Regular dental care may be able to significantly lower patients' stroke risk, according to a January 15 study published in the journal Stroke. This research furthers the scientific evidence that cardiovascular health is deeply connected to oral health.
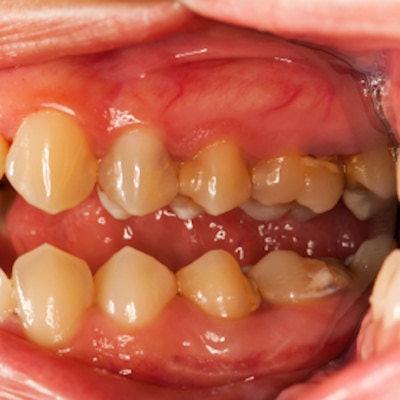
The study, which included thousands of U.S. adults, found a significant association between inflamed gums and ischemic stroke incidence. Inflammation may be the link between periodontal disease and stroke, and further studies are needed to better understand how dental treatment can reduce stroke risk, according to the researchers.
"Our findings show that periodontal disease is an independent risk factor of incident ischemic stroke," wrote the authors, led by Souvik Sen, MD, MPH, from the University of South Carolina School of Medicine in Columbia. "It is significant that the high gingival inflammation group ... likewise had an increased risk of ischemic stroke."
Stroke and gum disease linked by inflammation
Some small or observational studies have previously found that poor gum health is associated with an increase in stroke risk. However, long-term, population-based research on this topic is lacking in the U.S., where more than half of adults age 30 and older have periodontal disease, according to the study authors. Therefore, they decided to investigate the link between gum inflammation and stroke incidence using long-term data of U.S. adults.
The researchers used data from dental exams performed on more than 6,730 participants in the Atherosclerosis Risk in Communities (ARIC) study. The ARIC study enrolled more than 10,000 middle-aged adults in 1987 and 1989, then studied their long-term health outcomes through 2012.
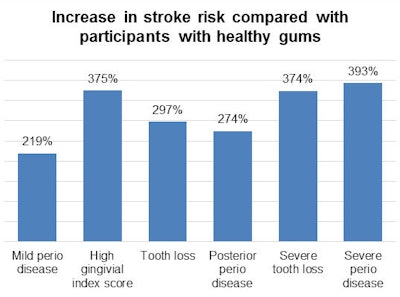
Participants with any form of periodontal disease, including mild periodontal disease, were significantly more likely to experience an ischemic stroke than those with healthy gums, according to the researchers. This was true even after adjusting for potential confounding variables, such as smoking status, education, diabetes incidence, and body mass index.
After further studying the results, they found that inflammation appeared to be the real driver between periodontal disease and stroke incidence. For instance, participants with high gingival inflammation but mild periodontal disease had at a higher risk for stroke than those with lower inflammation levels but more attachment loss.
"These data emphasize the importance of inflammation rather than just the level of attachment as being the main determinant of risk," the authors wrote.
The good news? Participants who visited the dentist at least once per year were significantly less likely to have periodontal disease and had a lower risk for ischemic stroke than those who only visited the dentist when they had a problem. Because of these findings, the authors suggested that regular dental visits may be able to lower stroke risk.
"To our knowledge, this would be the first U.S. study to report the independent role of regular dental care in prevention of incident ischemic stroke in a relatively elderly population," they wrote. "This is further validated by the fact that dental care was associated with lower burden of periodontal disease."
Tipping point
The authors acknowledged several study limitations, including only one periodontal assessment at the outset of the ARIC study and the lack of information on potential socioeconomic confounding variables, such as income and access to dental care.
However, they noted that their study is just the tipping point for research on the link between oral health and heart health, and future research on how to prevent stroke through dental and periodontal treatment is still ongoing and needed.
"The treatment of probing depth could plausibly reduce stroke incidence," the authors concluded. "The effect of probing depth treatment on recurrent vascular events in stroke/transient ischemic attack in patients is currently being investigated. ... Results may further help verify if periodontal treatment may reduce stroke risk."