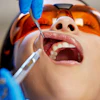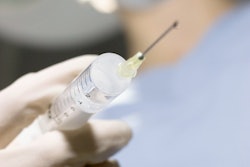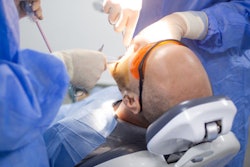
Remimazolam had a higher success rate in sedating patients undergoing outpatient oral surgery compared to midazolam, according to a study published on September 15 in the Journal of Oral and Maxillofacial Surgery.
Despite its ultrashort half-life, remimazolam required fewer additional doses, the authors wrote. The small study is believed to be the first to evaluate the sedation effects of remimazolam in outpatient oral surgery in relation to midazolam.
"It can be a new sedative option for outpatients undergoing ambulatory oral surgery," wrote the authors, led by Dr. Xudong Yang, PhD, of Peking University in Beijing.
Intravenous minimal and moderate sedation is widely used in patients to help them overcome dental anxiety. Midazolam is commonly used for sedation in outpatient procedures. But it's not without its disadvantages, including increased accumulation and respiratory depression.
On the other hand, remimazolam, a short-acting benzodiazepine, is rapidly distributed following administration, with a mean half-life of between 0.5 and two minutes. Its terminal half-life in plasma is 37 to 53 minutes. Remimazolam's clearance is not linked to body weight, and previous trials have shown no statistically significant differences in heart rate, oxygen saturation levels, or respiration rates.
To determine whether remimazolam can achieve the same sedation effects as midazolam, a prospective, randomized, controlled, single-center study of 40 patients undergoing ambulatory oral surgery procedures, including tooth extractions, was conducted. The patients were randomly and evenly divided into remimazolam and midazolam groups. The success rate of sedation, which was defined as completing the procedure without the use of rescue sedatives, was the primary outcome, according to the study.
Overall, the sedation success rate was 82.5%. When comparing the two sedatives, the remimazolam group had a sedation success rate of 95%, while midazolam had a rate of 70%, the authors wrote.
Also, there was a statistically significant difference in the median number of additional doses administered within five minutes between the midazolam patients and the remimazolam patients (0.82 vs. 0.51, p = 0.006), they wrote.
The study had limitations, including its small sample size. The results must be validated in a wider area, the authors noted.
"(Nevertheless), the use of remimazolam is effective for sedation of patients undergoing ambulatory oral surgery," Yang et al wrote.