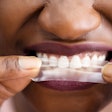
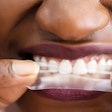
Sugar-free chewing gum has been associated increasingly with oral benefits such as fighting caries. Now a new study has found that using sugar-free chewing gum after whitening could reduce the intensity of tooth sensitivity following in-office procedures (British Dental Journal, June 2010, Vol. 208:12, pp. 571-577).
Study authors Brian Tang, D.D.S., who runs a private practice in Mountain View, CA, and Brian Millar, Ph.D., a professor at King's College London Dental Institute, wanted to determine if chewing sugar-free gum containing Recaldent (casein phosphopeptides and amorphous calcium phosphate [CPP-ACP]) could reduce the incidence, duration, and intensity of whitening-induced tooth sensitivity.
“Think of it as Lamaze technique for the teeth.”
— Van Haywood, D.M.D.
The findings might provide supporting evidence for a simple and cost-effective treatment modality that could enhance patients' comfort in the future, according to the researchers.
"To my knowledge, this is the only study that looks at the use of chewing gum for sensitivity relief," Dr. Tang said. "Most studies done on chewing gum focus on remineralization."
Dr. Tang decided to conduct the study after he tried sugar-free chewing gum for sensitivity relief postwhitening in his own office and found it effective. "I wanted to see if it would work clinically in a blinded study," he said.
A cost-effective treatment
Dr. Tang and his colleague looked at 88 patients who had their teeth whitened in a single in-office visit with 15% hydrogen peroxide augmented by light for a treatment period of one hour.
Following the procedure, each patient was randomly assigned to one of three study groups: group A used a sugar-free chewing gum with Recaldent, group B did not use any desensitizing agent, and group C used a sugar-free chewing gum without Recaldent.
The participants returned for a 24-hour follow-up visit where they completed a questionnaire regarding the incidence, duration, and intensity of tooth sensitivity.
Among the study findings:
- The majority of the participants (85.2%) reported sensitivity following the whitening procedures.
- On average, the sensitivity experienced by the subjects was relatively short-lived, with a mean of 4.9 hours and a range of 0 to 12 hours.
- The median intensity of sensitivity was notably higher among the subjects who did not use any desensitizing agent (group B) when compared to the other two groups who chewed sugar-free gums (groups A and C).
- The difference between group B and the other two groups was statistically significant; there was no statistically significant difference between group A and group C.
How gum relieves sensitivity
Dr. Tang and Millar offered various theories that could explain why both groups of gum users experienced less sensitivity. The reduced sensitivity could be a placebo response, or the distraction associated with gum chewing might provide some actual therapeutic effect above and beyond the placebo effect, they said.
"As a result of the strong psychological component of pain perception, supplemental use of nonpharmacological analgesic techniques can sometimes be effective," they wrote.
Also, chewing gum could increase stimulated salivary flow that may, in turn, reduce sensitivity.
"This study suggested that using a sugar-free chewing gum (both with and without CPP-ACP) could reduce the intensity of tooth sensitivity associated with in-office whitening procedures," the authors concluded. "However, it failed to demonstrate conclusively that using a sugar-free chewing gum with CPP-ACP could provide additional therapeutic benefits."
Dr. Tang said he was surprised that gum with Recaldent was not more effective in blocking sensitivity than regular sugar-free gum. He hypothesized that Recaldent could potentially provide a desensitizing effect through rapid protein binding deposition of calcium and phosphate ions within the exposed dentinal tubules.
One possible reason Recaldent gum was not more effective could be the relatively low concentration in the chewing gum that they used (0.6% in Trident White [Cadbury Adams USA] versus 10% in MI Paste [GC America]), he noted.
Chewing is the key
ACP did not help with sensitivity because it is primarily a tubular blocker, and the bleaching sensitivity comes from the easy passage of material through the tooth, not the tubules, said Van Haywood, D.M.D., a professor of oral rehabilitation at the Medical College of Georgia School of Dentistry who has also done research on bleaching sensitivity (Quintessence International, February 2001, Vol. 32:2, pp. 105-109).
"Its primary use is remineralization," he told DrBicuspid.com. "Any help with sensitivity is minimal if true, and no studies really show that happens."
While this was an interesting study, he added, what was demonstrated was that chewing reduces pain or awareness of sensitivity.
"Think of it as Lamaze technique for the teeth, sort of a distraction from the sensitivity," Dr. Haywood said. "I don't think there is any validity of ACP in chewing gum making a difference, which is what this paper shows."
It would have helped if group B had chewed a piece of leather or some inert material, he added.
"If you don't chew, you would be more aware of the sensitivity," Dr. Haywood concluded.
Dr. Tang suggested that dentists could keep a copy of this study in their office to offer as evidence that chewing gum can help relieve sensitivity and hand out gum samples after whitening.
"Even though gum works well by itself, it can also be used as a cheap, accessible adjunct treatment along with fluoride and potassium nitrate," he said, adding that follow-up studies with more patients and higher Recaldent dosages are needed.
Copyright © 2010 DrBicuspid.com