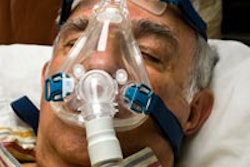
SAN FRANCISCO - In a presentation at the California Dental Association's CDA Presents conference, Steve Carstensen, DDS, of Bellevue, WA, spoke on the importance of recognizing sleep apnea in patients who may not know they suffer from it.
"You have to realize you have a responsibility to get the ball rolling in recognizing patients who may have sleep apnea," Dr. Carstensen told a capacity audience.
He noted that a patient who "just snores" after a few alcoholic drinks or a patient who has put on some weight could be at risk for sleep apnea, which may lead to other issues, such as cardiovascular problems, depression, diabetes, and other conditions.
“You have to realize you have a responsibility to get the ball rolling in recognizing patients who may have sleep apnea.”
Many dental offices are not aware of how widespread obstructive sleep apnea (OSA) can be, Dr. Carstensen said. About 80% of patients with drug-resistant hypertension and the same number of those with congestive heart failure have OSA, he noted in his presentation. Studies have also shown that more than 70% of those patients with type 2 diabetes have OSA, and 70% of patients with orofacial pain have some sort of sleep disorder, he added.
A patient's neck size also can be a predictor, Dr. Carstensen said. His quick guide is that if female patients have a neck size larger than 15 inches and male patients have a neck size greater than 17 inches, they are at risk for sleep apnea.
He then posed the question of how the different categories of sleep apnea were defined. Obstructive apnea is the absence of airflow despite persistent effort; central apnea is the absence of airflow because of a lack of effort; and mixed apnea is a combination of the two.
Dr. Carstensen suggested that practices begin using a risk assessment, if they don't already have one in place. The risk assessment for sleep apnea should be part of a routine patient history and doesn't add much time to a patient visit, he said.
The risk assessment includes blood pressure monitoring at each visit, asking questions about quality of sleep, looking for any risk signs of sleep apnea, and also asking patients if they are aware of sleep apnea risks and consequences.
As other studies have noted, the use of the STOP-Bang sleep apnea questionnaire (snoring, tiredness, observed stop breathing, blood pressure, body mass index [BMI], age, neck circumference, and gender) is effective. Male gender is a risk, along with age older than 50 and a BMI greater than 35, he said.
Dr. Carstensen then discussed treatments, such as oral appliance therapy (OAT). Patient selection for oral appliance therapy is important, he said. Choosing patients who are not obese, who have mild to moderate OSA, and those with "mild" anatomic problems is important, he noted, stating that those with severe anatomic problems may not benefit from OAT.
Oral appliance therapy works by opening the pharynx by protruding the mandible, he said. The passive stretch of soft tissue "lifts the base of the patient's tongue" and stiffens their palate. The dentist would need excellent impressions and protrusive bite recordings, he noted. Appliance categories include custom appliance, a tongue repositioning device (TRD), boil-n-bite, and others.
There can be complications, such as jaw muscle pain, drooling, tooth sensations, and tongue tenderness, Dr. Carstensen cautioned. He also asked, "How do you know if the therapy is working?" By further lab tests and by patient and bed partner assessments was his answer.
He concluded his presentation by noting that the coding for such treatment isn't similar to dental insurance. It is medical insurance, and he listed diagnosis and procedure codes.