A new device by Norwegian researchers can help rebuild the faces of patients who have been disfigured by mandibular cancer and help patients with loose teeth caused by periodontitis. The process uses artificial bone scaffolding that determines where new bone tissue will grow.
After surgery to treat mandibular cancer, patients are often left with disfigured faces. Mandibular bone can also be damaged by cancer, infections, and accidents.
Now a new invention, called NuBone, by researchers at the University of Oslo Faculty of Dentistry helps the body generate new bone as strong as the original, according to the school. Using this method, dentists can insert artificial, foam-rubber-shaped scaffolding that determines where new bone tissue will grow, helping the body repair the damage itself.
The device can also help patients with periodontitis, which can cause the bone adjacent to teeth to break down, loosening teeth.
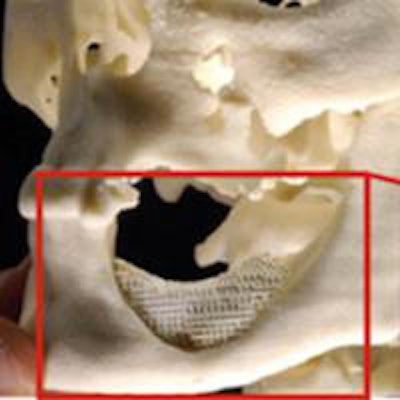
 If the mandible is damaged by cancer, an infection, or an accident, it may be a long time before the bone cells start growing into the scaffolding. The pace can be accelerated by adding the patient's own bone progenitor cells. Image courtesy of the University of Oslo.
If the mandible is damaged by cancer, an infection, or an accident, it may be a long time before the bone cells start growing into the scaffolding. The pace can be accelerated by adding the patient's own bone progenitor cells. Image courtesy of the University of Oslo.
Bone fractures and repair
To understand this new method, the researchers explained how bone can repair itself. After a fracture, the bone fragments can knit together only if they are in very close contact, they noted.
When a bone fractures, blood collects at the site, and blood contains organic molecules that coalesce into long strands. This coagulum is then populated with cells and turns into connective tissue that later calcify. The connective tissue functions as a porous growth platform for bone cells and blood vessels. The bone cells remodel the calcified structure and form functional bone, while new blood vessels help bring nutrients and oxygen.
The outer part of the bone is compact, while the inner part is porous. The porous part contains marrow cells, which are essential for maintaining the skeleton. Its porosity varies according to the type of bone.
“The artificial scaffolding is as strong as real bone and yet porous enough for bone tissue and blood vessels to grow into it and work as a reinforcement for the new bone.”
Artificial help for bones
If the gap is too wide between the bone fragments, or if parts of the bone have been damaged, the body cannot always repair the damage by itself, as happens when some of the bone has been removed during cancer surgery or when the bone has been damaged by radiotherapy.
"With our new method, it's sufficient to insert a small piece of synthetic, bone-stimulating material into the bone," said Ståle Petter Lyngstadaas, DDS, PhD, the research dean at the Institute of Biomaterials at the Faculty of Dentistry. "The artificial scaffolding is as strong as real bone and yet porous enough for bone tissue and blood vessels to grow into it and work as a reinforcement for the new bone."
Dr. Lyngstadaas and his colleagues, Håvard Jostein Haugen, PhD, and Jan Eirik Ellingsen, DDS, developed and patented the new technique.
Speeding with stem cells
"To speed things up, we can take bone progenitor cells or bone marrow that contain committed stem cells from the patients and insert them into the scaffolding," explained Dr. Lyngstadaas, noting that these materials can accelerate the healing process.
When bone needs to be built into defects where the distance between the bone fragments exceeds 1 cm, stem cells should be added to obtain a good result, but stem cells are normally not required to solve problems with loose teeth and periodontitis, Haugen said.
The bone cells are dependent on nutrients, good growth conditions, and a specific signal to differentiate into bone-forming cells.
It's important that the surrounding bone tissue is healthy and that there is ample blood supply to the surgical site, the researchers said.
Made from food additives
Manufacturing the material is simple: A mixture of water and ceramic powder is poured through ultrapure foam rubber designed to look like trabecular bone. The ceramic powder consists of medical-grade titanium dioxide monodisperse nanoparticles. Titanium dioxide has already gone through numerous toxicity tests and is a common additive to pharmaceuticals, the researchers noted.
The substance is also referred to as E-171 and is widely used to color candy, toothpaste, biscuits, baked goods, ice cream, and cheese. When the mixture has solidified, it is heated to a temperature that causes the foam rubber to dissolve into water vapor and carbon dioxide and the nanoparticles to ligate into one solid structure. The result is a mirror image of the foam rubber structure.
The structure is similar to that of the porous part of the bone, the researchers said.
The material can be manufactured like cinder blocks and cut to shapes that fit into the bone defect. The artificial bone scaffolding has an open porosity of 90%, containing mostly empty space that can be filled with new bone.
Ample empty space is important, the researchers said, because the cavities must be large enough to make space for bone cells and also blood vessels that can bring in nutrients and oxygen and remove waste products. One of the problems with current materials is that they do not provide space for both bone tissue and blood vessels, according to the researchers.
Different methods
Currently, damaged bone is repaired by removing tissue from healthy bones -- for example, from the lower jaw, shin, thigh, or hip, and implanting it in the damaged location. The surgery is uncomfortable and often leads to complications, the researchers noted.
When the patient's own bone tissue cannot be used, ground bone from other people can be used instead. In the U.S., ground bone from cadavers is often used. Unfortunately, this solution is neither sufficiently strong nor particularly porous. It also has the disadvantage of risking disease transfer, they said.
To avoid the risk of human disease transfer, in the European Union, ground and heat-treated bone from animals is used. To avoid disease, only animals from closed and controlled herds are used. And whatever the source of the natural bone is, after removal of organics and heat treatment, porosity is far below the optimum, and the material is too brittle and weak to add support to the regenerated bone, the researchers said.
"One of the advantages of the current methods is that the added bone is gradually devoured by the cells of the body," Dr. Lyngstadaas explained. "Our material, on the other hand, will never disappear, but always remain as an integral part of the repaired bone, working as reinforcement. This calls for higher safety requirements."
Ready for clinical studies
The researchers have tested the new method successfully on rabbits, pigs, and dogs. In 2014, they want to start clinical studies on patients with periodontitis and damage to their mandibular bones. To establish what method works best, it is advantageous to perform tests on patients with periodontitis in particular, the researchers said.
"The patients often suffer from bilateral periodontitis," Dr. Lyngstadaas said. "This permits us to compare results by testing the material on one side and have the control on the other within the same patient."
The researchers also hope that orthopedists will be interested in their new method. They are looking for a large industrial partner who can bring the product to market within a few years.
"Many millions of kroner are spent annually on implanting new bone tissue in mandibles in Norway," Dr. Lyngstadaas said, adding that millions of patients worldwide could benefit from the technique.
Dr. Lyngstadaas has co-developed the new material in cooperation with the company Corticalis, of which he presently is the acting CEO.