Dental professionals should vigilantly pursue proper diagnosis and management of problems associated with upper airway breathing passages to ensure that the brains of younger patients receive adequate oxygenation, a sleep apnea expert urged at the recent Rocky Mountain Dental Convention in Colorado.
Over the past 20 years, the research community has come to realize the importance of proper sleep in childhood and adolescence, said Dennis Bailey, DDS, a practicing dentist in Greenwood Village, CO, who has more than 25 years of experience in the use of oral appliances to manage snoring and sleep apnea and more than 30 years of experience in temporomandibular disorders, orofacial pain, and orthodontics.
“If you breathe through your mouth, all bets
are off.”
— Dennis Bailey, DDS
Heightened awareness of the topic has been marked by a 1,226% increase in articles on obstructive sleep apnea (OSA) and other sleep disorders, he noted. Accompanying this statistic is an incidence of about 7% of children and adolescents suffering from sleep-related breathing disorders.
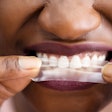
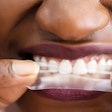
Nighttime mouth breathing stands as the most problematic, Dr. Bailey said, because it contributes to difficulties such as neurocognitive development, enuresis (bedwetting), poor academic performance, and alterations in craniofacial growth.
"What you're going to find out is that if you breathe through your mouth, all bets are off," he told his audience. "Breathing during the day is not the same as it is at night. That goes for children, adolescents, adults, and infants. I cannot stress to you enough how deleterious and how damaging mouth breathing is."
Why is it so dangerous? "Because the nose is the body's carburetor," Dr. Bailey said. "Every one of us in this world has brains that require more oxygen at night than they do during the day. If you don't get that oxygen to the brain during the nighttime, what happens is that a host of neurochemicals are not being produced properly by the brain. It leads to depression, it leads to developmental problems, and it leads to things like ADHD [attention-deficit/hyperactivity disorder]."
An oral rather than a nasal orientation to breathing can actually foment a cascade of damaging events, he noted. Mouth breathing leads to compromises associated with poor breathing habits during sleep. These in turn lead to snoring, which can then lead to upper airway resistance syndrome (UARS), or labored breathing. UARS occurs when muscles of the airway become relaxed during sleep, reducing the diameter of the airway.
To properly diagnose and mitigate these complications, the nasal and oral airways should be considered individually in all patients -- especially younger ones, according to Dr. Bailey.
"We need to look for altered breathing patterns -- mouth or nose," he emphasized. "Find out if that child or adolescent is a mouth breather at night, and if they are a mouth breather at night, start looking for causes, such as allergies, nasal airway obstructions, or enlarged tonsils."
Dr. Bailey also recommended looking for signs of sleep deprivation in younger patients' behavior, such as reduced attention span, sleepiness, and snoring.
"Do they have headaches? Pain? Ear and throat infections? Is their growth and development not on par? Do they have narrow dental arches? High palettes? Malocclusions?" he said. "All of these things are foreboding signs that that child is at risk for a sleep breathing disorder because these are the outcomes that can occur."
Dentists can help manage sleep-related disorders with sinus rinses and palatal expansion for improvement of nasal airway patency, he said. At minimum, Dr. Bailey suggested, the dentist should work with the patient to complete a pediatric sleep questionnaire.
Copyright © 2011 DrBicuspid.com