Periodontitis and rheumatoid arthritis (RA) are both chronic inflammatory diseases and share other similarities. But is there a causative relationship? A new study examines the evidence.
The study reviews the clinical and experimental findings supporting the connections and potential mechanisms between periodontitis and rheumatoid arthritis. Despite differences in etiology, the conditions are similar in terms of pathogenesis, according to the authors.
"The body of evidence built up over the past decade leaves little doubt that periodontitis and RA are intimately linked, and that these links are not just due to similarities in pathogenic mechanisms and shared environmental and genetic risk factors," the authors wrote (Nature Reviews Rheumatology, August 24, 2017).
The lead author was Jan Potempa, PhD, DSc, a professor in the oral immunology and infectious diseases department at the University of Louisville School of Dentistry in Kentucky.
Making the periodontal pathogenesis case
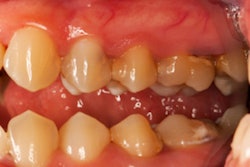
Periodontitis is arguably the most prevalent bacteria-driven chronic inflammatory disease on earth, with 46% of U.S. adults having some form of it and 11% of adults worldwide having the most severe forms. Rheumatoid arthritis is a systemic autoimmune disease that causes chronic, painful joint inflammation, as well as disability and increased mortality. Its prevalence in the U.S. is around 0.6%. However, it is only in recent years that growing evidence suggests a strong link between periodontitis and systemic diseases, the authors noted.
Studies have shown that periodontitis is more prevalent in patients with active rheumatoid arthritis than in healthy individuals, while rheumatoid arthritis is more prevalent among those with periodontitis than those without it.
“The body of evidence built up over the past decade leaves little doubt that periodontitis and rheumatoid arthritis are intimately linked.”
The two conditions share various attributes:
- They are both diseases that can have a variety of different causes, and both involve localized chronic inflammatory reactions spurred by similar cytokines.
- Connective tissue breakdown occurs in both diseases.
- Bone erosion is often seen.
- The diseases share environmental and genetic risk factors, such as expression of the gene HLA-DRB1, smoking, aging, nutrition, socioeconomic status, and psychological factors (such as stress).
Alvin Danenberg, DDS, a periodontist based in South Carolina, emphasized the connections between periodontal disease and the health of the rest of the body. Dr. Danenberg was not connected with the study.
"Porphyromonas gingivalis, which is a virulent bacterium in active periodontitis, creates an enzyme, P. gingivalis, peptidylarginine deiminase, known as PPAD, that eventually is involved with a specific antibody that almost always leads to rheumatoid arthritis," Dr. Danenberg told DrBicuspid.com. "It is important to make sure active periodontal disease is diagnosed properly and treated effectively because of this close association."
Bringing it back to the dental chair
So how can knowledge about the links between periodontitis and rheumatoid arthritis best be used by dentists to care for their patients? Active disease in one part of the body can affect other parts of it, noted Dr. Danenberg, adding that treating any sources of infection and chronic inflammation is important for the entire body to be healthy.
 Alvin Danenberg, DDS.
Alvin Danenberg, DDS."When there is an acute infection like periodontitis, it must be treated first," he stated. "That would include efficient scaling and root planing, which must be done thoroughly with the tissues being numbed. Medication may be required, depending on the severity of the infection."
A patient diagnosed with rheumatoid arthritis by a medical doctor should undergo a comprehensive examination for any gum disease, Dr. Danenberg noted. He also recommended that all individuals perform proper brushing and interdental cleaning with a device and avoid the daily use of antimicrobial mouthwash, since it can kill necessary healthy bacteria.
Dentists should also be aware that other factors besides P. gingivalis can lead to the development of rheumatoid arthritis without active periodontitis, according to Dr. Danenberg.
"Specifically, pathogenic immune reactions in the lungs from cigarette smoking or in the gut from unhealthy changes in the microbiome could lead to conditions that can precede the clinical manifestation of RA by many years," he stated.
At the same time, the study authors noted that more research is needed on the connection between periodontitis and rheumatoid arthritis.
"Further well-designed mechanistic and epidemiological studies into the links between periodontitis and RA are needed to elucidate the mechanisms involved," they concluded.