercing can chip teeth. People with tongue piercings are also subject to infections, and a severe tongue infection can cause breathing problems.
The piercing community does not deny these risks.
"There are always risks attached to oral piercings," said James Weber, president of the Association of Professional Piercers (APP). "We try not to downplay them."
Chipped teeth, gum recession, and swelling are potential side effects of piercing, he said. But appropriate placement and the right kind of jewelry can lower those risks significantly, he added.
"Right now, most piercing salons have to abide by very few regulations, if any, and that is why the clients need to take responsibility," Weber said.
The APP urges people to go to a piercer who is skilled, experienced, and uses sterile instruments, jewelry, and disposable needles. Clear aftercare instructions should also be provided. According to the APP, if a piercer tells their clients to treat a piercing with harsh soap, ointment, alcohol, or hydrogen peroxide, the studio is not keeping up with industry standards. The APP recommends sea salt and a mild liquid soap. (For more details on ensuring safer piercings, you can direct your patients to the APP Web site, which has information on choosing a piercer and oral piercing risks and safety measures.)
ADA consumer advisor Matthew Messina, D.D.S., who practices in Cleveland, has done fillings and crowns on chipped teeth and dealt with several infections -- all related to piercings.
An oral piercing is an open wound, he pointed out. Unlike an ear piercing, if you remove the jewelry from an oral piercing, the hole closes because it is moist tissue.
An antibacterial rinse should be a mandatory part of the daily routine for anyone with a tongue piercing, as should cleaning the piercing bar regularly to avoid tartar buildup, Dr. Messina said. He also recommended having patients seek immediate medical help if there is any redness, swelling, or pain around the piercing.
In the long run, however, the dental community's advice: Don't do it!
"Teenagers are not easy to manage," Dr. Levin noted. But "try where possible to dissuade your teen from getting a piercing," he said. "They will thank you when they are older."