I have no gum disease.
I have superb nutrition and an extremely diverse gut microbiome. In fact, one of the core elements of my Balanced Metabolic Coaching program focuses on dental health.
So how come my latest periodontal exam showed signs of tooth decay? And why is it highly likely this decay is connected to my cancer battle?
Let me walk you through some of my history and thought process.
My diagnosis of root caries
 Dr. Alvin Danenberg.
Dr. Alvin Danenberg.My 25-hydroxyvitamin D blood level is 83 ng/mL, and I take 0.03 mg of vitamin K2 daily. The two-week standard deviation of my glucose variability is 10 (amazing!). And I cycle into and out of ketosis weekly.
The above factors suggest that I have a robust immune system. So my mouth should be in perfect shape.
But something happened.
I have an area of root decay on my lower right cuspid. Even though it is incipient, I am concerned that this could have happened to me.
Let me be candid and transparent, which I have been throughout my cancer journey. I will explore the following:
- How the decay was diagnosed
- How it could have happened
- What I'm going to do about it
- My experiment to remineralize active decay
Let's get into it.
How was the decay diagnosed?
I made an appointment with my buddy periodontist to examine my mouth on October 28, 2021. This was my first periodontal exam since being in hospice in August 2019.
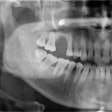
After his detailed evaluation, he determined my overall mouth health was excellent. But he noticed a small area of soft decay on the side of the root of my lower right cuspid (tooth #27) between the cuspid and lateral tooth. It was not significant on the x-ray, but he diagnosed it with a dental instrument.
What? How could that be? How could I develop tooth decay?
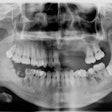
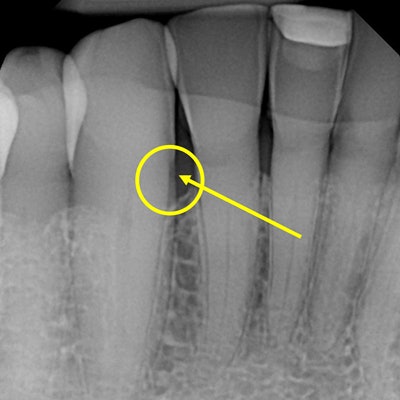
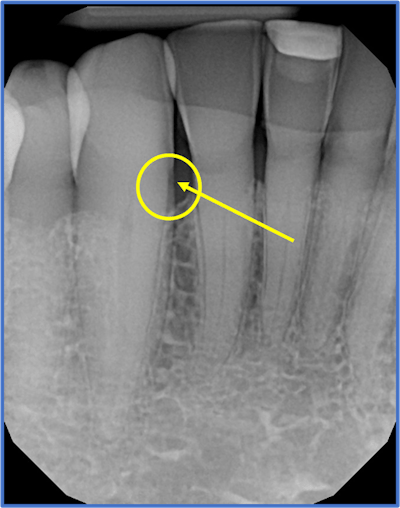 A dental x-ray showing root decay on the mesial of #27. Image courtesy of Dr. Alvin Danenberg.
A dental x-ray showing root decay on the mesial of #27. Image courtesy of Dr. Alvin Danenberg.How could that happen?
When I fell in my bathroom in August 2019, I split my right femur and right humerus in half and broke a couple of ribs. That was my worst setback. I could not imagine that my body and quality of life could recover from so much damage.
In hospice, I was bedridden, catheterized, demoralized, depressed, and constipated. I was unable to clean my mouth for over a month. The best I could do was try to brush and use TePe EasyPicks until my right humerus began healing and my right hand could function.
But I did eventually recover, revoke hospice, and reintroduce my unconventional cancer protocols. I amazed all my doctors! By the middle of October 2019, I returned to my oncologist and was on the mend. He couldn't believe I was still alive!
However, the weeks in hospice -- and then several more weeks of recovery -- came with various infections, mouth issues, and antibiotics. While on narcotics and many drugs during hospice, my gut microbiome was severely compromised. The catheterization caused me to develop two urinary tract infections that required antibiotics. As a result of antibiotics and other meds, I also had several bouts of yeast infection in my mouth, which needed to be treated.
Once I was able to start flossing and cleaning my mouth correctly, I mistakenly believed all was OK. There were no signs or symptoms of any residual damage in my mouth -- no pain, bleeding, swelling, or problems eating or speaking.
So, I went on my merry way. Then, a couple of weeks ago, I decided to have my mouth checked out since it was more than two years since my last dental exam. I know! How stupid was it to procrastinate until now?
On October 28, 2021, I scheduled my first periodontal exam in a long time. Thinking I was in great shape, I looked forward to an excellent report.
Surprise! I didn't get it. I was diagnosed with isolated early root decay.
This should be a "heads up" warning for all of us. You don't know what you don't know!
What am I going to do about it?
My isolated decay appears to be very early stage. One option would be to place a composite restoration to repair the decay. That would involve some mechanical trauma to the tooth to place the filling. It also could cause possible nerve damage to the pulp of the tooth depending on the depth of the existing decay and further preparation of the tooth for the filling. In addition, I would prefer to avoid a chemical in my mouth, if possible.
A better option would be to attempt to remineralize the area of decay naturally. Because the decay is very early, remineralization should be easy and predictable.
There are several peer-reviewed medical papers discussing the benefits of microhydroxyapatite particles remineralizing active decay. There also are a few published dental clinical trials showing that manuka honey will decrease the pathological activity of decay-forming bacteria (e.g., Streptococcus mutans) as well as decrease the pathological potential of various periodontal pathogens (e.g., Porphyromonas gingivalis).
Since my entire cancer journey has been an experiment with only me as the subject (N = 1), I am going to try to remineralize this early but active decay. I'll document the existing decay with a current x-ray and then follow up with necessary dental appointments.
My personal experiment to remineralize active decay
On November 2, 2021, I had a full-mouth series of dental x-rays confirming root decay on the mesial of #27 and evaluating other areas in my mouth. My dentist mechanically removed the soft decay in the area and placed ozone to kill the bugs.
Immediately, I began using a TePe EasyPick first dipped in manuka honey and then dipped in Shine powder (a microhydroxyapatite powder marketed by OraWellness). I gently rub them onto the surface of the decayed root three to four times per day.
I will let the Shine powder stay on the surface of the root decay without rinsing it out of my mouth. It contains microcrystalline hydroxyapatite from powdered bone of grass-fed New Zealand cattle, as well as sodium bicarbonate, birch xylitol, white kaolin clay, calcium lactate, magnesium carbonate, Himalayan salt, and cinnamon oil. I am not a fan of xylitol used daily because it prevents healthy dental plaque from forming, but I am using this as an isolated therapy for active root decay.
Every couple of months, I'll have my dentist check the area to evaluate remineralization. If I am unsuccessful, I will have a composite restoration to fix the decay.
I am hopeful that my experiment will work. It might also work for others who have early tooth decay. But many other factors must be in place to create remineralization: a nutrient-rich way of eating, a diverse gut microbiome, a healthy gut lining, and a daily mouth cleaning regimen. I have all of those bases well covered.
Dr. Alvin Danenberg has retired from the private practice of periodontics in Bluffton, SC. He continues to be on the faculty of the College of Integrative Medicine and created its integrative periodontal teaching module. He also spent two years as chief of periodontics at Charleston Air Force Base earlier in his career. His website is drdanenberg.com.
The comments and observations expressed herein do not necessarily reflect the opinions of DrBicuspid.com, nor should they be construed as an endorsement or admonishment of any particular idea, vendor, or organization.