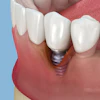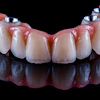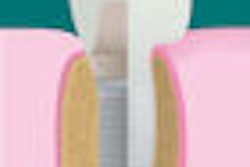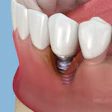
Immediate implant placement and provisionalization in the aesthetic zone results in excellent short-term treatment outcomes for survival and also minimal change of peri-implant soft- and hard-tissue dimensions, according to a new study in the Journal of Periodontology (February 6, 2014).
Single-tooth implant placement in the aesthetic zone is a highly reliable treatment option, but, recently, research interest has shifted away from implant survival after this procedure to optimal preservation of soft and hard tissue, as well as aesthetic outcomes, the study authors wrote.
“The patient immediately benefits from this treatment.”
In this latest study, the researchers assessed the condition of implant survival, peri-implant soft- and hard-tissue changes, and aesthetic outcome, as well as patient satisfaction after immediate placement.
The current literature lacks a complete overview of immediate implant placement of a single tooth in the aesthetic zone, according to lead author Kirsten Slagter, DDS, from the department of oral and maxillofacial surgery at the University Medical Center Groningen in the Netherlands. "Other reviews only look at survival, marginal bone loss, or soft-tissue changes, but in this review all the different aspects are taken into account," she said in an interview with DrBicuspid.com.
The researchers searched Medline, Embase, and Central databases for studies published up to June 2013, and found 993, 273, and 130 hits, respectively. All studies of immediate implant placement of a single tooth in the aesthetic zone that met the search criteria were included in the study.
The current study included prospective studies with a follow-up period of at least one year or observational studies with implants placed in the aesthetic zone with a follow-up of at least a year. The researchers also considered case reports that evaluated more than 10 cases. They included 34 studies in their final analysis.
The researchers defined the aesthetic zone as from the second premolar to the second premolar. They defined immediate placement as an implant placed immediately after an extraction. They required that the included study reported implant survival, marginal peri-implant bone level change, change on peri-implant soft tissue, or aesthetic outcome. The researchers then did a pooled analysis to identify factors associated with survival and peri-implant tissue changes.
"To our knowledge this is the first pooled analysis," Dr. Slagter said. "By doing a pooled analysis, all immediately placed implants in the aesthetic zone could be analyzed in all the different available studies."
Of the 34 studies, the researchers analyzed a total of 985 implants in 979 patients. Median patient age was 46 years, median follow-up period was 18 months, and 76% of the patients underwent immediate provisionalization.
Dr. Slagter noted that all the outcome variables of the implants in the studies were placed in a database, and with a total 985 implants, they got a good indication of the average values.
The researchers found that the survival rate of immediately placed single-tooth implants was 97.1%, as 956 of the 985 implants considered in the study survived.
The mean marginal peri-implant bone loss was 0.81 ± 0.48 mm, mean loss of interproximal peri-implant mucosa level was 0.38 ± 0.23 mm, and mean loss of peri-implant midfacial mucosa level was 0.54 ± 0.39 mm.
Also, delayed provisionalization, use of a flap, and use of a connective tissue graft were associated with marginal peri-implant bone level change of greater than 0.50 mm.
For aesthetic indexes and patient satisfaction, the authors tried to analyze these aspects but due to underreporting, no analysis could be done.
The study authors noted that the survival of immediately placed implants after a one-year follow-up was excellent and comparable with previously published survival rates. Also, the timing of provisionalization was not associated with outcome in terms of implants survival and were not inferior to those of delayed provisionalization.
"Dentists in everyday practice who are not sure whether to use immediate provisionalization or delayed after immediate implant placement know now that it is not associated with survival," Dr. Slagter said.
She added that immediate provisionalization is not even a risk factor for marginal bone loss, since the change was less than 0.5 mm. Also, micromotion is possibly not as important as previously thought.
"The use of a flap and connective tissue graft should be avoided, because it is associated with marginal bone level change of more than 0.5 mm," Dr. Slagter said. "The mean calculated marginal bone loss is in line with other studies, as well as the calculated interproximal mucosa level and midfacial mucosa level."
The authors did note, however, that the postoperative surgical site is not always suitable for immediate placement, and there are certain clinical conditions in which it is not an optimal treatment option. For example, it is not recommended in the case of severally inflamed areas or medically compromised patients. In these cases, a flap or connective tissue graft can be used, or special precautions need to be taken.
They also noted that since patient satisfaction is an important current issue, aesthetic indexes and patient satisfaction scales need to be applied in future studies that assess treatment outcomes.
"Immediate placement and provisionalization in the aesthetic zone has some important advantages, and the patient immediately benefits from this treatment, which can substantially have a positive impact on their quality of life," Dr. Slagter concluded.