Inserting gauze coated with an antibiotic-corticosteroid ointment into a wisdom tooth extraction site may control dry socket, infection, and pain. The findings come from a study published earlier this month in Oral Science International.
Filling the socket with gauze covered in oxytetracycline-hydrocortisone ointment resulted in an open wound, which inhibited bacterial growth and reduced postoperative infection and pain. Furthermore, Winter’s position classification, a method for the spatial assessment of impacted teeth, is suggested to be an independent prognostic factor for postoperative pain, the authors wrote.
“Our procedure both prevents the occurrence of dry socket and suppresses spontaneous post-extraction pain,” wrote the authors, led by Dr. Moriyasu Adachi of the department of oral and maxillofacial surgery at Shizuoka General Hospital in Japan (Oral Sci Int, June 15, 2023).
Common complications
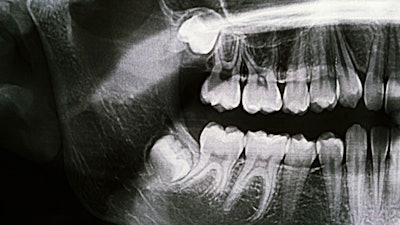
It’s not unusual for patients undergoing third-molar surgery of the lower jaw to experience dry socket, post-extraction pain, and infection. In the field of oral and maxillofacial surgery, dry socket is one of the most studied complications of extractions.
To try and suppress the occurrence of dry socket and postsurgical pain and infection, the gauze technique was used in 286 patients after they underwent mandibular third-molar extractions. Using this method, the incidence of dry socket and postsurgical infection after extraction was 1.05% (95% confidence interval [CI], 0.22% to 3.03%) and 0.35% (CI, 0.01% to 1.91%), respectively. These percentages are lower than previous reports of an approximate 30% incidence rate of dry socket and up to 6% incidence of postoperative infection.
Inserting the gauze covered in the ointment likely allowed the extraction socket to remain open, preventing bacteria from growing. Also, the antimicrobial effect of the tetracycline in the salve may have also helped prevent infection and associated pain, the authors wrote.
Additionally, the mean visual analog scale (VAS) for pain severity on the day of the extraction surgery was 4.15 (CI, 3.86 to 4.45). On postoperative day one, the VAS was 2.28 (CI, 2.05 to 2.50]. On postoperative day three, VAS was 1.40 (CI, 1.21 to 1.59); on postoperative day seven, it was 0.55 (CI, 0.41 to 0.68), according to the study.
In the regression tree analysis, the Winter position classification was the main predictive factor for having pain on postsurgical days one and seven. On postoperative day one, the VAS was predicted to be lower in Winter position classification A, which is a vertical impaction, than that of classification B or C, which are mesioangular and horizontal impactions, they wrote.
The study had several limitations. The bone condition of the extraction socket and poor oral hygiene were not analyzed as predictive factors for post-extraction complications, the authors acknowledged.
Future studies needed
Additionally, more research is needed, because this study did not compare the postoperative course of the gauze insertion group with that of a gauze-free group, they wrote.
“(Using gauze covered in ointment not only can result in a low incidence of dry socket and post-extraction infection and pain, but) “the Winter position classification was suggested to be an independent predictor of postoperative pain,” Adachi and colleagues wrote.