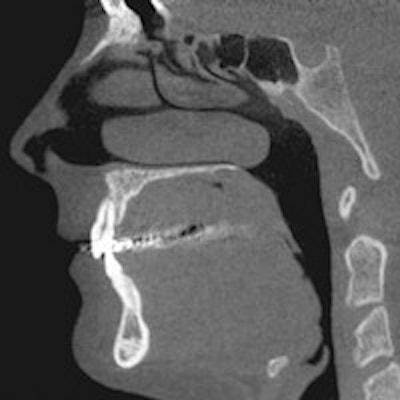
Although cone-beam CT (CBCT) has been around for almost 20 years and is often used for implant planning, cases of impacted teeth and trauma, periapical diagnosis, and more, it is well known that it delivers a radiation dose higher than conventional dental radiography.
Many CBCT systems are currently available, and features, radiation doses, and image quality varies among them. The authors of a new study in Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology recognized the clinical need to limit radiation exposure while maintaining image quality (March 2015, Vol. 119:3, pp. 357-365). They sought to assess image quality by using a standardized method for the optimization of these different devices.
The researchers investigated the relationship between physical factors and subjective image quality, and they also attempted to assess the differences in the required physical image quality according to diagnostic tasks. They found that, when using CBCT, it is important for the practitioner to consider the diagnostic job to be completed when evaluating the image and image quality.
The researchers, led by Jin-Woo Choi, DDS, of the department of oral and maxillofacial radiology in the College of Dentistry at Dankook University in Seoul, South Korea, collected CBCT images of a real skull phantom and a SedentexCT IQ phantom under different exposure conditions using a Dinnova3 CBCT scanner (HDXWILL) at 60-110 kV and 4-10 mA.
After the images were obtained and stored, radiologists were asked to judge the image quality and categorize it as either acceptable or unacceptable. The researchers also measured the modulation transfer function (MTF), contrast-to-noise ratio (CNR), and image uniformity using the SedentexCT IQ phantom images. They also evaluated any differences in physical factors.
Results
Images of the SedentexCT IQ phantom were acquired under 24-exposure combinations to measure the physical factors of each image. A total of 640 slices of an axial image were loaded under each exposure condition. Suitable inserts for each physical measurement were selected manually. All image factors were measured repeatedly for reliability: 10 times in the MTF measurement and three times in the other measurements.
In the maxilla, MTF and CNR values showed no significant differences between periapical diagnosis and implant planning in the acceptable groups. Higher MTF and CNR values were required in the periapical diagnosis compared with the implant planning of the mandible.
However, the researchers found significant differences in the MTF values between clinically acceptable and unacceptable images in all tasks. The authors cautioned that this does not prove the usefulness of the MTF as the cut-off value of MTF 10 was low and the success of a diagnostic task often depends on small differences of spatial resolution.
While CBCT in dentistry is mainly used for high-contrast anatomic structures (such as tooth and bone lesions), the periodontal ligament space and lamina dura (which have relatively low contrast compared with trabecular bone) also should be clearly depicted in any image, as they are important anatomic structures, the study authors noted.
In the case of the mandible, the periapical diagnosis required better physical image quality compared with implant planning, they added. The study "proved that MTF and CNR values have a significant association with subjective image quality," the authors concluded, and they recommended that the diagnostic task be considered in evaluation of CBCT image quality.