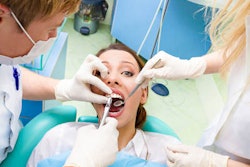
The administration of local anesthesia as a delegated dental hygiene duty was established in Washington state in 1971. In the 50 years since this precedent, all but four states have adopted this delegated duty into their state practice act. One of those states lagging behind is Georgia.
 Suzanne Newkirk, RDH.
Suzanne Newkirk, RDH.Although the state legislature granted the Georgia Board of Dentistry the authority to promulgate rules for the administration of local anesthesia by dental hygienists more than 30 years ago, the dental board only recently drafted the first proposed rule for dental hygienists who meet all educational and practice requirements. For the past 11 months, the dental board has been working to provide course requirements for practicing dental hygienists and for teaching dental hygiene students injection skills.
The proposed rule, a synopsis of which was published in the May 6 dental board minutes, authorizes dental hygienists working under the direct supervision of a Georgia licensed dentist to administer intraoral block and soft-tissue infiltration anesthesia to a nonsedated patient 12 years of age or older after all educational and practical experience requirements have been met.
The proposed change is a long time coming in Georgia, since dental hygienists are already required to be well-versed in anesthesia and pain management during training. Dental hygienists are required to take an eight-hour written National Board Dental Hygiene Examination, which assesses each candidate's ability to understand information related to dental hygiene, including the pharmacology, chemistry, and anatomy related to the administration of local anesthetic agents.
In addition, the ADA Commission on Dental Accreditation, which develops and implements the accreditation standards of all dental and dental hygiene programs in the U.S., mandates that all accredited dental hygiene programs include education on pain management in the core curriculum.
In the half-century since local anesthesia was established as a dental hygiene duty, states have even changed their requirements to reflect the safety of dental hygienists administering local anesthetic agents. As of 2022, approximately 50% of states no longer require an examination after dental hygienists have met their state course requirements, and nine states authorize the administration of local anesthesia by dental hygienists working without a dentist present in the treatment facility.
Despite the safe history of hygienists administering local anesthesia, not everyone is on board with Georgia dental hygienists joining the majority of the country in this practice. During the July 1 dental board meeting, representatives from the Georgia Dental Association (GDA) expressed concerns about dental hygienists administering block injections, but not because hygienists lack the skills.
Instead, the administration of local anesthesia by hygienists for a doctor's patients is "a production argument and reputational concern," according to one member of the GDA delegation.
Concerns about ... production?
The GDA stated their preliminary concerns had to do with issues they hear from patient complaints concerning overtreatment and aggressive treatment planning. According to the GDA delegation, local anesthesia given by a dental hygienist would put pressure on younger dentists to produce more money by doing more treatment.
When questioned by Dental Board President Dr. Glenn Maron, the GDA stated that dentists are currently limited to how many procedures they can perform, because they have to administer local anesthesia themselves and wait for it to take effect. If dentists can delegate the administration of local anesthesia to a hygienist, they can work on a patient in that time.
Extrapolating on this statement, the GDA's concerns are not about whether or not a dental hygienist is competent. The real issue is that younger dentists need to produce a certain amount of treatment to keep their spot.
As for the reputational concerns, although the proposed rule requires local anesthesia be provided under the direct supervision of a Georgia dentist, who is the sole decision-maker in the practice, the GDA stated that dentists do not always have the ability to oversee what dental hygienists are doing. The GDA gave an example of an elderly couple who were told they needed a deep cleaning and were charged a large sum of money -- only to be told by their past dentist that the deep cleaning wasn't needed.
What the GDA didn't say in the meeting is that the association not only supports but advocates for Georgia dentists to increase office production and efficiency via the delegation of services to their auxiliary personnel.
Under the expanded duties section of the education and training section of the GDA website, the association writes, "Like many dentists, you may be looking for ways to increase your practice's efficiency, production and revenue. Achieving those goals may be within reach when you enroll your assistants in the GDA Expanded Duties courses. According to an ADA survey, dentists who employ assistants with Expanded Duties in their practices report being able to use their time more efficiently and see more patients per day."
When considering the GDA's concerns regarding the delegation of services to dental hygiene auxiliary staff, one might suggest the GDA has its own reputational concerns to consider.
The real issue is ethics
The GDA statements are extremely disturbing on several levels. They suggest that Georgia dentists lack awareness of what procedures are being provided in their own practice. They infer the quality of care being provided under their supervision may be questionable due to "a potential high-pressure situation." And they insinuate Georgia's newly graduated dentists lack the ethical capabilities to plan treatments appropriately and will instead succumb to pressure to overtreat patients to maintain employment.
Considering the assertions made by the GDA and the board's decision to amend the proposed local anesthesia rule, the question that begs to be asked is do some Georgia dentists have a problem with ethics?
I hope not, as dental providers have an ethical duty to practice within the rules and regulations of their governing body. As such, before being granted licensure by the Georgia Board of Dentistry, both dentists and dental hygienists are required to take a jurisprudence exam on the laws and rules governing the practice of dentistry in the state.
Dental clinicians also have a moral obligation to maintain an honest relationship with society by rendering the best quality dental services to their patients. Both the ADA and the American Dental Hygienists' Association have codes of ethics that were established to provide guidance for their members to adhere to high ethical standards of conduct.
During the August 5 dental board meeting, the proposed rule was amended to restrict Georgia supervising dentists from having the authority to delegate this service to their dental hygienists for the doctor's patients.
This issue will be brought before the public for a final vote at the November 4 dental board meeting.
Suzanne Newkirk received her dental hygiene degree from the University of Alaska, Anchorage in 1981. A recognized key opinion leader in periodontal endoscopy, she has published numerous articles and co-authored several dental textbook chapters on minimally invasive nonsurgical periodontal therapy with use of the dental endoscope.
Newkirk is the national and international dental endoscopy instructor for Zest Dental Solutions and is a professional speaker. You can visit her website at www.perioscopyprofessionals.com. She can be contacted at [email protected].
The comments and observations expressed herein do not necessarily reflect the opinions of DrBicuspid.com, nor should they be construed as an endorsement or admonishment of any particular idea, vendor, or organization.