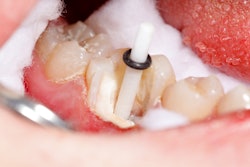
Did you perform crown lengthening (D4249) or crown exposure (D4212) on a tooth? Often, there is confusion about which of these procedures is correct when it comes to coding treatment, and mixing them up could cost you and your practice.
Insurance plan payers often deny coverage for crown lengthening because the clinical data submitted does not match the standard descriptor and nomenclature provided in the Code on Dental Procedures and Nomenclature (CDT) code manual. For proper claims submission and to eliminate the chance of denials, it is vital to understand the correct coding for procedures performed in your practice.
 Estela Vargas.
Estela Vargas.The coding of dental claims is far more complicated than a few years ago, and it continues to change every year. Below are some key differences for billing crown lengthening and crown exposure procedures. If your team needs help with coding and claims submission, consider outsourcing it to a professional billing company that accepts a commission and guarantees results.
Crown lengthening vs. crown exposure
D4249 (Clinical crown lengthening -- hard tissue) is hard tissue or bone removal, a surgical procedure. Crown lengthening is a restorative procedure performed on a tooth with little to no tooth structure exposed in the oral cavity. This procedure can provide both functional and aesthetic benefits to natural and restored teeth. Creating a healthy and stable foundation to support a new crown is the goal.
From a coding standpoint, trimming soft tissue to expose more tooth structure is not the definition of crown lengthening. Soft-tissue removal would most likely be billed as code D4212 (Gingivectomy or gingivoplasty to allow access for restorative procedure, per tooth). Most payers consider soft-tissue removal part of the crown preparation procedure and don't allow a separate payment.
D4249 is also only indicated when there is a healthy periodontal environment. If periodontal disease at the site of the crown lengthening is present, then D4249 may not be the correct code and D4261 (Osseous surgery ... one to three contiguous teeth or tooth-bounded spaces per quadrant) may be indicated.
Billing procedures and narratives for crown lengthening
For crown-lengthening procedures, the description in the clinical notes should expressly support and reflect raising of a full-thickness flap and removal of bone, altering the crown-to-root ratio. Clinical notes should also say crown lengthening was performed in a healthy periodontal environment, with no presence of periodontal disease.
Billing insurance plans for a crown-lengthening procedure at the exact service date of a crown prep will most certainly be denied. Most payers require at least a six-week healing period before a final impression can be made.
Before proceeding with any crown-lengthening procedure, a treatment plan should be written up and analyzed for the proper clinical course of treatment and follow-up care. Crown-lengthening claims must be supported by excellent narratives derived from detailed clinical notes and supporting evidence.
D4249 requires a detailed narrative, site periapical radiographs, and current periodontal charting to prove the periodontal health of the area. Photographs are beneficial if the tooth is fractured at or below the gum line before treatment, since fractures are often not visible on radiographs.
Clinical documentation from the treatment provider must show that bone was removed to create an adequate width between the apical margin of the restoration and the bones. A statement of a healing period of six weeks before the final impression should be provided as well. Depending on the payer, it may be necessary to give a final seat date for the crown.
The clinician must describe the decay and lost tooth structure, such as, for example, "ML cusp fractured off within 1 mm of crest bone, see M decay. See attached periodontal chart with the radiographic image."
Photos taken during treatment are essential to support the evidence and treatment choice. Mark the photographs showing the teeth and surfaces.
Billing for crown exposure
D4212 is a procedure to allow access to a tooth for a restorative procedure per tooth. It entails removing gingival tissue to provide access to the margins of a crown preparation site. The goal is to get a good impression and good margins so the crown fits properly and functions as a natural tooth.
Narratives should include periapical radiographs, photographs before and during the procedure, and periodontal charting. It is a good idea to allow for healing for this procedure also. Many dental payers don't pay for this service because it is considered inclusive of crown preparation.
Record the process step by step and how much time it took to complete the gingivectomy for the payer to see it should be considered as separate from inclusion of the crown. Removing excess tissue is not crucial to the claim. A scalpel, electrosurgery, and laser are used for this purpose.
Estela Vargas, CRDH, is the founder and CEO of Remote Sourcing, a dental insurance billing and revenue recovery service. She is a graduate of Miami Dade College's dental hygiene program. Vargas' extensive background in the clinical arena of dentistry is coupled with her experience as a practice administrator and business executive.
The comments and observations expressed herein do not necessarily reflect the opinions of DrBicuspid.com, nor should they be construed as an endorsement or admonishment of any particular idea, vendor, or organization.