Post-treatment apical periodontitis and endodontic treatment failure may be associated with factors such as intraradicular and extraradicular infections, according to a study recently published in the Journal of Endodontics.
Additionally, granuloma was identified as the most common histopathological diagnosis among post-treatment lesions, the authors wrote.
“The primary cause of posttreatment disease is bacterial infection in or outside the root canal system,” wrote the authors, led by Dr. Andrea F. Campello, PhD, of Iguaçu University in Brazil (J Endod, March 20, 2026).
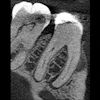
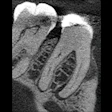
The study analyzed the histobacteriological and histopathological features of biopsy specimens from teeth with post-treatment apical periodontitis. The sample included 71 biopsy specimens from root canal-treated teeth, collected from 71 patients with an average age of 37. Specimens consisted of root tips with attached lesions obtained during periradicular surgery or tooth extraction.
Furthermore, all cases were considered treatment or retreatment failures due to persistent, worsening, or newly developed lesions, or the presence of clinical signs and symptoms after at least one year of follow-up. The analyses evaluated intraradicular and extraradicular infections; inflammatory and epithelial changes; and classified lesions as abscesses, granulomas, or cysts, with further subtypes based on epithelial features and structural characteristics.
Intraradicular infection was identified as the primary factor associated with post-treatment apical periodontitis. Bacteria were detected in the apical root canal system in 94% of specimens, frequently forming biofilms in 79% of cases, with expansion into dentinal tubules and canal ramifications. Extraradicular infection occurred in 37% of cases and was almost always associated with a concurrent intraradicular infection.
Biofilms in the main apical canal were significantly more common in teeth with underfillings and inadequate root canal treatment (p < 0.05), while extraradicular infection was more often observed in symptomatic cases, sinus tracts, abscesses, large lesions, and retreatment cases (p < 0.05). Granuloma was the most common histopathological diagnosis, with nonepithelialized granulomas accounting for 42% of post-treatment apical periodontitis lesions.
However, it is possible that intra- or extraradicular bacteria were not detected due to limitations in the methods used, as similar oversights in earlier studies may have led to the assumption that post-treatment apical periodontitis had nonmicrobial causes.
“Intraradicular infection was the major factor associated with posttreatment apical periodontitis,” Campello and colleagues concluded.