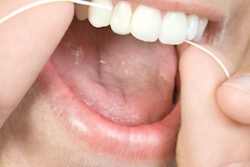
How does flossing compare with other interdental oral hygiene aids for maintaining periodontal health? Could the longstanding dominance of floss be heading for a further tumble? Researchers analyzed the existing evidence in a new study and reached some interesting conclusions.
U.S. researchers conducted a meta-analysis of randomized clinical trials on the effects of various interdental oral hygiene aids on gingival inflammation and bleeding on probing, as well as plaque and probing depth. They found good results for interdental brushes and water jets, with floss and toothpicks bringing up the rear (Journal of Periodontology, February 19, 2018).
"Interdental oral hygiene aids are important supplements to toothbrushing and should be recommended," lead study author Georgios Kotsakis, DDS, told DrBicuspid.com in an email interview. "All are effective to a certain extent. If one oral hygiene aid does not work for the person in our chair, we should explore other alternatives."
Dr. Kotsakis is an assistant professor of periodontics at the University of Washington School of Dentistry in Seattle. The study co-authors were from the University of Minnesota in Minneapolis and the University of Texas Health Science Center at Houston.
Inflammation minimization
The availability of multiple oral care products can be confusing for consumers, as well as dentists, Dr. Kotsakis noted. Additionally, available data on the effectiveness of various interdental cleaning devices are limited. The situation has been further complicated by a 2015 European Federation of Periodontology workshop consensus that concluded that floss should only be recommended for sites with gingival and periodontal health in which interdental brushes don't fit, according to the authors of the current study.
“If one oral hygiene aid does not work for the person in our chair, we should explore other alternatives.”
"Until recently, the use of floss was considered the gold standard, but nascent scientific information challenged the notion that everyone can floss effectively," Dr. Kotsakis told DrBicuspid.com.
Many studies on interdental tooth cleaning are sponsored by industry or compare only a single intervention to toothbrushing alone. Meta-analysis can be helpful when comparing two interventions but can be limited in effectiveness beyond that, the authors wrote.
To assess multiple interventions, the researchers used the statistical technique of Bayesian network meta-analysis to determine the relative efficacy of various interdental oral hygiene aids at reducing plaque and gingivitis.
They required that included studies be randomized clinical trials with at least 10 patients in each study group and at least two weeks of follow-up that included the following additional attributes:
- Assessment of interproximal oral hygiene methods performed by physically competent people
- Report of outcomes measuring gingival inflammation, plaque, or probing depth
Ultimately, the study included 22 clinical trials, with their results published in journals from 1980 through April 2015. Nine (40.9%) were industry-funded, and the remaining ones did not provide funding information. The researchers judged four studies to have a low risk of bias, one to have a high risk, and the remaining to have an unclear risk.
The number of participants per study arm ranged up to 110. The researchers grouped the included interventions into the following categories:
- Toothbrush only (control)
- Flossing
- Powered flossing
- Toothpicks
- Toothpicks and intensive oral hygiene instructions
- Water jet irrigation devices
- Interdental brushes
- Gum massaging devices
- Powered, electric, and sonic toothbrush (powered control)
- Power control and water jet
Toothpicks with oral hygiene instruction had the greatest reduction in bleeding on probing (26.4%) compared with toothbrushing alone, followed by the water jet (19.3%). Both were the most likely to be categorized as the best for reducing bleeding on probing. Additionally, floss and automated floss were significantly more effective than toothbrushing alone at reducing bleeding on probing, although the effect size was relatively small.
The greatest reduction in gingival inflammation as measured by gingival index reduction was achieved with interdental brushes, followed by water jet irrigation devices -- both of which were also most likely to be categorized as the best methods for reducing the gingival index. Unsupervised flossing, however, did not lead to substantial lessening of gingival inflammation.
Interdental brushes were more effective than most alternative oral hygiene aids for plaque index reduction, with a mean effect of 0.34 reduction in gingival inflammation compared with the control of toothbrushing only and ranking first for probing depth reduction.
Interdental brushes and water jet irrigation systems consistently ranked high among interventions, while the use of a toothpick combined with intensive oral hygiene instruction was more likely to rank first for reducing bleeding on probing, the authors reported.
"It appeared that all interdental oral hygiene aids, with the exception of toothpicks, were better than toothbrushing alone in reducing gingivitis between the teeth," Dr. Kotsakis told DrBicuspid.com. "[Interdental brushes and water jets] are more straightforward for home care, which points to the fact that ease of use may be an important factor in selection of oral hygiene aids."
The findings are in agreement with the European Federation of Periodontology workshop consensus, the authors noted. The current study results indicate that flossing may be efficacious, but its effective use can be elusive.
"Our results support that dental floss is not the quintessential interdental oral hygiene method," wrote the authors, adding, however, that "persons that are effectively using floss should not be instructed to discontinue their oral hygiene habits."
Not the last word
The authors noted the following limitations of their study:
- Many of the included studies lacked information on participants' periodontal status.
- Available statistical models had limitations to reach more definitive conclusions.
- The study did not include relevant safety outcomes, such as gingival trauma.
- A small number of studies involving certain interventions were included.
- There was heterogeneity in the sample populations and methods of interdental oral hygiene instruction.
They added that the use of patient-oriented concepts such as oral health-related quality of life instead of measures like gingival inflammation would allow for a more comprehensive measurement of the total effect of an intervention.
However, their study findings showed that unsupervised flossing does not result in substantial reduction in gingival inflammation, the authors concluded.
"This study has far-reaching implications as it provides the highest level of evidence in regard to the recent flossing debate," Dr. Kotsakis noted.