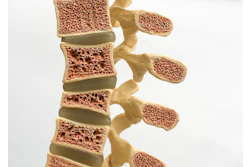
Oral bacteria linked to gum disease that migrates to the gut may be linked to bone loss and the development of osteoporosis, especially among postmenopausal women, according to a press release dated March 4.
A better understanding of how oral bacteria affect gut metabolism may help pioneer treatments that improve older patients’ quality of life, according to the release from the Sichuan University School of Stomatology in China.
“We were motivated by the clinical reality that many patients suffer simultaneously from periodontal disease and osteoporosis, yet treatment strategies rarely consider their biological connection,” Dr. Fuhua Yan, a professor at the Nanjing University Institute of Stomatology in China, said in the release.
Researchers analyzed salivary microbiota from individuals with advanced periodontitis and compared them with samples from periodontally healthy donors. The microbiota was then administered to ovariectomized mice, which are commonly used as models for postmenopausal osteoporosis.
The study’s design allowed the researchers to evaluate the effects of oral microbial communities without the influence of inflammatory factors. Imaging and histological analyses showed that mice receiving microbiota from patients with periodontitis had significantly lower bone mineral densities and poorer trabecular bone structure than control mice.
Additionally, these skeletal changes were linked to a noticeable increase in osteoclasts, the cells responsible for bone resorption. Further analysis suggested that the bone loss was driven by changes in the gut. Although periodontal pathogens did not strongly colonize the intestine, the salivary microbiota altered the overall gut microbial environment.
Metabolomic testing showed suppressed tryptophan metabolism, highlighting microbial metabolites as important signals in the oral-gut-bone connection. Among these metabolites, indole-3-lactic acid (ILA) appeared protective, as reduced levels were linked to increased osteoclast activity and bone loss, while oral ILA treatment restored bone density and improved bone structure in the affected mice.
In the future, the researchers aim to change how chronic inflammation-related systemic diseases are prevented and treated, encouraging greater collaboration among dentistry, microbiology, and metabolomics.
“This study shows that oral health cannot be viewed in isolation from systemic physiology,” Yan said.