The role dentists and hygienists can play in helping patients reduce their risk of cardiovascular disease (CVD) is highlighted in a new literature review that further links periodontitis and the risk of heart disease, stroke, congestive heart failure, and peripheral artery disease.
The authors of the new report in Trends in Endocrinology and Metabolism (April 16, 2015) cited previous studies that show "excess risk" for CVD in patients with periodontitis. As almost half of the U.S. population has generalized periodontitis and up to 90% has a milder form, the public health implications of untreated periodontal disease are clear, they wrote.
“Periodontitis is not just a dental disease, and it should not be ignored, as it is a modifiable risk factor.”
"The majority of diseases and conditions of aging, including obesity and type 2 diabetes, have a major inflammatory component that can be made worse by the presence of periodontitis," stated senior author Thomas E. Van Dyke, DDS, PhD, chair of the department of applied oral health sciences at the Forsyth Institute, in a press release. "Periodontitis is not just a dental disease, and it should not be ignored, as it is a modifiable risk factor."
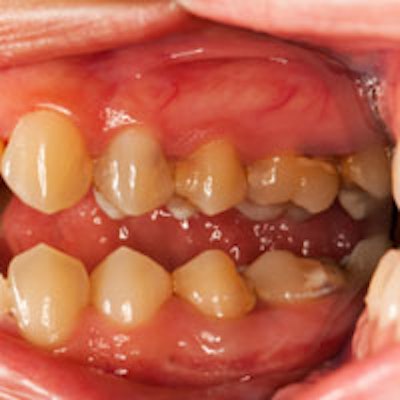
The report defines generalized periodontitis as involving more than a third of a patient's dentition. Cardiovascular disease is a chronic condition that can lead to coronary heart disease, stroke, congestive heart failure, peripheral artery disease, and more.
Periodontal diseases are multifactorial chronic inflammatory diseases, characterized by progressive destruction of the supporting structures of multiple teeth. The process begins as gingivitis, caused by a "resident biofilm" (plaque) that forms on tooth surfaces at the gingival margin.
The current belief is that systemic exposure to oral bacteria triggers inflammatory processes in the cardiovascular system, which may lead to the initiation and progression of CVD, according to the authors. They cited numerous studies over the last 15 years that have shown that periodontal bacteria are present in atheromatous plaques.
While the rates of CVD have dropped over the last 30 years, the condition is still responsible for almost a third of deaths in the U.S., with three people dying every two minutes of atherosclerotic vascular disease, according to the review authors.
Potential treatments
How does bacteria travel from the mouth to the cardiovascular system? It has been estimated that ulcerated epithelium-lining periodontal pockets are usually between 8 cm2 and 20 cm2 in generalized periodontitis patients. The pockets provide a way for bacteria to enter into a patient's circulation. These pockets can also be heavily populated by phagocytic cells, which also transport bacteria to other parts of the body.
What can patients be told in terms of treatment? Patients need to participate in taking better care of their teeth, Van Dyke said. However, treatment isn't as simple as recommending inflammation reducers. Over-the-counter nonsteroidal anti-inflammatory drugs may have significant cardiovascular side effects, meaning alternative treatments should be considered, he noted.
One commonly prescribed cholesterol-lowering medication, atorvastatin, in high doses boosts blood levels of the anti-inflammatory molecules lipoxins and resolvin. This medication also prevents both periodontal and cardiovascular inflammation and reverses existing disease in humans without suppressing the immune system. Van Dyke noted that this potential treatment is "exciting and promising."
"New discoveries of natural pathways that resolve inflammation have offered many opportunities for revealing insights into disease pathogenesis and for developing new pharmacologic targets for the treatment of both oral infections and cardiovascular disease," Van Dyke said.