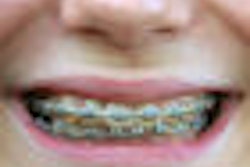
With access to care and healthcare reform such hot-button issues these days, a recent study in the Journal of the American Dental Association highlights another underserved population U.S. policymakers should give more consideration: Medicaid patients with malocclusion (JADA, October 2010, Vol. 141:10, pp. 1202-1212).
Noting that patients enrolled in Medicaid have limited access to orthodontic services in the U.S. but that no studies have fully assessed the clinical, economic, and psychosocial burdens on these patients, researchers from the University of Washington conducted a systematic review of the relevant economic literature.
“Ortho treatments typically run at about 50% overhead, and Medicaid runs at about 50% of
the cost.”
— Steve Dickens, DDS, MS
"Treatment of malocclusion has become common in the U.S. because patients generally believe that it provides significant long-term benefits in quality of life and overall oral health," they wrote. "Despite this, rates of untreated malocclusion remain high among children who are socially disadvantages (for example, racial/ethnic minorities, immigrants from lower-income families, and those living in rural communities), resulting in a substantial oral health burden."
These children have limited access to orthodontic services because of their families' competing needs for limited resources and also because of the limited availability of orthodontists in their communities and a shortage of orthodontists who are willing to treat patients enrolled in Medicaid, the researchers added.
Economic lit review
To assess the economic literature pertaining to the costs and burdens associated with malocclusion, two of the researchers did keyword searches on PubMed, Google Scholar, Medscape, the National Health Service Economic Evaluation Database, and ScienceDirect. Their searches involved these keywords: malocclusion, cost, cost-effectiveness, occlusion, Medicaid, and orthodontics. They grouped the terms together in various forms and reviewed the resulting list of article titles and abstracts to determine their relevance for the population of interest (children in Medicaid).
The researchers determined that 15 articles met their criteria for cost-effectiveness of orthodontic care or malocclusion. Of these, they chose eight for the JADA review.
They found that several U.S. studies have evaluated Medicaid reimbursement with regard to malocclusion, including one that found that men, blacks, Hispanics, and children from low-income families were less likely to receive care despite their clinical need (Journal of Public Health Dentistry, Winter 2007, Vol. 67:1, pp. 20-27), while another found that Medicaid patients and those who had private insurance experienced similar malocclusion improvement following early orthodontic treatment (American Journal of Orthodontics and Dentofacial Orthopedics, May 2005, Vol. 127:5, pp. 592-598).
Using this information, the authors then developed a conceptual framework that could be used to evaluate the costs and effects of treating or not treating malocclusion in Medicaid patients.
"Our model framework provides one representation of treatment decisions related to malocclusion, although there may be other ways for healthcare providers and families to evaluate these issues," they wrote. "We would expect their choices to be influenced by the coverage and reimbursement policies of the Medicaid programs in their state."
For example, they suggested, orthodontists in private practice and professional organization could introduce solutions such as shorter treatment time to reduce the clinical, psychological, and economic burden of malocclusion on low-income patients.
"Third-party payers are searching for methods to improve the value delivered for the reimbursed dollar," the authors wrote. "Strategies that motivate patients to make stronger commitments to their treatment plans ... may help generate improved dental care outcomes and provide more cost-effective solutions. Such strategies also may persuade more orthodontists to become Medicaid providers."
Compliance and reimbursement rates
The JADA review was interesting and well-done, noted Steve Dickens, DDS, MS, a former professor at the University of North Carolina who has conducted related research, including one of the eight studies cited in the JADA article (Journal of Public Health Dentistry, Summer 2008, Vol. 68:3, pp. 167-169).
"This was a tough review to do because there is not a lot of information about the cost or burden of malocclusion for people who can't afford treatment," he told DrBicuspid.com. "There are no real numbers for the cost of severity of malocclusion that goes untreated and what it would cost society to fix that."
One of the key sticking points when it comes to providing orthodontic care to Medicaid patients is the reimbursement rate, he added. In fact, the JADA authors addressed this issue directly in their analysis of state-by-state Medicaid policies and the effect these policies have on practitioners' treatment decisions:
"Orthodontists have conflicting incentives regarding treating low-income patients with malocclusion and must balance economic and clinical decisions," they wrote. "As dental care providers they want to provide high-quality care and reduce the burden associated with oral conditions. However, they generally are in private practice (versus public clinics) and must take into consideration practice management expenses. Therefore, restrictive Medicaid reimbursement policies may not provide a sufficient incentive for clinicians to administer the highest quality, most resource-intensive care and sometimes may limit clinically appropriate care."
Dr. Dickens, who is now back in private orthodontic practice, agreed. "Practitioners see the fee for reimbursement as a real barrier," he said. "There is also the perception that Medicaid patients are less compliant. And some practitioners feel they don't want to mix Medicaid population with their fee-for-service population in the waiting room."
One of the findings of Dr. Dickens' 2008 study, however, was that there were no differences in compliance between Medicaid and fee-for-service patients. In the long run, he said, orthodontists would be more inclined to provide more care to Medicaid patients if the incentives were improved.
"I definitely think that increasing the reimbursement rate would break down the major barrier for practitioners to treat Medicaid patients," he said. "Ortho treatments typically run at about 50% overhead, and Medicaid runs at about 50% of the cost. So you don't really make money treating Medicaid patients unless you have volume. However, if the volume goes up, generally the quality goes down. But if they would increase the rate you are reimbursed, it would increase the number of Medicaid patients treated."
Copyright © 2010 DrBicuspid.com