You know how to handle a frank cavity and what to do with a healthy tooth. But what about the many lesions that fall in between? A brace of new studies on resin infiltration suggests it can successfully treat lesions that are too small to restore but too big to ignore.
The evidence, including studies to be presented at next month's International Association for Dental Research (IADR) meeting in Barcelona, Spain, has reached the point that dentists should consider adding resin infiltration to their armamentarium, said Joel Berg, D.D.S., M.S., chair of the pediatric dentistry department at the University of Washington School of Dentistry. "These studies show the infiltration technique has the potential to stop lesions that might have progressed."
But he cautioned that practitioners must carefully select cases for the technique, and that questions remain.
How does it work?
Currently, only one resin infiltration product is on the market: Icon (DMG America). To use it, practitioners first open the pores of the lesion with hydrochloric acid. The low viscosity of the resins allows it to penetrate these pores by capillary action. Once hardened, the resin then protects lesions from both acid and nutrients that feed bacteria.
DMG recommends the product for two indications:
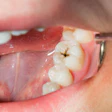
Proximal lesions to which applying a sealant would be difficult. Infiltration doesn't work well on occlusal surfaces because of the thickness of the enamel that must be stripped with acid.
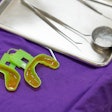
White spot lesions such as those left after treatment with orthodontic brackets. According to DMG, practitioners can achieve an almost immediate cosmetic effect because the acid removes some of the white enamel, and the resin changes the refraction index of the lesion.
“Most people find this valuable in young permanent teeth that you are really reluctant to cut.”
— Joel Berg, D.D.S., M.S.
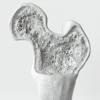
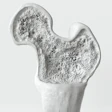
However, once infiltrated, the lesions cannot remineralize. While DMG recommends the product for lesions that extend up to D1 -- slightly into dentin -- Dr. Berg said he is most comfortable using the product in lesions that are up to the enamel-dentin junction but not beyond. "These lesions are too large to remineralize," he said, though he acknowledged there is debate among experts about just how deep a lesion can remineralize.
"Most people find this valuable in young permanent teeth that you are really reluctant to cut because there is a life span to a restoration," he said. "When you replace it, it's going to get larger."
Bitewing radiography is essential for determining exactly which lesions lend themselves to this approach, according to Dr. Berg, who has personally used Icon and spoken to many private dentists who are using it. "It's only as valuable as your ability to detect the depth of the lesion," he said.
Promising research
One study being presented at the IADR meeting compared three treatments for incipient proximal lesions: infiltration, sealing, and flossing with instruction. Researchers at Bosque University and the University of Copenhagen randomly assigned lesions in young adults to one of the three treatments.
The lesions were all around the enamel-dentin junction or in the outer-third dentin. Examiners assessed all the lesions radiographically and visually, using spacers. They used four criteria (plaque stagnation area, visual appearance, feeling, and papilla bleeding) to determine whether the lesions were active.
A year later, they used paired x-rays to determine which lesions had progressed. Of the active lesions available for follow-up, they found that five of the 26 in the infiltration group had progressed, compared to seven of the 27 in the sealant group and 13 of the 25 in the flossing group. (The group has not yet reported their calculations of statistical significance.)
But could such lesions have remineralized with a little help -- say, a fluoride varnish? In another study, the same team of researchers assigned two lesions in each of 40 Greenland children either to fluoride varnish or infiltration (Caries Research, March 2010, Vol. 44:1, pp. 41-46).
After a year, using the International Caries Detection and Assessment System (ICDAS), they found that 31% of the infiltrated lesions and 62% of the varnished lesions had progressed (p < 0.01). Radiographically assessing the lesions produced similar results.
Other studies -- most of them conducted by two of the product inventors, Hendrik Meyer-Lückel and Sebastian Paris of Christian-Albrechts University -- have achieved similar findings.
Remaining challenges
In one exception to be presented at the IADR meeting, researchers from Hacettepe University artificially created lesions in 64 extracted human molars and randomly divided them into groups treated with infiltration, topical fluoride gel, fissure sealant, or no treatment. They then subjected the teeth to pH cycling to mimic conditions in the human mouth.
The researchers subsequently fractured the teeth, examined them with scanning electron microscopes, and measured minerals using an energy dispersive spectrometer. All three preventive treatments protected the lesions, but the infiltration was no better than the sealant or -- more important -- the fluoride.
And even those who find the technique promising say there are challenges. Removing the surface zone of the lesion with hydrochloric acid is "tough," wrote the authors of the Caries Research article, "and for that particular reason alone, the adjacent teeth and surrounding soft tissues need to be protected, for example, by rubber dam."
They also noted that the resin used is sensitive to saliva. They recommended "modern clinical equipment" and said that one person can't perform the procedure unassisted.
To these cautions, Dr. Berg added that it remains to be seen how long the infiltrations will last once they're placed. But after reviewing the literature as a whole, he was encouraged.
"I think it's a useful product," he said.
Copyright © 2010 DrBicuspid.com