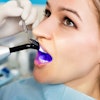
If you offer teeth whitening in your practice, you're probably concerned about both the cosmetic result and keeping your patients' teeth and gums healthy.
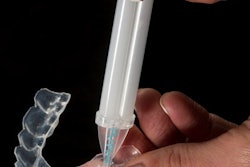
Teeth bleaching is a popular method for both in-office and at-home teeth whitening, but researchers from Brazil wanted to know if the chemicals involved would damage the dental pulp of patients. Their study in the Journal of Applied Oral Science investigated using both in-office and at-home bleaching processes.
"Tooth bleaching is a technique of choice to obtain a harmonious smile, but bleaching agents may damage the dental pulp," the authors wrote (J Appl Oral Sci, September-October 2016, Vol. 24:5, pp. 509-517).
Inflammatory measurements
Teeth bleaching is generally considered a conservative and effective technique, but the pulp's inflammatory response should be better understood before a bleaching technique is used clinically, the researchers noted. They measured inflammatory events and cells involved in the human pulp response to at-home and in-office bleaching.
The study included 29 human pulps from caries-free third molars from healthy patients (mean age of 23.5 years). The researchers divided them into three groups:
“Findings suggest that bleaching techniques should be carefully selected and that this treatment should be selectively indicated.”
- Control -- no teeth bleaching (CG) (n = 7)
- At-home bleaching with 15% carbamide peroxide (AH) (n = 10)
- In-office bleaching with 38% hydrogen peroxide (IO) (n=12)
The pulps were stained for microscopic analysis of inflammation intensity, collagen degradation, and pulp tissue organization.
The researchers found that in-office bleaching with 38% hydrogen peroxide had "more intense inflammation, higher macrophages migration, and greater pulp damage" than the carbamide peroxide group. They noted, however, that these techniques did not induce migration of mast cells and actually increased the number of blood vessels.
The in-office group had the highest number of pulp samples with moderate or severe inflammation (scores 1 or 2), whereas a large majority of the samples in the at-home group had no inflammatory infiltrate. See results in the table below.
| Intensity of inflammation after teeth bleaching | |||
| No inflammation | Moderate inflammation | Severe Inflammation | |
| Control group (n = 7) |
7 (100%) | 0 (0%) | 0 (0%) |
| At-home group (n = 10) |
8 (80%) | 2 (20%) | 0 (0%) |
| In-office group (n = 12) |
3 (25%) | 8 (67%) | 1 (8%) |
Careful selection needed
The authors cited several possible limitations to their study, including the following:
- The mechanical method of dental pulp removal may have "disorganized the odontoblastic layer of all pulps" and affected the evaluation.
- The thickness of the enamel-dentin of the third molars may reflect less inflammation and damage than teeth with thinner enamel and dentin.
- Teeth were extracted seven days after bleaching, which may impact the intensity of the inflammation, the authors noted. They recommended that future clinical trials include teeth extracted at different time intervals.
"The clinical relevance of this study lies in the fact that findings suggest that bleaching techniques should be carefully selected and that this treatment should be selectively indicated, since mild to moderate short-term changes were found in third molars that underwent in-office bleaching," the authors concluded.