Periodontal health has again been linked to kidney health in two new studies presented at the recent 2018 International Association of Dental Research (IADR) meeting in London. The studies found a significant association between chronic kidney disease and signs of poor periodontal health.
 Jacopo Buti, DDS, PhD.
Jacopo Buti, DDS, PhD.In one study, periodontal inflammation was associated with a decrease in kidney function, and in the other, patients with worse clinical attachment levels (CAL) were significantly more likely to have worse kidney function in the future. The research adds to the growing body of research that demonstrates the intricate relationship between oral and systemic health.
"Poor oral health -- and particularly destructive periodontitis -- is associated with poor prognostic factors in chronic kidney disease patients, including malnutrition and inflammation, and may predict progressive kidney disease," one IADR presenter, Jacopo Buti, DDS, PhD, senior clinical lecturer of restorative dental sciences at Eastman Dental Institute in London, told DrBicuspid.com. "Periodontal diseases have also been linked to systemic adverse outcomes in patients with other comorbidities, including diabetes and cardiovascular diseases."
Perio inflammation and systemic inflammation
Chronic kidney disease affects millions of people and is the ninth leading cause of death in the U.S. Previous research has linked chronic kidney disease to heart disease through systemic inflammation and oxidative stress. Therefore, researchers from the U.K., including IADR presenter Praveen Sharma, BDS, were curious whether those factors would also link kidney disease to periodontal disease.
 Praveen Sharma, BDS.
Praveen Sharma, BDS.To find out, Dr. Sharma and colleagues recruited 770 patients with stage 3 to stage 5 predialysis chronic kidney disease. They measured periodontal inflammation using the periodontal inflamed surface area (PISA) score and kidney function using estimated glomerular filtration rate (eGFR), a test that measures how well the kidneys are working.
The researchers found that a 10% increase in PISA score equated to a 2.5% decrease in eGFR, suggesting that periodontal inflammation indirectly affected kidney health.
"One of the ways that periodontal inflammation might affect renal function is by influencing 'factors' in the blood that then get transported to the kidneys," said Dr. Sharma, a clinical lecturer at the University of Birmingham School of Dentistry in Birmingham, U.K.. "That is an assumption we tested, and we found that the assumption that periodontal inflammation influences oxidative stress, stress on a cellular level, which in turn affects renal function."
It is important to note, however, that PISA score did not have a significant, direct effect on eGFR, nor was there a direct or indirect effect of eGFR on PISA score. Nevertheless, the findings call for further study.
"We are undertaking a pilot study to see if treating periodontitis in patients with kidney disease influences their cardiorenal health," Dr. Sharma said. "In addition, our team in Birmingham will also be following up a cohort of patients with kidney disease to see if renal function declines more in patients with periodontitis than those without."
CAL and kidney health
Meanwhile, Dr. Buti and another team of U.K. researchers investigated how dental and periodontal health metrics related to eGFR using data from almost 200 participants with stage 3 to stage 5 kidney disease. All study participants were recruited to the renal unit of the Royal Free Hospital in London between September 2003 and August 2007 for a study on kidney health and cardiovascular disease.
At the outset of the study, a single dental examiner completed full dental and periodontal assessment that included recordings of clinical attachment level (CAL), plaque index, bleeding score, and decayed, missing, and filled teeth score. The eGFR of the patients was then monitored over the course of five years.
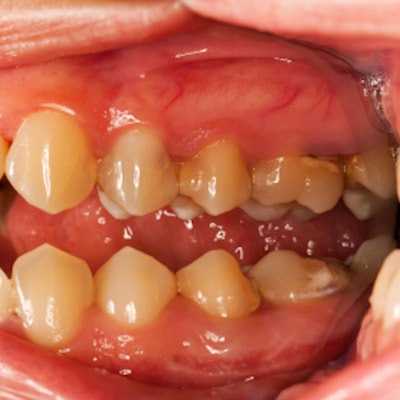
The researchers found that patients with chronic kidney disease presented with substantial oral health treatment needs and that the vast majority (89%) had moderate to severe periodontitis.
Furthermore, eGFR scores were significantly associated with CAL measurements at the outset of the study, and poor periodontal health metrics at the beginning predicted decreased kidney function in the future. However, the researchers aren't exactly sure why this is.
"The mechanism of association is still under investigation," Dr. Buti said. "Bacterial dissemination as well as a state of chronic inflammation, endothelial dysfunction, and increased systolic blood pressure are all considered as plausible mechanisms linking periodontal diseases to other chronic disorders, including diabetes and chronic kidney disease."