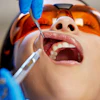
An intravenous sedative that induces a more natural, sleeplike experience with fewer side effects than other sedatives could find its way into dental offices in the near future.
A recent study in Anesthesia Progress concludes that intravenous dexmedetomidine (Dex), commonly used in intensive care units following surgery, is appropriate for use by anesthesia-trained professionals in certain dental applications (Fall 2008, Vol. 55:3 pp. 82-88).
"Dex induces a sedative response that exhibits properties similar to natural sleep, unlike other anesthetics," the study authors wrote. "Patients who are given Dex experience a clinically effective sedation yet are still easily and uniquely arousable -- an effect that has not been observed with any other clinically available sedative."
Sedation with Dex may be optimal for dental procedures, they contend, because it exhibits many of the properties of an ideal sedative agent: It takes effect quickly, sedative levels are easily manipulated, circulation and respiration are only minimally altered, and patients are easily brought to consciousness after the procedure.
But there are limitations. For example, while patients "wake up" more easily from their sleeplike state with Dex than with other sedatives, they also remain disoriented for a longer period of time after regaining consciousness than they do with other sedatives. In addition, using Dex (or any intravenous sedative) requires special training and licensing. General dentists more commonly use conscious oral sedatives such as nitrous oxide, Halcion (triazolam), or lorazepam for those patients with special needs or dental anxiety.
"Dex is an interesting drug, but there is a delay in onset and very long recovery period in the outpatient setting," said Steve Ganzberg, D.M.D., M.S., clinical professor of anesthesiology at Ohio State University and co-author of the Anesthesia Progress study. "There is less consistent amnesia than with benzodiazepine sedation, plus required IV administration. My opinion is that we have better drugs for the anxious patient population, so I would probably not recommend this agent at this time for the IV conscious sedation provider."
In the Dex study, 13 healthy volunteers were sedated with Dex at a loading dose of 6 mcg/kg/h for 5 minutes and a continuous infusion dose of 0.2 mcg/kg/h for 25 minutes. The recovery process was observed for 60 minutes postinfusion.
Results showed that low doses of Dex produced effective sedation, even though patients were easily awakened after dosing was discontinued. Patients responded to the sedative within 10 minutes of the start of the infusion and regained orientation within 15 minutes after its discontinuation, with full equilibrium restored in 60 minutes (as measured by standing on one leg with eyes closed).
According to the bispectral index, which measures sedative state, patients remained in a sedative state even when they appeared to be clearly conscious. Thus, discontinuing the Dex infusion approximately 15 minutes before the end of the procedure is recommended to minimize recovery time.
According to the researchers, it is important to note that patients in this study were relatively young and healthy. Higher doses and differences in age and health may thus affect the performance of Dex. Duration of the procedure is also a factor.
"Higher dosages need to be tested for their safety in certain patient populations," co-author Hiroyoshi Kawaai, D.D.S., Ph.D., department of dental anesthesiology at Ohu University School of Dentistry in Japan, stated in an e-mail interview with DrBicuspid.com. "It is okay to use Dex for longer procedures, but you should use sedation that finishes a procedure within two hours."
Dr. Kawaai and his colleagues use a combination of Dex, midazolam, and opioids for sedation during longer procedures.
"If you use Dex without combination drugs for procedures lasting more than two hours, it will take a lot of time for the patient to regain orientation," he noted. "We use midazolam and opioids such as butorphanol for sedation maintained with Dex infusion. If we perform sedation for a two-hour procedure, 0.05 mg/kg midazolam and 0.01 mg/kg butorphanol are given after the IV is given, and the sedation is maintained with a dose of Dex (0.2-0.7 mcg/kg/hr)." Advantages of this method include a sufficient amnesia effect -- lack of memory of the procedure or the injection -- and the patient being able to go home within three hours post-op, he added.
Dex may also have benefits for patients with heart disease or high blood pressure, according to the researchers. In the study, Dex produced a small but significant decrease in mean arterial blood pressure during the procedure, from 85 mm Hg to 77 mm Hg.
"Dex is an excellent sedative for poorly controlled hypertensive patients and those severely medically compromised patients for whom tachycardia and/or hypertension must be avoided at all costs," said Joel Weaver, D.D.S., Ph.D., president of the American Society of Dentist Anesthesiologists and editor of Anesthesia Progress. "However, the major use I might have for Dex is for patients who are obese and/or have obstructive sleep apnea, where traditional sedation might compromise the patency of the airway when they relax during dental treatment."
However, preliminary clinical research for this group of individuals needs to be conducted before recommending Dex for them, he added.