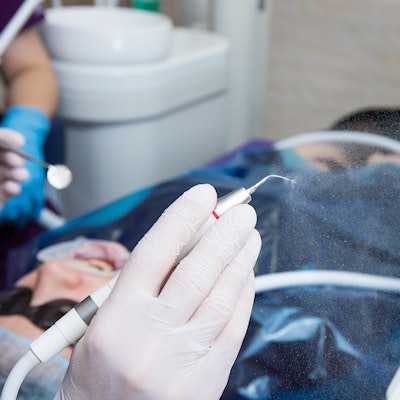
Dental hygienists should consider multiple factors, including positive COVID-19 cases in their communities, before using ultrasonic scalers on patients, according to a webinar hosted by the American Dental Hygienists' Association (ADHA) and the ADA on May 4.
Though the U.S. Centers for Disease Control and Prevention recommends avoiding the use of scalers during the pandemic, hygienists must weigh the benefits and risks of using them, said JoAnn Gurenlian, RDH, PhD, the chair of the ADHA's Return to Work Taskforce.
"Look at all factors to make the clinical decision," Gurenlian said.
Hygienists should consider the number of COVID-19 positive cases and vaccination rates in the areas where they work, consider how aerosols are reduced at their workplaces, and seek recommendations from local health departments, according to Gurenlian. Also, hygienists should keep up with research about the risks of using ultrasonic scalers, she added.
"Some evidence shows hand scaling is more effective than a Cavitron," Gurenlian said. "What risks will you take over the benefit?"
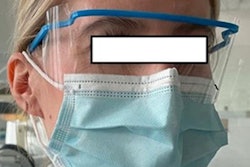
One benefit of not using a scaler is that hygienists do not need to wear N95 respirators, which are only required during aerosol-generating procedures, Gurenlian noted. Gurenlian also disputed the idea that adding chlorhexidine to a scaler makes it safer, saying there was no evidence to support this practice.
"I'm not sure it's a good practice," Gurenlian said. "We don't know if it causes damage to the water lines."
Post-pandemic in the dental office
In the webinar, Gurenlian also explored the idea of what the future dental practice will look like as the world transitions from pandemic to post-pandemic. One question she asked is whether proof of a negative COVID-19 test should be required for dental patients.
"It's not recommended by any national organization at this time," Gurenlian said. "I don't know at this point if we have to go to that extreme. We'll have to see where we go from here."
However, it is appropriate to ask patients if they have been vaccinated for COVID-19. Asking about vaccinations, including measles, mumps, and COVID-19, should be part of taking routine patient medical histories, she said.
Gurenlian warned that it is important to remember that patients are not always forthright with vaccine information. Therefore, patient mask wearing in office settings should remain a requirement even at practices with fully vaccinated teams.
"Some patients will say they are fully vaccinated but were vaccinated three days ago," she said. "You don't know what they're bringing to you and what they're exposed to. A little extra caution right now is a good idea."
Furthermore, it is crucial to continue patient screenings prior to dental visits, noted Ann Battrell, MSDH, the ADHA CEO.
"Cases in oral health professionals are low due to screening procedures," she said. "Asking patients if they are fully vaccinated is an important part of keeping a safe environment."
Additionally, dental practices should not stop taking patients' temperatures. An elevated temperature is an indicator of infection and a low temperature could be a sign of another problem. In fact, dental teams should be taking and recording all patient vital signs, including blood pressure, pulse, height, weight, and respiration, Gurenlian said.
"We are healthcare providers, and we should be doing all vital signs in all practices," she said.
"We should evaluate systemic health on all vital signs."
Eventually, the Occupational Safety and Health Administration (OSHA) may change guidelines related to aerosol-generating procedures, like the organization did for bloodborne pathogens during the AIDS epidemic, Gurenlian said. In 1991, OSHA instituted a standard for bloodborne pathogens aimed at protecting workers, including dental professionals, from the risk of exposure to HIV and hepatitis B.
"Things will change over time," she said. "We're learning one thing. This virus is unlike any other. The best we can do is give infectious disease specialists a chance to learn and be part of the process."