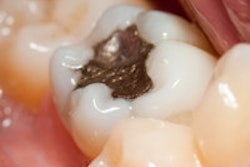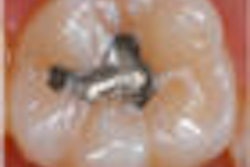
There's a pervasive problem in restorative dentistry, according to a new study in the Journal of the American Dental Association (July 2011, Vol. 142:7, pp. 842-849): Too many dentists are replacing amalgam restorations when a repair may suffice, and therefore practices have patients spending more money while limiting the life span of their teeth.
The seven-year clinical study, conducted at the University of Florida College of Dentistry, found that repairing amalgam restorations can be less costly and equally effective as replacements. These results could impact a pattern of overtreatment occurring in dentistry today, the lead author told DrBicuspid.com.
“The longevity result alone makes a strong argument to consider repair as a routine treatment.”
— Valeria Gordan, DDS, University
of Florida
"The presence of defective restorations is one of the most frequent problems encountered by general practitioners today, and, too often, dentists replace restorations that could have been treated differently," said Valeria Gordan, DDS, MS, a principal investigator at the College of Dentistry and lead author of the prospective longitudinal cohort study. "The repair treatment remained stable over a seven-year observation period. Just the longevity result alone makes a strong argument to consider this option as a routine treatment."
Amalgam replacement also results in a significant loss of tooth structure, which has a long-term impact on the tooth, she added.
"There are several reports in the literature that refers to the ‘rerestoration cycle' or ‘cycle of rerestoration,' which means that the tooth has a lifetime that starts with the first restoration, and, depending on when that first restoration takes place, it's going to dictate more or less the end of this tooth," Dr. Gordan explained.
Evaluating repair effectiveness
Possible options for treating defective amalgam restorations include repairing, sealing, refinishing, and replacement, Dr. Gordan and her colleagues noted. Repairing involves removal of the part of the restoration that is defective, as well as any affected tissue adjacent to the defective restoration. Sealing consists of applying a resin-based sealant on the defective site or margin. Refinishing consists of using finishing burs to remove surface defects or excess amalgam from restorations. Replacement entails removal of the entire restoration and placement of a new restoration.
To assess restoration repair effectiveness, Dr. Gordan and her team observed the longevity of amalgam restorations in 50 patients ranging in age from 21 to 77 with 113 total defective amalgam restorations on posterior teeth. Each restoration was assigned to one of five treatment groups:
- 25 received no treatment.
- 20 were repaired with amalgam.
- 23 had a resin-based sealant applied.
- 23 were refinished.
- 22 were replaced.
47 teeth were randomly assigned to the replacement and no treatment groups for comparison with the other treatment groups.
In the repair group, the clinicians removed the amalgam at the defective site with a carbide bur to allow for a proper diagnosis and an evaluation of the extent of the defect. Provided that the defect was limited and localized, the clinicians removed any defective tooth tissue, then roughened the amalgam surface with a diamond bur and repaired the restoration with a dispersed-phased amalgam.
In the resin-based sealant group, restorations with a crevice or a "ditch" at the cavosurface margin received a resin-based sealant after the clinicians performed acid etching with 34% phosphoric acid for 15 seconds. The clinicians then polymerized the sealant with a light-curing unit.
For refinishing, the clinicians used carbide burs to remove defective areas of the restorations that contained excess amalgam and silicone-impregnated rubber points to polish the occlusal and buccolingual surfaces of the restorations.
In the replacement group, they removed and replaced the defective restorations with a dispersed-phased amalgam. They did not use any bonding agent or liner underneath the amalgam restorations. In the no-treatment group, they examined the restorations visually but did not perform any treatment in the defective area.
Before and after a particular treatment was administered, two clinicians examined each restoration using modified U.S. Public Health Service criteria: occlusal and proximal marginal adaptation, occlusal and proximal anatomical form, occlusal and proximal contact, postoperative sensitivity, and secondary caries. Recall visits took place one, two, and seven years after the initial treatment, and three evaluations were performed at each follow-up visit.
Big-picture advantages
Of the original 113 restorations, 94 were observed after one year, 74 after two years, and 54 after seven years. The researchers examined the data in two ways to minimize attrition bias. In the first, they analyzed the teeth that had returned during the seven-year recall and the restorations that had downgraded or failed at the two-year mark with the assumption that downgrades would remain downgrades.
The second analysis was the same, but they excluded the restorations that had received a downgrade at the two-year recall. While some patients had multiple restorations, the researchers found that there was no relationship between this factor and the final outcome.
At the seven-year mark, no significant failure rate was observed across all treatment groups, while some degradation occurred in all of them, the researchers noted. Of the repaired restorations, 13 received an upgrade or had no change, 1 received a downgrade, and none failed. Of the replacement restorations, 12 received an upgrade, 5 received a downgrade, and 2 failed.
These results indicate that repair is an alternative to replacement for defective restorations, Dr. Gordan and her team concluded.
"When other factors are considered during the removal of existing restorations -- such as stress on the tooth, postoperative sensitivity, and re-exposure of the dentinal tubules with possible pulp dentin reaction to thermal or mechanical stimulus -- it makes perfect sense to pursue the repair of defective restorations as a predictable and conservative approach to preserving tooth structure," she said.
Dr. Gordan also sees big-picture advantages to a shift in dentistry's approach to defective restorations.
"These restorations can be completed more quickly and with lower operational costs," she said. "Therefore, repaired restorations could present a reduction in patient and/or the third-party payors' cost, which would make it possible for a higher number of individuals to afford dental care."
Dr. Gordan urges practitioners to only consider replacement if they cannot properly remove the affected defective area without removing the entire restoration.
"When the clinician is evaluating an existing restoration with one or more localized clinical features that deviate from ideal and the restoration is considered defective, the clinician should assess if the restoration in question can undoubtedly benefit from a new restoration," she explained. "If he or she is faced with a borderline situation, the best approach would be to assess the patient's past dental history and current caries risk status, and consider the best alternative treatment for the tooth in question."