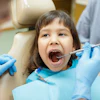
Older adults who skip needed dental care because of cost may significantly raise their risk of heart attack, stroke, or dementia. The large-scale study was published in The Journals of Gerontology, Series A.
It is the first study to tie financial barriers with the incidence of cardiovascular disease (CVD), the No. 1 cause of death, and dementia, the No. 6 cause of death, among those age 55 and older.
About 31 million U.S. adults age 55 and older lack dental insurance, with the cost of dental care out of reach for most. Medicare coverage for dental care is limited, and preventive services are often excluded.
“Cost is one of the main barriers to dental care. As a result, people often delay critical care,” said the study’s lead author, Mabeline Velez, MS, an instructor at the Boston University (BU) School of Public Health (BUSPH) and a doctoral student at BU’s Henry M. Goldman School of Dental Medicine, in a news release. “Finding ways to make dental care more accessible and affordable for everyone is a preventative measure that we can take to improve health outcomes down the line.”
The study sought to determine if older adults who declined dental care because of the financial costs later developed CVD or dementia. Velez and other researchers used data from the All of Us study, with a cohort of nearly 99,000 individuals. Participants responded to a questionnaire asking about their unmet dental care needs. They were then followed five years later via electronic health records to determine if they experienced a heart attack, heart failure, stroke, or dementia.
After adjusting for certain demographic factors, participants who reported forgoing needed dental care because of costs were 45% more likely to develop heart failure (hazard ratio [HR] = 1.45; 95% confidence interval [CI], 1.30 to 1.63), 37% more likely to have a myocardial infarction (HR = 1.37; 95% CI, 1.17 to1.61), 45% more likely to have a stroke (HR = 1.45; 95% CI, 1.24 to 1.70), and 37% more likely to later develop dementia (HR = 1.37; 95% CI, 1.05 to 1.76).
These associations changed slightly after adjusting for factors like socioeconomic status and behavioral and clinical factors, while there were no differences by gender, racial and ethnic identity, or a diagnosis of periodontitis. The researchers found that eliminating financial barriers could prevent 2% to 4% of each outcome, which could represent hundreds of thousands of cases across the U.S. older adult population.
Growing research has linked periodontal health with systemic conditions, including CVD, stroke, and dementia. It’s theorized that the bacteria causing periodontitis enter the bloodstream, triggering systemic inflammation.