Using a 3D dental replica when planning tooth autotransplantation offers benefits, including shorter surgical times and less trauma to the periodontal ligament, according to a communication published on December 8 in the Journal of Stomatology, Oral and Maxillofacial Surgery.
When a tooth can't be saved and an appropriate 3D replica is available, autotransplantation should be the first treatment choice for clinicians, the authors wrote. It should also be the default treatment when a replacement tooth has incomplete root development.
"Digital planning and using 3D replicas make democratizing this type of procedure possible with respect to invasive surgery, such as pre-implant and implant surgeries on agenesia or nonconservable teeth," wrote the authors, led by Cyril Debortoli, a resident at the University Hospital of Nice in France.
For many years, autotransplantation has been used in oral surgery to transplant mature or nonmature teeth into a site where no tooth existed or the tooth could not be restored. Ideally, this technique is used for a tooth with an open apex that remains under development. For the technique to be successful, the periodontal ligament must be preserved to prevent postsurgical complications, including root resorption, and to allow orthodontic movement.
Since innovations in digital technology, specifically surgical planning, have allowed for biocompatible and sterile dental replicas to be used during surgery, the authors aimed to introduce autotransplantation using a 3D dental replica.
Steps to creating a 3D replica
The authors followed the following four steps to create and place a 3D replica:
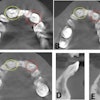
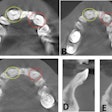
- Data was extracted from the patient's cone-beam computed tomography (CBCT) scan, and the dimensions of teeth and the space created by the orthodontist in three dimensions were measured.
- The CBCT scan was used to isolate the impacted teeth and the stereolithography files were sent to a 3D printer.
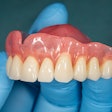
- Dental replicas were printed on a workable resin.
- A passive preformed orthodontic wire was provided postoperatively to exert the fewest constraints on the transplanted teeth and was placed in an underbite to avoid static and stress.
When it was time for surgery, the patient was placed under general anesthesia. Local infiltration was performed with 0.9% sodium chloride adrenaline 1-to-200,000.
An intrasulcular incision was made from 44 to 34, with two vertical discharge incisions to provide laxity to the flap. The detachment revealed cortical effraction in front of 33. Implant material was used to prepare the sockets, and spiral drills that would accept the replica without stress were used, according to the note.
Once the sockets were recreated, the impacted canines were extracted without iatrogenic movement to preserve the pericoronary sac. To avoid damaging the alveolar ligament cells, teeth should be handled by the crown and not the root. The teeth were placed in their respective places, and pericoronary sacs were sutured to the gum, the authors wrote.
An orthodontist must create a passive arch support with a rectangular steel wire that a patient must wear for three weeks. Furthermore, preserving the pericoronary sac increased the sealing, which prevented bacteria from entering and allowed the gum to heal, the authors wrote.
About six months after the procedure, imaging showed no resorption, abscesses, mobility, or infections. Therefore, using 3D dental replicas offer a dependable, reproducible, and valid treatment with a favorable benefit-risk balance, they wrote.
"Autotransplantation should be the first-line treatment option when criteria for surgical indications are fulfilled," Debortoli wrote.